BME100 f2016:Group8 W8AM L3
| Home People Lab Write-Up 1 | Lab Write-Up 2 | Lab Write-Up 3 Lab Write-Up 4 | Lab Write-Up 5 | Lab Write-Up 6 Course Logistics For Instructors Photos Wiki Editing Help | ||||||||||||||||||||||||||||||||||||
|
OUR TEAM
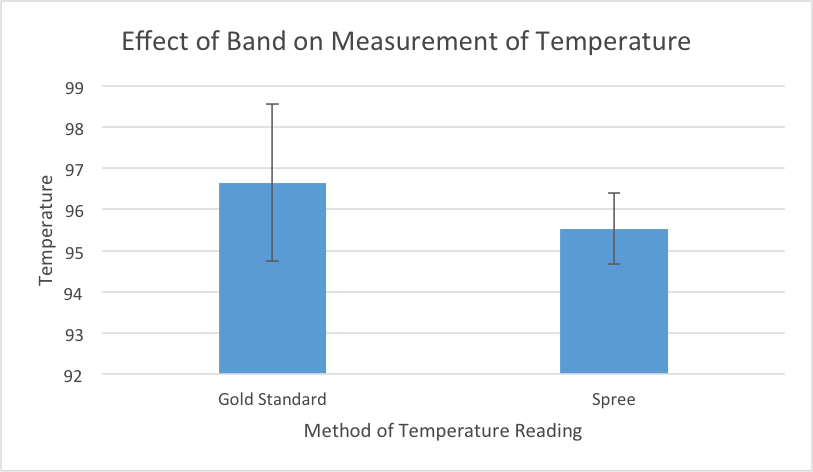
LAB 3 WRITE-UPDescriptive Stats and GraphTemperature Data:
Inferential StatsTemperature (Spree vs. Gold Standard): p-value (paired t-test): 1.09676 E^(-21) This p-value is less than 0.05, which shows that there is a statistical difference between the two means between the temperature readings of the Spree Band and the Gold Standard (oral thermometer). This means that the Spree Band's temperature sensor is not effective and accurate in its measurements of an individual's temperature, as the p-value signifies that there is a statistical difference between the two means of the Spree Band readings and the Gold Standard readings, and the temperature readings between the Spree Band are not very close to the actual readings of the Gold Standard. Pearson's R Correlation Coefficient: 0.192798089 ANOVA p-value (disregard since not a 3 or more test): 1.85543 E^(-20)
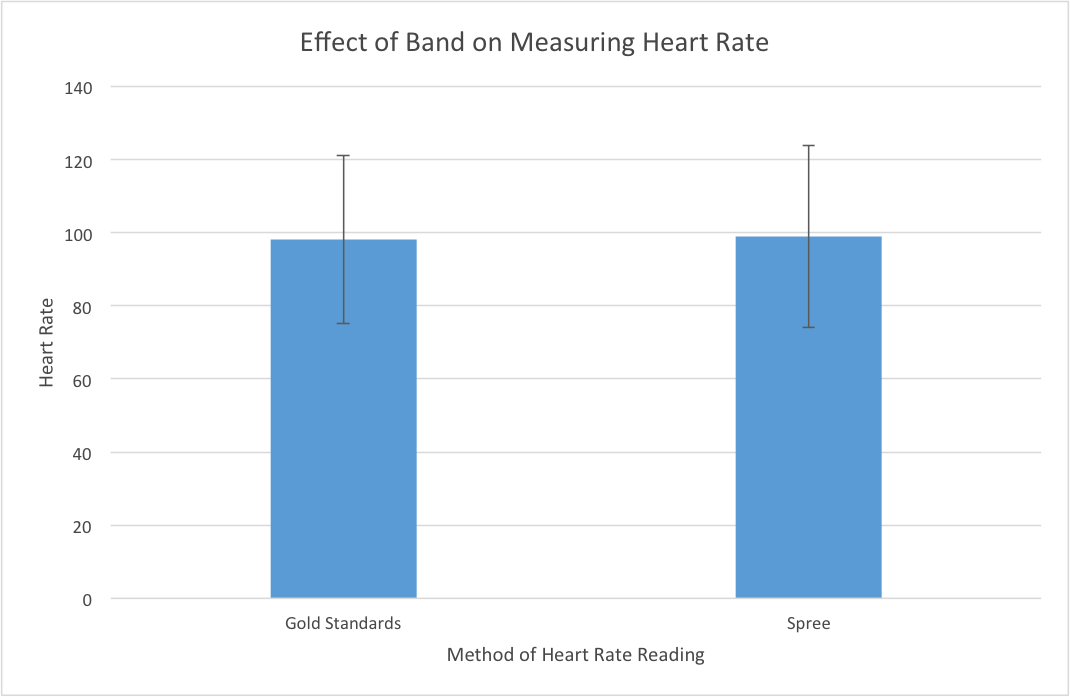
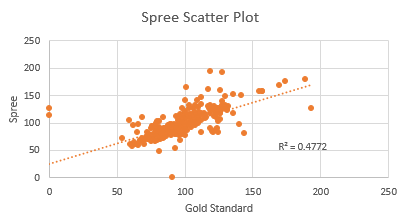
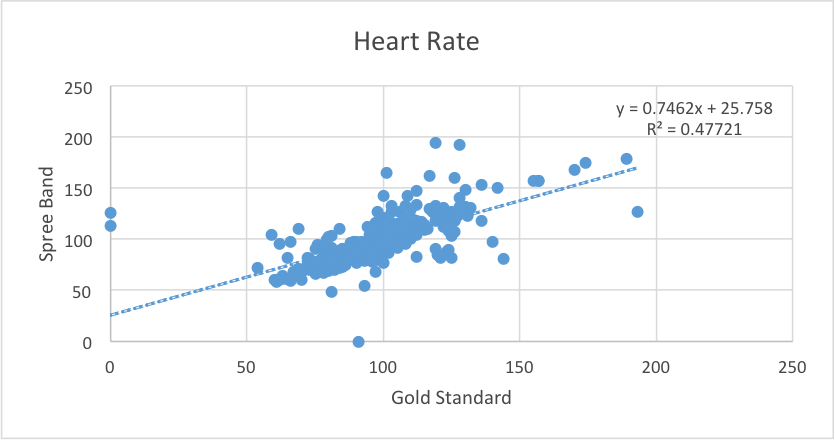
Heart Rate (Spree vs. Gold Standard): p-value (paired t-test): 0.427116193 This p-value is greater than 0.05, which shows that there is no statistical difference between the two means between the heart rate readings of the Spree Band and the Gold Standard (pulse ox). This means that the Spree Band's heart rate monitor is effective and accurate in its measurements of an individual's temperature, as the p-value signifies that there is no statistical difference between the two means, and the heart rate readings between the Spree Band are very close to the actual readings of the Gold Standard. Pearson's R Correlation Coefficient: 0.690806489 ANOVA p-value (disregard since not a 3 or more test): 0.661777944
