BISC209:BootCamp
Lab 1 Microbiology Boot Camp
In this first lab you will learn:
- Who microbiologists are and what they do
- To learn aseptic technique so that you don't contaminate yourself or your cultures
- To begin to become familiar with some of the basic equipment and procedures used in microbiological investigation
- To use a lab notebook to record the progress of your experiments
- About the different habitats that you can choose among for your semester project
Introduction To Microbiology
Welcome to the unseen world of microorganisms. For most of us, microbes are out of sight and out of mind; largely, the human population would prefer it that way. However, since microbes have a major and continuing impact on us and on our planet, it behooves us to understand them better. By the end of this course, you will. Understanding the microbial world is a huge undertaking. A discipline that defines its scope as including all life forms (and some non-life forms like viruses and prions) that are invisible to the unaided human eye is a bit like saying we will study all humans and other animals shorter than 4 ft. Besides including a huge number of members, the diversity of such a group is overwhelming.
Where do we begin in the study of microbiology? It's good to start with appreciating the power of these tiny, unseen life forms to thrive and spread without our permission or knowledge. It is also wise to recognize that although a tiny fraction of the microbes in our world are disease causing, there are devastating infections caused by microbial pathogens. Although none of the microorganisms that we will knowingly work with this semester are commonly human pathogens, we require that you read and agree to certain rules for working in the microbiology lab that are designed to keep you from infecting yourself, your classmates, and the community. We will also begin today to learn aseptic techniques that will reduce the chance of contaminating your cultures or the chance that your cultures will contaminate you.
Lab Safety
Please download, read, and sign your agreement to follow the Wellesley College Microbiology Lab Safety regulations: Media:Wellesley_College_Lab Safety.doc. These regulations can be found in this lab wiki at:
BISC209/S10:ReadMe
If possible, watch these YouTube videos on lab safety at [1] and [2]
Introduction To the Tools and Techniques of Microbiology
Whether you are trying to keep a desired organism from being overgrown by a contaminant, or you are attempting to prevent contaminating yourself, your lab bench, or your lab partner with your cultures; awareness of potential sources of contamination in a microbiology lab is critical. Your success in the lab depends on being open to learning and adopting the standard procedures used in microbiology. Today you will practice aseptic transfer technique and immediately assess your success.
Aseptic transfer
Please watch the YouTube video on how to use the Bunsen burner [3] and broth to broth Aspetic transfer technique [4].
Aseptic transfer technique is important to prevent contamination of your cultures, yourself, others, and the laboratory. Manipulation of the many tubes, plates and transfer tools requires patience and practice and its mastery is vital to success in the microbiology laboratory. By the end of the semester you will become proficient at many of the transfer methods, you will know when and what to sterilize, and you will be able to keep pre-sterilized tools sterile.
After a demonstration by your instructor, you will practice the basics of aspetic transfer techniques and assess your success.
Activity 1: Practice Exercise on Aseptic Transfer:
1. Obtain and label a tube of water using a piece of your team color tape. Do not write directly on these non-disposable culture tubes with your Sharpie. Include on the label, your initials, date, Lab Section code (T or W), type of medium and organisms or id of inoculum.
Imagine that an organism is suspended in the stock tube (Tube A-found on your bench). Using Tube A and referring to the instructions for aseptic transfer (broth to broth), transfer a loopful of the contents of Tube A to a destination culture tube of water. (This first transfer is just for practice so you need not incubate this tube or save it for the next lab). Call your instructor over and ask her to assess your technique.
2. Label a destination nutrient agar plate with your initials, your lab section, the date, and the organism(s) or sample id. Always label on the AGAR side of plate. Why is it important to not label on the cover part of the plate? Cultures on solid media are usually incubated agar side up (covers down) to prevent condensation forming on the tops and then "raining" on your growing colonies, smearing them and making it more difficult to keep them separated--the goal. In addition if 2 or more plate covers fall off accidentally, you will be unable to match the cover to the correct plate.
Tube B contains a mixed culture of bacteria in nutrient broth: Serratia marsencens and Staphylococcus epidermidis. Mix the bacteria by "flicking" or with a GENTLE vortex (do NOT invert it as these caps are purposely not air tight). Flame sterilize your loop and then insert the loop portion into the broth in Tube B. Remove the loop from the broth culture and lightly touch and drag the contaminated loop across section 1 of the destination plate. Follow the remaining instructions for isolation streak technique.
