BME100 s2014:T Group7 L3
| Home People Lab Write-Up 1 | Lab Write-Up 2 | Lab Write-Up 3 Lab Write-Up 4 | Lab Write-Up 5 | Lab Write-Up 6 Course Logistics For Instructors Photos Wiki Editing Help | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
OUR TEAM
LAB 3A WRITE-UPDescriptive Statistics
Results
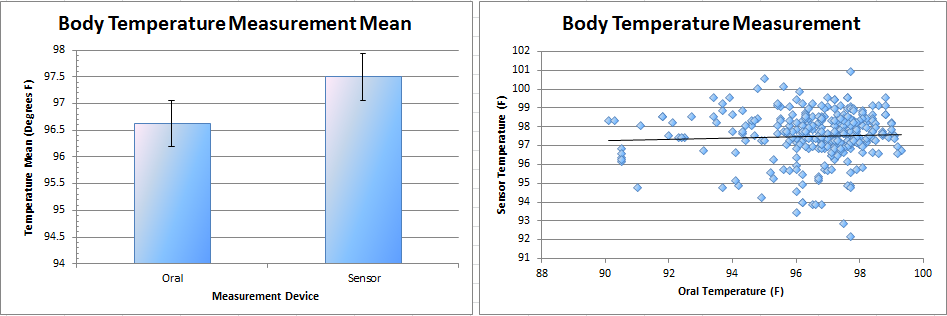
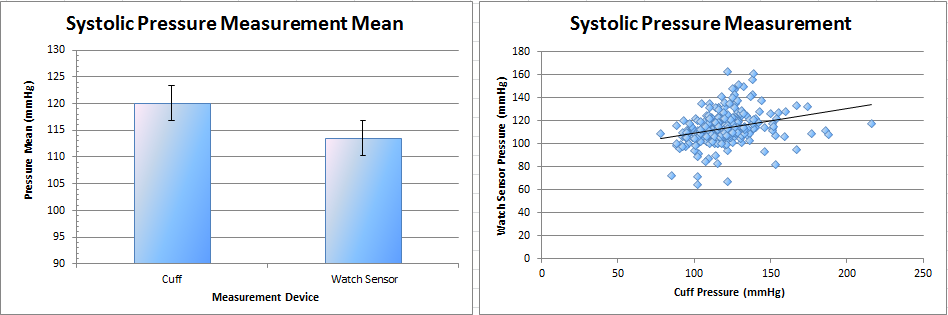
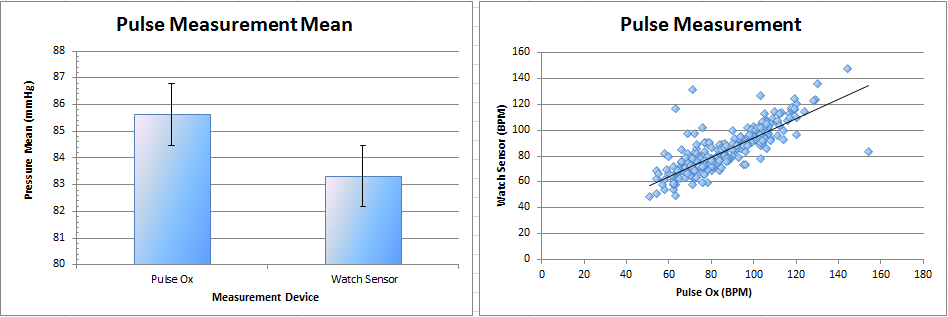
AnalysisBody Temperature MeasurementThere was very little correlation (4.8%) between measuring body temperature with the oral thermometer, used as the experiment standard, and the RAIIN sensor. The RAIIN sensor tended to measure significantly higher temperatures than the oral thermometer. Systolic Pressure MeasurementThere was some correlation (27.6%) between systolic pressure measurements taken with the blood pressure cuff, used as the experiment standard, and the watch sensor. A significant trend existed wherein the watch sensor tended to consistently measure a lower systolic pressure than the blood pressure cuff. Pulse MeasurementThere was substantial correlation (81.4%) in pulse rate measurements taken with the pulse oximeter, the device used as the experiment standard, and the watch sensor. Similar to the blood pressure measurements taken with the watch sensor, pulse measurements taken with the watch sensor tended to measure consistently lower than the pulse oximeter.