Design Flaws and RecommendationsBased off the data collected and the statistical analysis done on the data, it can be concluded that the Spree Band is not an effective tool in measuring the temperature of an individual, but is an effective and accurate device in measuring the heart rate of an individual. Our null hypothesis stated that if the p-value was less than 0.05, then there was a statistical difference between the two means (Spree Band Readings and Gold Standard Readings), which would mean that the readings from the Spree Band were inaccurate compared to the Gold Standard temperature and heart rate readings. For these data sets, Suntronic would have wanted to see a p-value greater than 0.05, which signifies that there is no statistical difference between the two means, meaning that the readings of the Spree Band are accurate to the actual readings of the Gold Standard. The p-value was calculated for the temperature readings of the Spree Band versus the Gold Standard at 1.09676 E^(-21), which indicates that there was statistical difference between the groups in the means, which signifies that the Spree Band did not work effectively and accurately as a temperature sensor. However, when the p-value was calculated for the heart rate readings of the Spree Band versus the Gold Standard, it was found to be 0.427116, which signifies that there is no statistical difference between the means, which signifies that the Spree Band did work effectively and accurately as a heart rate monitor. Moreover, the Pearson's "r" coefficient was calculated for both data sets. The Pearson r for the temperature readings was calculated to be 0.192798089, which shows a weak correlation between the two means of the Spree Band temperature readings and the Gold Standard temperature readings. The Pearson r for the heart rate readings was calculated to be 0.690806489, which shows a stronger correlation (closer to 1) between the two means of the Spree Band heart rate readings and the Gold Standard hear rate readings. Overall, the Spree Band works as an accurate heart rate monitor but does not effectively work as a temperature sensor. It is also aesthetically unappealing as it goes around the forehead, which users may find as a flaw with the device.