Take the labeled plate you have inoculated to the designated rack for incubation at RT.
Come back to the lab in a few days to check on your cultures. You hope to see well isolated colonies (two different looking types) in the last zones of your streak plate.
The BISC209: Aseptic Transfer and BISC209: Streaking for Isolation protocol are found in the Protocols section of this wiki.
Bacterial Morphology
Background
The morphological characteristics of bacteria, including size, shape, and arrangement, can be seen by staining a bacterial smear so that individual bacterial cells are distinguished. For most species, morphologic characteristics are genetically determined and, thus, typical of the species. Generally, bacteria range in size from approximately 0.2 µm to 3.0 µm. The basic shapes are spherical (coccus), rod-shaped (bacillus), curved (vibrio), or helical (spirillum, spirochete). However, there are some species of bacteria that show considerable within species variation (termed pleomorphism). For example, both Mycoplasma (bacteria lacking the rigid cell wall of most bacteria) and Arthrobacter (a type of soil bacteria) show forms ranging from coccoid (round) to rodlike to filamentous. Some pathogenic species such as Mycobacterium tuberculosis and Corynebacterium diptheriae are also pleomorphic.
Bacteria are often individual but some species take on a group arrangement based on the way cell division and subsequent separation of the daughter cells occur. Most of the Gram-negative bacilli (rods) are found singly (Escherichia coli) or, sometimes, characteristically in pairs (Klebsiella pneumoniae). The cocci, Streptococcus pneumoniae and Neisseria are called diplococci because they tend to pair. Bacilli found in chains include some Bacillus species. The coccus genera that most often form chains are named Streptococcus for this defining arrangement. A few cocci make regular packets of four or eight (Micrococcus) and some are seen in irregular clumps that resemble bunches of grapes (Staphylococcus). Short rods that form parallel lines, called palisades, include the species that causes diptheria, Corynebacterium diptheriae. Chinese character formation describes a sharply angled bacterial arrangement. Because of their waxy cell walls, Mycobacterium species are difficult to emulsify and tend to stick together in clumps. The pathogen in this group, Mycobacterium tuberculosis, may form long cords of cells.
Keep in mind that individual cells may show deviations from these standard forms. For example, cocci of Neisseria show flattened sides, making them bean-shaped. The rods of Corynebacterium and Mycobacterium often appear club-shaped, with swollen ends or knobs. Both groups may show irregular staining. The diplococci of Streptococcus pneumoniae often appear slightly elongated and lancet-shaped (with one flattened end and one tapered end).
Making a Bacterial Smear
Activity 2: Prepare a Bacterial Smear Slide of Serratia marcescens and Staphylococcus epidermidis and a mixture of both bacteria.
This protocol is found below and at BISC209: Preparing a bacterial smear slide in the Protocols section of this wiki.
Preparing a bacterial smear slide
1. Label a clean, glass slide with a graphite pencil on the far left of the slide with SE, SM, MIX. (The decolorizer in the Gram stain can remove your labels if you use pen or wax pencil.) By convention, labels (top to bottom) match smears (left to right).
2. Place three very small loopfuls of deionized water on the slide as far from each other as possible. (You can use the deionized water bottle on your bench; remove the cover and dip your loop in since sterility is not required for this step.
3. Flame the loop, allow it to cool for a few seconds and touch the cooled loop to a colony of S. epidermidis , picking up a TINY bit of white growth from the bacterial colony. An invisible amount of growth obtained from just touching the cooled loop to the colony is fine.
4. Place the loop with the bacterial growth into the drop of water on far left of the slide. Use a circular motion to make a smooth suspension of the bacteria in the water. Stop when there is a circle of emulsified bacteria about the size of a nickle on the slide. Be sure to leave room for the adjacent drop of water to be spread to a similar size without mixing the two smears.
5. Reflame the loop.
6. Repeat step 4 with the Serratia marcescens in the middle drop of water and then, without flaming your loop, touch the loop to the drop of water on the far right and mix briefly.
7. Reflame your loop and touch it to a Staphylococcus colony again. Place the loop in the far right drop of water mixing it with the Serratia and spread the drop as in step 4 to create a mixed smear.
