Preparation for Cell Culture - Alistaire Rauch and Abraham Waldman
Introduction: Materials and Preparation for Cell Culture
As microfluidics becomes more significant and notable for its ability to recreate in vivo environments, this area of research often implies the use of cells. Following specific guidelines and understanding the interaction between the cell culture and microenvironment is crucial as it will eventually lead to a more developed microfluidic cell culture technology [1].
Device Preparation
2D versus 3D Cell Culture

Most conventional cell culture methods (to date) utilize a two-dimensional (2D) approach which is characterized by culturing cells in monolayers upon a flat and rigid substrate [24]. Although this method does have its purpose, it has been proven to have limitations that make it unsatisfactory [24]. A notable discrepancy between two-dimensional and three-dimensional cell culture (3D) is that 2D lacks the surrounding 3D environment which is the underpinning to in vivo environments; consequently, 2D cultures can result in aberrant cell morphology or physiology concomitantly leading to inaccurate data [24].
An aspect to consider between 2D and 3D cell culture often involves culturing them. In comparison to 2D cell culture, usually grown as a monolayer upon a surface, 3D cell culture often results in spheroids which are aggregates of cells [24]. Sometimes, spheroids form through the foundation of a matrix whereas scaffold-free 3D cell spheroids can be generated through the hanging drop method, suspensions by the forced floating method, or agitation-based approaches [25]. The hanging drop method involves placing small aliquots of cells and a suspension liquid into a well which is then inverted; this causes drops to form (due to surface tension) where the cells aggregate at the bottom of the drops and proliferate [25]. Another simple method is the forced-floating method which is characterized by preventing cell attachment to a surface through surface modification; as a result, the cells localize and adhere to each other forming spheres [25]. With spheroids in 3D culture, cell-cell interactions and cell-matrix interactions closely mimic the in vivo environment [24]. Likewise, spheroids accurately represent tissues as the outer layers of spheroids include proliferating, quiescent, apoptotic, hypoxic, and necrotic cells, whereas the core cells receive less oxygen and nutrients [24].
Another difference between the two methods is exposure to medium and drugs; in 2D, cells are equally exposed to nutrients, growth factors, or drugs, while in 3D these elements may not penetrate the core of the spheroids [24]. In addition, gene/protein expression in 2D is often aberrant, whereas in 3D the cells exhibit profiles similar to those in vivo [25].

Substrate Stiffness
As cells require adhesion to an extracellular matrix (ECM) for survival, the stiffness of a substrate is also a consideration to make in designing cell culture. When cells adhere to a substrate, a strain is induced; the cell responds to this strain with a certain amount of resistance as a result of its cytoskeleton [26]. Although each cell and its cellular force response is different, it remains that cells on stiffer substrates maintain a more organized cytoskeleton [26].
A crucial aspect of stiffness concerns Young’s Modulus (E) which is the resistance of an object to deform; mathematically, it is the ratio of stress to strain forces [26]. To provide some reference points, mucous has an E of 10 pascals (Pa), the brain is around 100 Pa, muscle is around 12 kPa, tendon and cartilage range around a MPa, and bone and glass have an E exceeding 1 GPa [26]. From these numbers, it can clearly be understood that cells placed upon a plastic or glass substrate do not provide a suitable foundation capable of mimicking the physiological mechanical environment [26].
To meet the demand of this field, many developments have been made within biomaterials that can be incorporated into cell cultures; hydrogels (composed of collagen, fibrin, matrigel, etc.) are the most common. For example, Sun et al. used fibronectin coated polyacrylamide hydrogels with variable stiffnesses (13 to 68 kPa) to modulate the mechanical environment of bone marrow mesenchymal stem cells; they demonstrated stiffness increases directly correlated to an increase in cell spreading and adhesivity upon a substrate [27]. Similarly, Mabry et al. synthesized degradable polyethylene glycol (PEG) hydrogels with an elastic modulus from 0.24 kPa to 12 kPa; after polymerization of the gel, the elasticity increased having a direct effect upon the cells [28]. In all, a variety of various substrates exist and creating a tunable substrate that is personalized for a specific type of cell is one step closer towards mimicking the in vivo environment.