DiscussionRAIIN SensorThe RAIIN sensor appeared to be extremely inaccurate at measuring body temperature. With almost no correlation between the RAIIN sensor and the oral thermometer, measurements taken from the RAIIN sensor can be said to be at best educated guesses at body temperature. For serious applications where accurate body temperature is required, this group would not recommend using the RAIIN sensor. Beyond accurate measurements, the RAIIN sensor was unwieldy and cumbersome to use. The tester for this experiment constantly complained of the pain associated with using the device. The sensor required careful and uncomfortable accommodations to wear properly, having an awkward shape and a very small surface for dermal contact. Beyond the extra steps required to use and secure the device, no problems were observed. The software for this device worked as expected without incident. As noted by the tester, a substantial improvement to the device would be to increase the area on the device able to take measurements. This would preclude the need to wear the device in potentially awkward or painful positions. Another improvement would be to include a purpose-built attachment system, adjustable for each individual user of the device. Attaching the device in a position able to take proper measurements proved to be an unnecessarily clumsy process. Without relying on user dexterity to attach the device (an endeavor that required more than one person), usability could be increased substantially for relatively little cost. Watch SensorThe watch sensor proved to be mostly ineffective at measuring accurate systolic pressure when compared to the blood pressure cuff and reasonably accurate at measuring pulse rate compared to the pulse oximeter. This group would recommend using the watch sensor only in a limited capacity. This could be when accurate equipment is not available, when extremely accurate blood pressure and pulse rate are not needed, or when ease of use is preferable to more accurate measurements. The watch sensor main advantage is that it is simple to use, comfortable for the wearer, and can provide both blood pressure and pulse with one device. The tester did not make note of any significant problems with using the device. One potential design flaw to note is the strict positioning requirement of the watch sensor. The sensor had a very low tolerance for variations in positioning on the