6. Allow the slide to air dry completely! Be sure all the water on the slide has evaporated before proceeding to heat fixation!!! This drying step is crucially important. If you are impatient, you will "explode" the cells in the next step .
7. Heat fix (to kill and attach organisms to the slide) by quickly passing the slide (smear side up) through a flame 3 times. Use a clothes pin or slide holder and avoid contact with hot glass.
An example of a multiple smear labeled slide:

The Gram Stain
Background on Using Stains in Bacteriology
The first of the dyes most useful to bacteriologists was a reddish violet dye, mauvein, synthesized in England by William. H. Perkin, and patented by him in 1856. This synthetic dye and others were immediately appreciated by histologists, but were not applied to bacterial cells until Carl Weigert (a cousin of Paul Ehrlich) used methyl violet to stain cocci in preparations of diseased tissue in 1875. Subsequently, the use of various synthetic dyes for bacteriological preparations developed rapidly when they were promoted through the publications of Robert Koch and Paul Ehrlich.
The synthetic dyes are classified as acid dyes, or basic dyes, depending on whether the molecule is a cation or an anion. The introduction of the terms acidic and basic was unfortunate because it would be more revealing to refer to them as cationic or anionic dyes. A look at the structural formula reveals the nature of the dye.
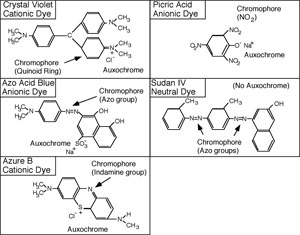
Each dye molecule has at least two functional chemical groupings. The auxochrome ionizes and gives the molecule the ability to react with the substrate, while the unsaturated chromophore absorbs specific wavelengths of light. The color of the solution obtained is that of the unabsorbed (transmitted) light. To be a dye, the molecule must have both auxochrome and chromophore groups. The auxochrome is usually an ionized carboxyl, hydroxyl, or pentavalent nitrogen group. The chromophore may have unsaturated nitrogen bonds such as azo (-N=N-) indamine (-N=), nitroso (-N=O) or nitro (O-N=O), groups; or unsaturated carbon to carbon, carbon to oxygen, or carbon to sulfur bonds, such as ethenyl (C=C), carbonyl (C=O), C=S, or the quinoid ring (= = =).
Resonance is also important to color. In crystal violet, an electron resonates between the three benzene rings. As the pH of the solution is lowered, the resonance becomes more and more restricted. When the resonance is restricted from three to only two benzene rings, the solution turns from violet to green, and then to red when resonance between the two rings ceases.
Cationic dyes will react with substrate groups that ionize to produce a negative charge, such as carboxyl, phenolic, or sulfhydryl groups. Anionic dyes will react with substrate groups which ionize to produce positive charges, such as the ammonium ion. Any substrate with such ionized groups should have an ability to combine with cationic or anionic dyes. Generally, the most important staining substrates in bacterial cells are proteins, especially the cytoplasmic proteins; however, other substances also have dye affinity. These include amino sugars, organic acids, nucleic acids, and certain polysaccharides.
Sudan III, or sudan black B, is a popular stain for fatty material. It does not have an auxochrome group, and is insoluble in water, but soluble in fatty material. When a solution of sudan black B in ethylene glycol is placed over bacterial cells, the fatty material will dissolve some of the dye and thus take on the color of the sudan black. The staining effect is purely a solubility phenomenon, and not a chemical reaction, or physical adsorption.
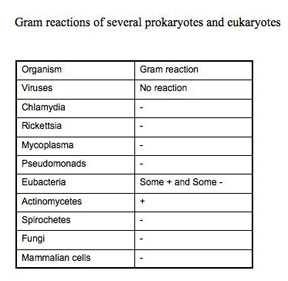
There are many stains that can reveal the morphology of the cell, and some simple stains, such as methylene blue, are quite good for viewing bacteria. The Gram stain is especially useful because it not only reveals bacterial morphology, but also is a differential stain. A differential stain differentiates organisms. (A differential stain shows a visible difference between different groups of organisms based on some characteristic they do not share, even though the procedure to stain the different looking organisms is the same). The Gram stain relies on cell wall differences between groups of bacteria.