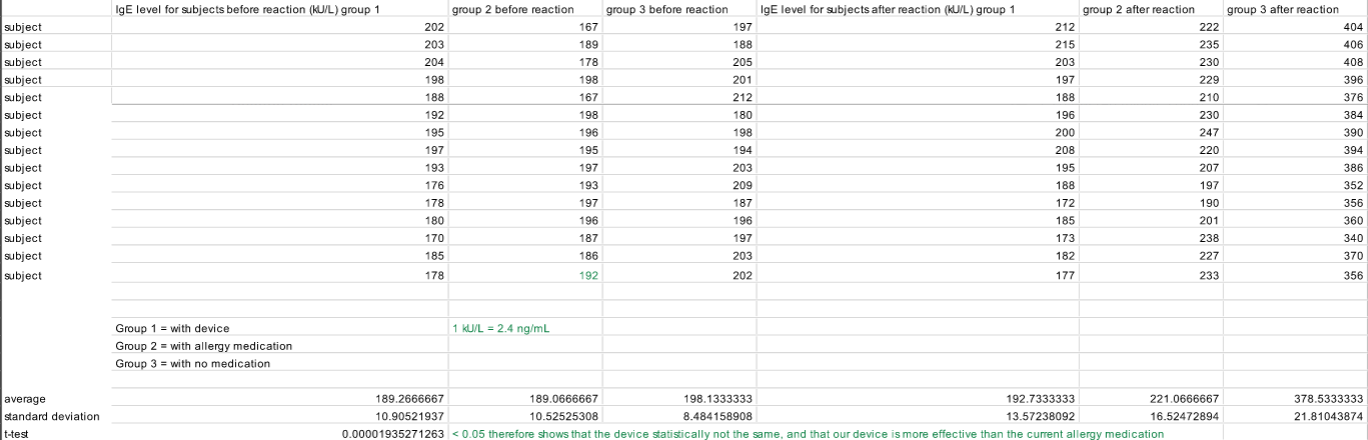
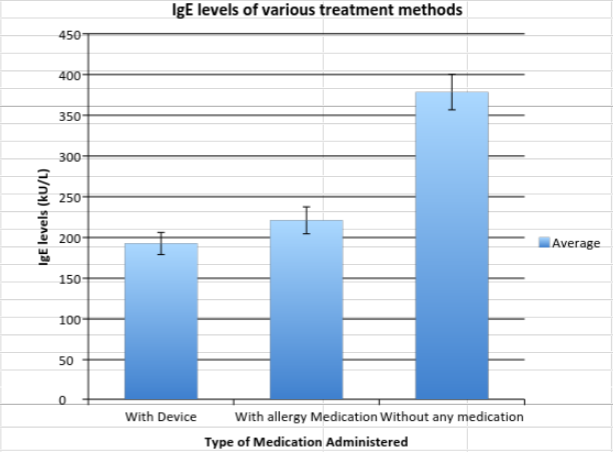
Experimental Design of Own DeviceObservation: Current nasal allergy medication can be tedious for patients to take, as well as ineffective in delivering the drug to the allergic site. Question: Can a direct delivery system of antihistamines be used to more effectively combat allergic reactions in individuals? Hypothesis: Our device is a more effective and efficient method of distributing antihistamines to a patient than the current allergy medication (p-value < 0.05). Definitions: In this experiment, the independent variable will the method of allergic medication, the dependent variable will be the IgE levels of the test subjects of each group, and the control group will be the test subjects that are not allowed to take any allergy medication. Experiment and groups: We will put out an advertisement requesting people healthy individuals 18 and older to participate in an experiment testing a new device that could be a more effective solution to combating nasal allergies. Once we get 45 test subjects, we will split them into 3 different groups: one group will be receiving current nasal allergy medication as a solution, the second group will be receiving our device as a solution, and the third group will be the control group and will recieve no type of antihistamine medication. We will then expose all 45 test subjects to allergens such as pollen, dust, etc. in order to record their immunoglobulin E. (IgE) levels without medication and use that as a baseline to compare later results. The three groups will then be asked to either take a specific dosage of allergy medication per day, use the device implanted daily, or take no allergy medication for a week leading to the next test date. Once this week has passed, these three groups will come to the lab, where we will measure their IgE levels before exposing them to allergens. We will make sure this sample is unbiased by making sure that all test subjects do not exhibit any signs of allergic reactions (runny nose, itchy eyes, etc.). We will then expose these individuals to specific allergens that will cause an allergic reaction. Once an allergic reaction is viewed in the test subjects, or after the allergen has come into contact with the test subject, or after 15 minutes has passed since the test subjects were introduced to the various allergens, their IgE levels will be recorded and compared to their baseline IgE levels. What we should find is that individuals with the device have a more normal level of IgE in their bloodstream after they are exposed to various allergens, and that the IgE levels in the test subjects that will be taking the current allergy medication will be alittle higher than normal, showing that our device is more effective than the current method of combating allergic reactions.
| ||||||||||||||||||||||||||||||||||||