tester's wrist. It may be possible that erroneous readings were taken if the sensor were not in a perfectly optimal position. An improvement that could be made if this is the case would be to redesign the strap system to be less prone to inadvertent adjustments. This, however, would have the detriment of likely increasing the size and cost of the device.
LAB 3B WRITE-UPTarget Population and NeedThe target population for our product, Lass-E, includes the elderly with mental impairments and the people taking care of them. This device will be able to relate the location and pulse of the individual to an app for all related people to easily access their condition. This device will alert all emergency contacts who are registered as care givers of the patient when the elderly person is outside a specific radius or when their pulse exceeds or drops below a certain threshold. This device is essential because there are no devices that allow for easy monitoring of the elderly. The care takers of the elderly have lives of their own and this device allows them to go about their life without worrying about the health and safety of their loved one.
Device DesignOur device is wrapped around the upper arm. Included in the device is a built in GPS device that will monitor the location of the person and relay it to an app. The device also includes a pulse monitor to check in on their health remotely. Inferential Statistics
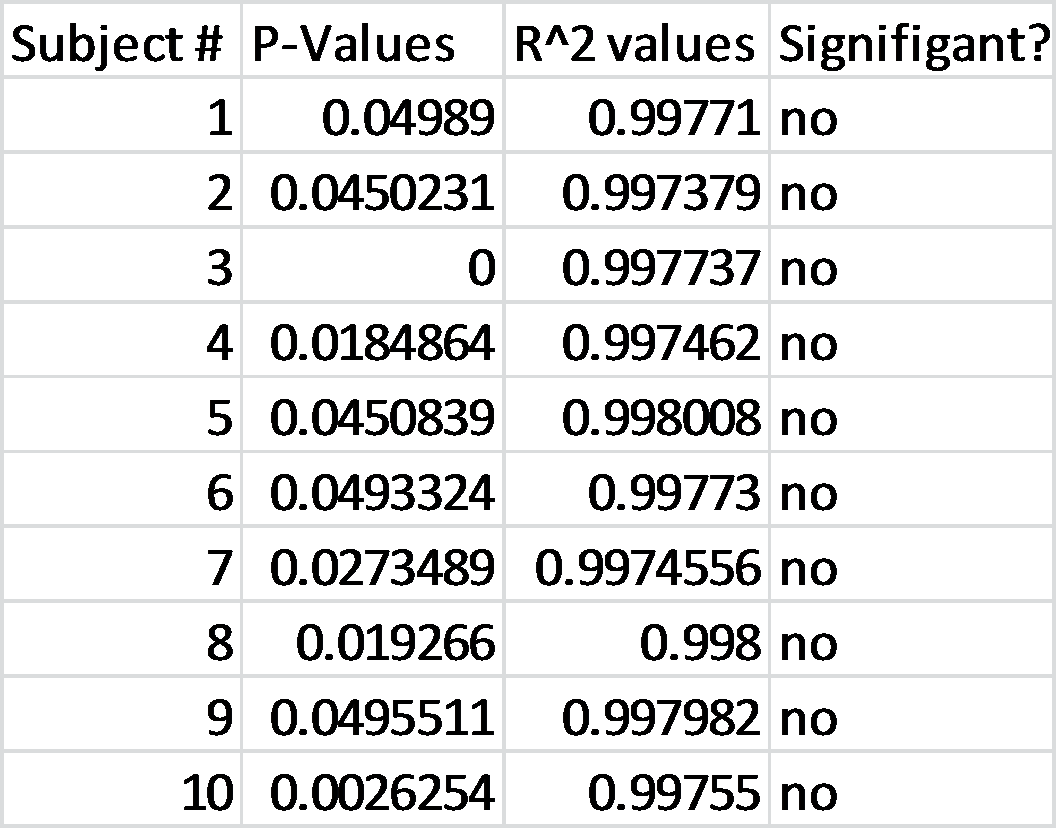
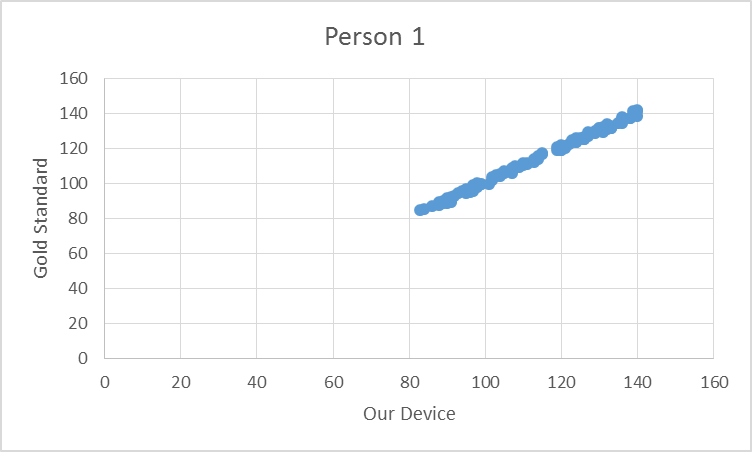
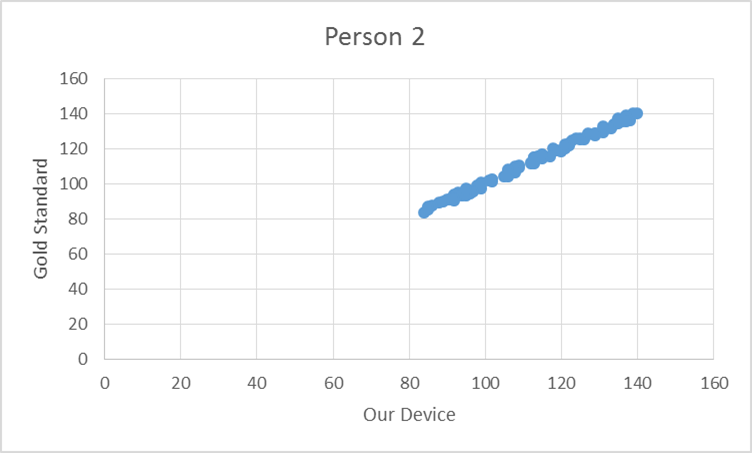
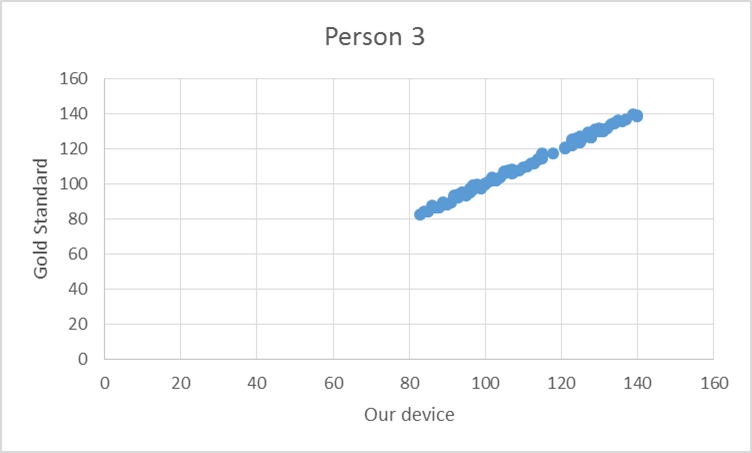
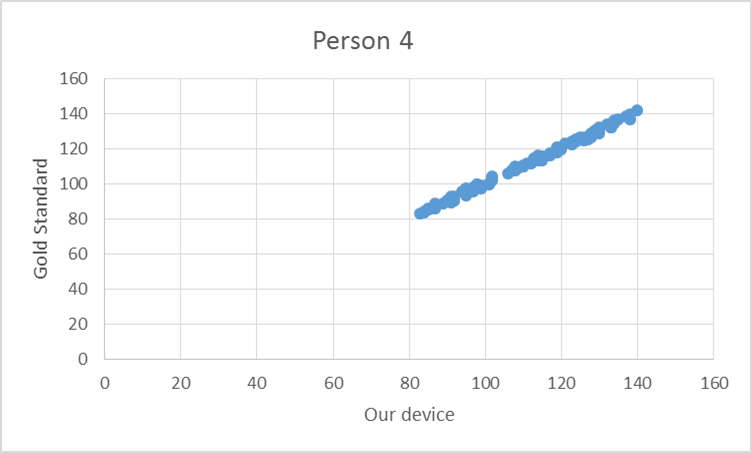
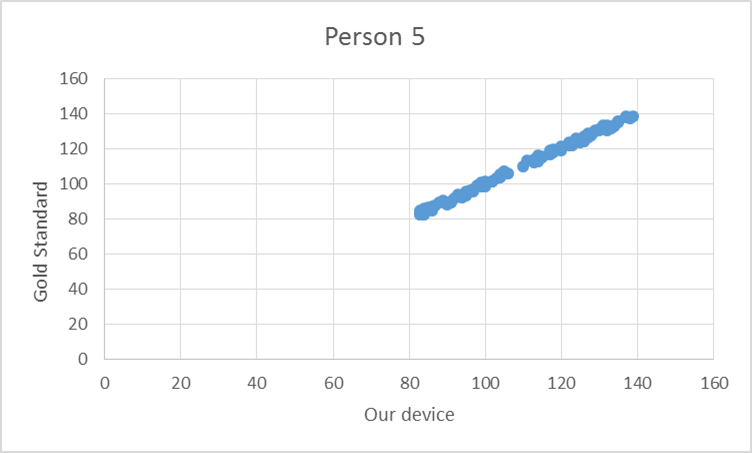
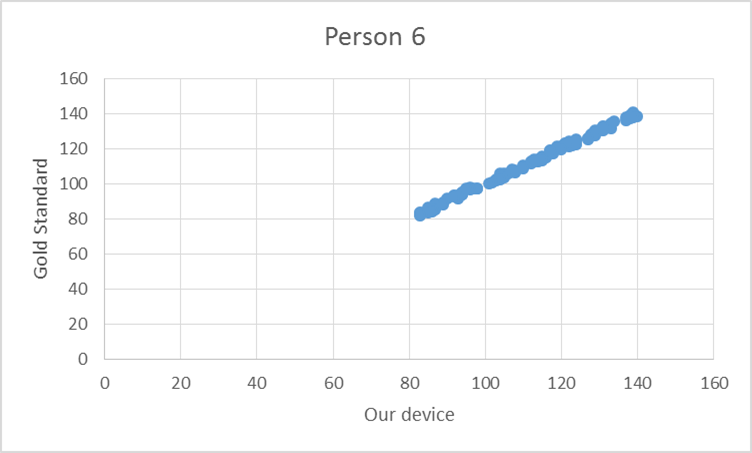
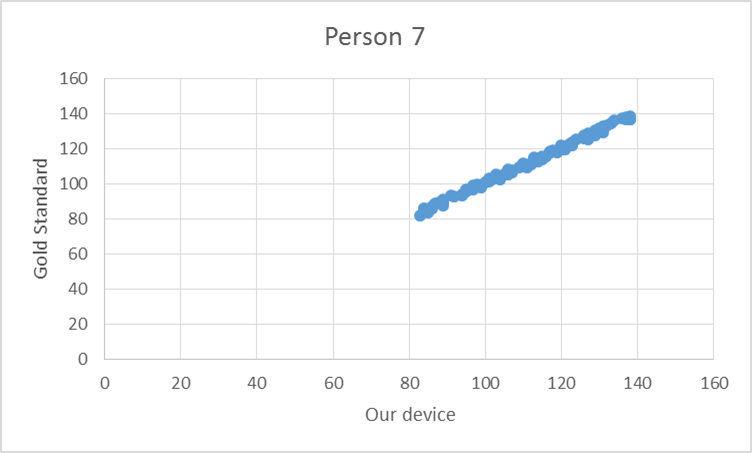
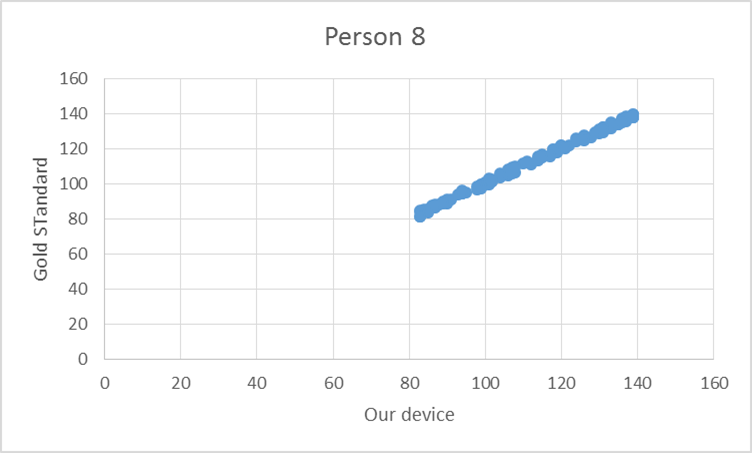
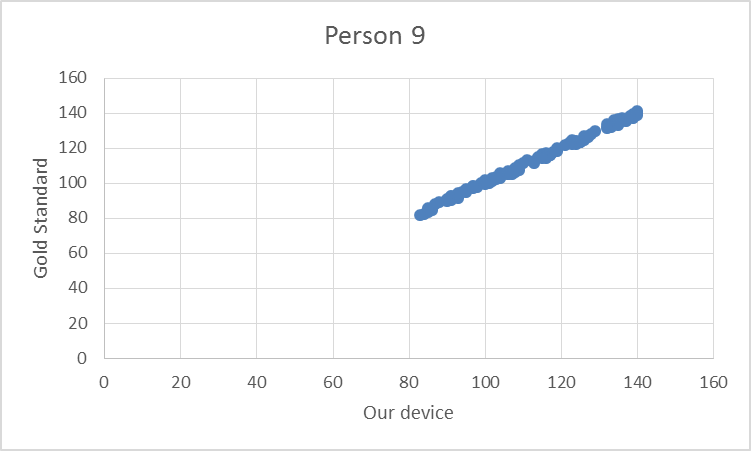
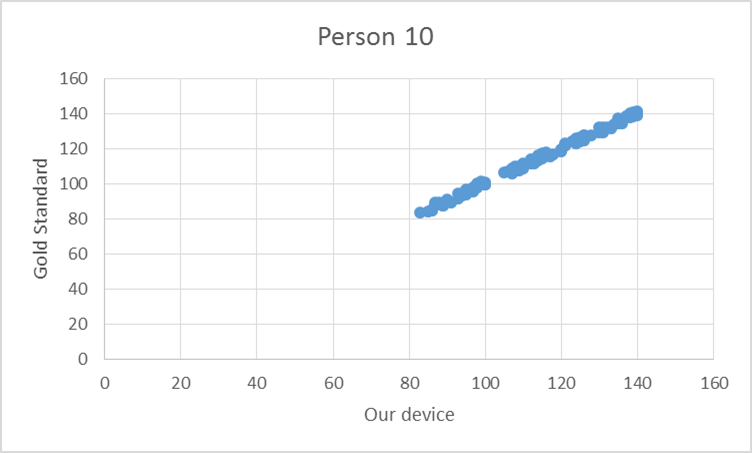
To test the device, the pulse from ten elderly individuals was recorded using both the gold standard and our device. Based on the T-test values and the R^2 values there is no statistical difference between Lass-E and the gold standard.
GraphShown below is the correlation between the gold standard and Lass-E. As can be seen the data set is almost in a straight line denoting that both devices produce similar results when testing pulse. This implies that both devices perform at the same level.
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||