The Gram staining procedure as it is done today, involves: a) primary staining of all cells with crystal violet, b) precipitating the primary stain dye within the cells with iodine (a mordant), c) removing the dye-iodine precipitate from some cells (the Gram-negative) with a decolorizer such as 95% ethanol, acetone, or n-propyl alcohol, and d) counter-staining of the decolorized cells with safranin. Organisms that retain the crystal violet primary dye are termed Gram-positive, while those which lose the primary stain and show the red safranin counter-stain are termed Gram-negative. This differentiation is not absolute, because it is based on the differences in the rate at which the primary dye is lost from the cells. If you over decolorize for too long or with too harsh a decolorizer, Gram-positive organisms will appear Gram-negative. Truly Gram-positive cells, such as Bacillus subtilis or Staphylococcus aureus, will not retain the primary dye if the iodine step is omitted. Criteria for a true Gram-positive state include the requirement of iodine following the crystal violet.
Since the term Gram positive or Gram negative actually refers to a type of cell wall, not all organisms that retain the primary dye of the Gram procedure are really Gram-positive, because they lack that particular cell wall composition. For example, Mycobacterium species have a different type of cell wall but they will take up and retain crystal violet if you use heat. In this case, the crystal violet will be resistant to harsh decolorization and be retained. However, a Mycobacterium type cell wall does not require the use of a mordant, like iodine, to precipitate the stain. True Gram-positive organisms do not retain the primary crystal violet without precipitation by a mordant. Using crystal violet with heat, harsh decolorization, and no mordant describes an acid-fast stain rather than a Gram stain. Mycobacteria have an acid-fast type cell wall; they are neither Gram-positive or Gram-negative, despite the fact that they will appear purple if you do a Gram-stain on them.
Activity 3: Preparing a Gram Stain
The Gram stain is a standard staining technique useful for the identification of culturable bacterial organisms and you will perform it now.
Use the slide prepared in Activity 2 and follow the Gram Stain Protocol found below and in BISC209: The Gram Stain in the protocol section of this wiki.
Gram Stain Procedure:
To Gram stain the bacterial smear slide that you prepared in Activity 2 that has 3 different smears on it, you must be careful to apply the staining reagents liberally so all the smears are evenly and completely covered and you must be sure to expose each smear to each reagent for the same amount of time.
1. Place your smear on the staining tray. It is important that the slide be level during staining so use paper towels under the tray to get it leveled. If you do, it is much easier to be sure that your smears will be covered evenly with each reagent.
2. Dispense just enough Crystal Violet solution (0.5% crystal violet, 12% ethanol, 0.1% phenol) to completely cover each smear and stain for 1 minute. (Crystal violet is the primary stain.)
3. Rinse the slide by lifting it at a 45 degree angle (using gloves or a clothes pin or slide holder) and use a squirt bottle to direct a very gentle stream of water slightly above the top smear. Rinse until the waste water coming off at the bottom is relatively clear; drain off excess water by touching the edge of the slide to a paper towel.
4. Dispense just enough Gram's Iodine (mordant)to completely cover each smear. Let stand for 1 minute. Rinse thoroughly with a gentle stream of water as in Step 1.
5. Lift the slide at a 45 degree angle and drip Decolorizing Reagent (80% isopropyl alcohol, 20% acetone) down the length of the slide making sure it comes in contact with all three smears. This step is tricky as it is easy to over- or under-decolorize. Do this for 10 seconds and IMMEDIATELY rinse, as in step 3, with a gentle stream of water.
6. Place the slide flat on the staining tray and dispense just enough Counterstain (0.6% safranin in 20% ethanol) to cover each smear. Let stand for 2 minutes; rinse with water as in step 3.
7. Blot dry using the bibulous paper package found in your orange drawer. Do not tear out the pages, just insert your slide and pat it dry.
8. Clean up your area; rinse your staining tray in the sink and leave it to drain upside down on paper towels.
9. Observe your stained microbes microscopically following the correct procedure for using the the oil immersion objective on your compound brightfield microscope. The directions for using the microscope are found in the protocol section of this wiki: BISC209: Microscopy
Use of the Compound Light Microscope
Activity 4: View your stained bacteria.