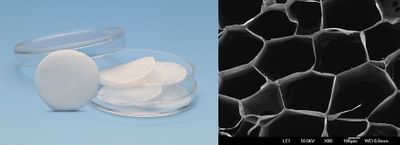
Cell Scaffolding
One of the main uses of cell culture microfluidics is for drug testing. Conventional drug testing models often result in inaccurate data for in vivo responses; rather than using cell culture in two-dimensional monolayers, cells cultured in a three-dimensional extracellular matrix (ECM) are more likely to result in physiologically relevant cells [2]. A potential reason for this failure may be a result of our lack of understanding of culturing cells in such a way that mimics their specific in vivo conditions (as not to alter their phenotypic characteristics). To achieve this ideal environment, the replication of an in vivo microenvironment is critical to successfully create a reliable drug testing system.
Human tissue is structurally diverse; characteristically, it contains a 3D microarchitecture that encompasses cells, an extracellular matrix, and signaling molecules [3]. In vitro this used to be difficult to accomplish but with recent advances in cell scaffolding biomaterials that provide a template for cell culture and mimic important features of the ECM, this becomes much more realistic [3]. Key components of an ECM include chemically modified hyaluronan, glycosaminoglycans, and ECM polypeptides containing thiol residues [4].
Extracel, for example, a commercially available hydrogel, provides an ECM template that offers a translational relationship between in vitro and in vivo experiments [4]. This biomimetic material has been used to promote the growth of healthy 3D tissues whether in vivo or in vitro; it has been tested with cell-line derived cells, endothelial and epithelial cells, fibroblasts, chondrocytes, hepatocytes among many others [4]. With Extracel, primary hepatocytes have been shown to retain their phenotypes and survive longer which is important to understand drug efficacy and toxicity within the human body [4]. This biomaterial overall provides a versatile in vitro structure for facilitating drug discovery and research [4].
Recently, through a growing number of studies, it has become more apparent that the ECM is not only important structurally but it also provides a framework of organized communication between cells embedded within the matrix [2]. Some studies have indicated that within specific in vitro cell cultures, target-specific signaling pathways may not always be active; this activity and predictability of cell cultures depends greatly on the quality of the cell culture system, thus displaying the importance of culturing cells in such a way that corresponds to an in vivo environment [5].
A limitation or challenge often faced in cell scaffolding remains to be the way in which cells are organized; it is common for cells in vivo to be (heterogeneously) mixed and arranged in such a way that contributes to their overall physiological role [3]. Currently, a new method of approaching cell organization is called “bottom-up tissue engineering” where small modular building blocks, which may be cell-entrapped or micro-engineered, are assembled together [3]. This strategy mimics the native microstructural functional units in vivo resulting in a more reflective microenvironment [6]. In comparison, the traditional method of tissue engineering employs a “top-down approach” where cells are seeded into a polymeric scaffold; from here, they are expected to populate the scaffold and create the correct ECM [6]. Although this method allows for a greater degree of biomimetic scaffolding, it often lacks the intricacies and features found within the tissues [6]. While the “bottom-up tissue engineering” method presents a powerful tool to tailor the structure and composition of the cell culture, this technique takes place largely on the macroscale (in millimeters or larger) [3].
Hydrogels in Cell Culture
To bridge the gap between in vitro and in vivo microenvironments, biomaterials often play a crucial role in replicating complexity into cellular systems [19]. With numerous biomaterials such as fibrillar foams or glass substrates, hydrogels have recently emerged as a promising technology. Hydrogels share properties similar to soft tissues; they also support cell adhesion and can mimic the majority of ECM elements [19].
The conventional model of 2D cell cultures involved placing cells upon a flat and stiff surface often resulting in aberrant phenotypes or other flawed cells [19]. A slightly newer approach for 2D cell culture involves placing cells upon a hydrogel film which does allow for a more tunable (substrate) stiffness and adhesivity but at the expense of drawbacks shared with the conventional approach [19]. The most optimal model involves 3D hydrogels interwoven with cell culture as this method is the most faithful to the microenvironment. A notable example that accentuates the differences between 2D and 3D cell culture was done by the Bissell lab; they demonstrated that human epithelial cells develop like tumor cells when placed upon a 2D surface, while the cells cultured within a 3D membrane-derived hydrogel grew normally [20].