Refer to the directions for using your compound brightfield microscope BISC209:_Microscopy found in the Protocols section. Today you will use only the 10x and 100x objectives. Remember also to read and follow the directions for care of this precision instrument (particularly on how to avoid getting immersion oil on any objective other than the 100x oil immersion lens). Be aware that there would be no field of microbiology if there weren't good, functioning microscopes to view this unseen world.
More Tools & Techniques of Microbiologists
Use and Calibration of Micropipets
How to Use a Micropipettor
The following website Using a Micropipette has more detailed information about micropipette use.
- Decide which of your micropipets is appropriate for the volume you want to measure and dispense.
- Adjust the volume dial to the appropriate volume, recognizing that your P1000 must have a zero added to the bottom of the volume display boxes and the P20 has a decimal between the bottom and second volume display boxes.
- Firmly seat a new micropipet tip of appropriate size on the micropipets.
- Depress with the thumb plunger to the first stop and hold the pipettor in this depressed position (DO NOT depress fully).
- Dip the micropipet into the solution far enough to account for the volume that will be withdrawn but not so far as to immerse the micropipet barrel.
- Gradually release the plunger, drawing fluid into the tip without forming bubbles.
- Carefully slide the micropipet tip along the side of the tube to remove any unwanted droplets of fluid sticking to the tip's surface.
- Expel the fluid into the desired container by touching the micropipet tip to the inside surface of the container and slowly depressing FULLY the plunger.
- Continue to hold the plunger in the fully depressed position as you remove the micropipet from the container.
- Eject the tip by pressing the eject button (if your micropipet has one) into an appropriate place (only tips that have been contaminated with microorganisms need to be ejected into an autoclave bag).
Don'ts in Using Micropipets
- DO NOT force or rotate the volume adjustment knob past the upper or lower ranges specified on the top of the micropipet.
- DO NOT use a micropipet without a tip since the precision piston that measures the volume can be ruined.
- DO NOT put the micropipet down on your bench with a filled tip since fluid can run back into the precision piston.
- DO NOT allow the micropipet plunger to snap back after fluid is either dispensed or drawn.
- DO NOT immerse the micropipet barrel into fluid.
- DO NOT flame the micropipet tip.
Activity 5: Protocol for Micropipet Calibration
1. To calibrate your P1000, P 200, and P 20 micropipets, label 6 microfuge tubes (1-6) and weigh them on a top loading balance. Don't forget to tare the balance. Record the weights in a table in your lab notebook, like the one below.
2. Using the information in the table below, pipet the specified volumes into the pre-weighed microfuge tubes prepared in step 1 and then reweigh the tubes. Record all weights.
3. Calculate the weight of the water in grams by substracting the dry weight from the weight of the tubes with water. Note that 1000 microliters of water should weigh exactly 1 gram at room temperature.
4. If the water in any tube weighs more or less than 1 gram, repeat that tube. Ask your instructor to check your pipetting technique if your calibration continues to be off after several repeated attempts.
| Tube # | Pre-weight | Tube Vol. in µl using P20 |
Vol. in µl using P200 |
Vol. in µl using P1000 |
Weight of water grams |
|---|---|---|---|---|---|
| 1 | _____ | 10 | 0 | 990 | ____ |
| 2 | _____ | 0 | 100 | 900 | ____ |
| 3 | _____ | 20 | 175 | 805 | _____ |
| 4 | _____ | 2 | 88 | 910 | ______ |
| 5 | _____ | 0 | 200 x 5 | 0 | _____ |
| 6 | _____ | 20 x 5 | 0 | 900 | _____ |
CLEAN UP
1. All culture plates that you are finished with should be discarded in the big orange autoclave bag near the sink next to the instructor table. Ask your instructor whether or not to save stock cultures and plates with organisms that are provided.
2. Culture plates, stocks, etc. that you are not finished with should be labeled on a piece of your your team color tape. Place the labeled cultures in your lab section's designated area in the incubator, the walk-in cold room, or at room temp. in a labeled rack. If you have a stack of plates, wrap a piece of your team color tape around the whole stack.
3. Remove tape from all liquid cultures in glass tubes. Then place the glass tubes with caps in racks by the sink near the instructor's table. Do not discard the contents of the tubes.
4. Glass slides or disposable glass tubes can be discarded in the glass disposal box.
5. Make sure all contaminated, plastic, disposable, serologic pipets and used contaminated micropipet tips are in the small orange autoclave bag sitting in the plastic container on your bench.
6. If you used the microscope, clean the lenses of the microscope with lens paper, being very careful NOT to get oil residue on any of the objectives other than the oil immersion 110x objective. Move the lowest power objective into the locked viewing position, turn off the light source, wind the power cord, and cover the microscope with its dust cover before replacing the microscope in the cabinet.
7. If you used it, rinse your staining tray and leave it upside down on paper towels next to your sink.
8. Turn off the gas and remove the tube from the nozzle. Place your bunsen burner and tube in your large drawer.
9. Place all your equipment (loop, striker, sharpie, etc) including your microfuge rack, your micropipets and your micropipet tips in your small or large drawer.
10. Move your notebook and lab manual so that you can disinfect your bench thoroughly.
11. Take off your lab coat and store it in the blue cabinet with your microscope.
12. Wash your hands.
13. See you next time!
Vist to the GreenHouse--Introduction to the Soil Communities & Diversity Project
If time permits today, we will take a walk through the Wellesley College Margaret Ferguson Greenhouses. Most of your work this semester will be an investigative project on exploring the microbial diversity of a greenhouse habitat. In table groups of four students, you will decide which of the habitats or micro-environments you and your group will investitgate: 1.tropical house; 2. seasonal display house--cool temperate; 3. water plant house (hydrophyte)---warm, moist temperate. We will collect soil samples next week and begin our work to identify the bacteria in these communities and explore their contributing roles.
Link to the Wellesley College Margaret Ferguson Greenhouses: [[5]]
You can download a pdf file of a greenhouse map and tour route here: [[6]]
Assignment
Get together with your partners and decide on which of the three Greenhouse habitats you would like to do your soil bacterial communities project. Since each group must chose a different habitat, those who decide most quickly are more likely to get their first choice. Your choices are: the seasonal display room (cool temperate- around the Durant camellia), the water plants room containing the hydrophytes (warm temperate--around the bamboo), or in the tropical house (anywhere in the center circle where the plants are not in isolated pots). Visit the greenhouse (hours and more information found at: | http://www.wellesley.edu/WCBG/Visit/info.html ) with your group or on your own, using the downloadable greenhouse map to guide you. Make notes about your habitat and how it is different from others. You can read ahead in Lab 2 Part A to see what information you need to record in your lab notebook about your habitat.
Start doing a little research on the soil bacteria that are most likely to be found in your selected habitat and how you might use selective or enrichment media to increase your chances of growing from your habitat the widest variety of culturable soil organisms possible. There are many articles posted to the References folder on the First Class Lab Conference that may help you with this task and a lot of information on media and BISC209: Enrichment in the Protocols section of this wiki. Note that you don't have to turn in a strategy for enrichment and selection yet, but devising such a "game plan" is coming.
Read the introduction to the soil communities and diversity project found at BISC209:Project1 and all of the LAB 2 protocols and information found at BISC209: Lab2. Outline or make a flow chart of your lab work for LAB 2 in your lab notebook. If you are unfamiliar with keeping a lab notebook, refer to the BISC209/S10:Resources section of the wiki where you will find some guidelines.
Homework Questions
You can download a .doc file of these questions at Media:BISC209Homework_questions1.doc
You will turn in the answers to these questions at the beginning of the next lab:
(You will need to use your text book to discover the difference in cell wall composition that is the basis for the Gram stain's ability to differentiate some bacteria)
1. Which organism, Staphylococcus epidermidis or Serratia marcescens, is Gram positive? Which is Gram negative?
2.. What color is a Gram negative organism and why?
What color is a Gram negative organism and why?
3. Explain the differences in cell wall composition in Gram negative and Gram positive bacteria and why those differences allow differentiation between Gram negative and Gram positive bacteria.
4. Compare and contrast the morphology(shape and arrangement)of the two bacterial species you stained this week.
5. Describe in detail the proper way to pipet 1 μL of a solute and 20μL of
solvent to combine them in a microfuge tube. Be sure to include which micropipet to use, the order of ingredients (if not specfied in the protocol)and describe any techniques used to improve accuracy and precision.
Links to Labs
Lab 1
Lab 2
Lab 3
Lab 4
Lab 5
Lab 6
Lab 7
Lab 8
Lab 9
Lab 10
Lab11
Lab 12