Of the various materials that hydrogels can be produced from (collagen, fibrin, synthetic polymers, etc.), polyethylene glycol (PEG) appears to be quite versatile and overall advantageous; aside from its inertness and hydrophobicity, it can be modified and customized with other functional groups and offers low protein fouling [19]. PEG-based hydrogels, for example, were used to mimic the invasive characteristics of the ECM; Lutolf et al. were able to demonstrate that fibroblasts can invade this synthetic material (along with the help of matrix proteinases) and break it down (which in vivo would typically enable tissue regeneration) [22]. Another interesting application of hydrogels is that researchers were able to develop synthetic biomimetic hydrogels that promoted and allowed for rapid angiogenesis [23].
An interesting property of hydrogels is their level of customizability and overall versatility. For example, Loebel et al. were able to utilize the shear-thinning and self-healing properties of hydrogels to create injectable therapeutics [21]. As specific hydrogels are biomimetic, they were able to show that their hydrogel design (when injected) was useful for delivering not only cells into highly vascularized areas but also for drugs [21].
Cell Immobilization

Another issue to account for in device preparation involves cell immobilization within a specific area or compartment of a microfluidic device. Cell immobilization ensures that the cell samples can be exposed to the tested drug uniformly and analyzed properly [3]. Typically, cell immobilization falls into one of the following categories: adhesion of cells upon a substrate, entrapment of cells within a polymeric material, or the capturing of cells behind a membrane [3].
Within a 2D cell culture, it has been noted that the adhesion and proliferation of cells depend on the surface topology, wettability, microstructure, chemistry, and charge [7-11]. To maintain greater control over these factors, ECM proteins such as collagen, fibronectin, and laminin are often used to enhance cell adhesion.
Similarly, another technique that can be used is micropatterning [3]. This typically falls into one of two categories: seeding of cells upon a chemically patterned surface with various cell adhesions or seeding of cells onto a surface that varies topographically [3]. Moreover, micropatterning is often achieved through microcontact printing which involves images that can be transferred to a substrate (in high resolution) [3].
For 3D cell cultures, although all of the 2D techniques are applicable and widely researched, the most common technique involves using a hydrogel for cell immobilization. This method requires mixing hydrogel suspensions and cells together; from here, this mixture can go through gelation [3].

PDMS in Microfluidic Cell Culture
Polydimethylsiloxane, or PDMS, is the material mainly used in microfluidic devices, and so its applications and use in microfluidic cell culture are very important. One major benefit of PDMS is that it is gas permeable, and so aerobic cells can receive oxygen without an oxygen supply fed directly into the system. One study, described below, found that Hepatocarcinoma liver cells grown in a 3D microfluidic device composed of two stacked layers of PDMS successfully adhered to and colonize on the PDMS until they reached confluence. Another major benefit of the PDMS device discussed in this paper was the ability to create organized microfluidic channels that were able to continuously supply nutrients to the cells, which is crucial for promoting cell growth. The paper also mentions PDMS’ cheap price and biocompatibility. Additionally, PDMS is clear, allowing for easy use of a microscope to observe the colonized cells [29],[30]. PDMS is also easily sealed to itself via a plasma oxidation procedure, and therefore does not require an adhesive, which is extremely beneficial when working on micro length scales [33].
In order to prepare a microfluidic device for cell culture, the PDMS elastomer base was mixed with its curing reagent in a 10:1 ratio by mass, and then poured onto a previously prepared mold. It is then degassed in a vacuum chamber multiple times to remove all present air bubbles, heat-cured, and then removed from the mold. In one specific paper, in which two stacked layers of PDMS were used to make the device, an O2 plasma treatment was used to bond the two PDMS layers together. One important benefit of this process is that it changes the surface properties of the PDMS as well: the plasma treatment causes the walls inside the device to become hydrophilic, without which, a hydrophilic media cannot be introduced into the structure [29]. However, this is not a permanent process, and air can cause the PDMS to become hydrophobic again [33]. This hydrophilic media is necessary for providing nutrients to the cultured cells. However, this plasma treatment is not enough to cause cells to consistently adhere to the device, and therefore a collagen coating on the walls of the device was used to allow for better cellular adhesion to the device. Prior to the addition of cells, the PDMS device must be autoclaved, in order to ensure that the device is sterile. It is then washed with phosphate-buffered saline (PBS), as well as a culture medium (this particular study used DMEM supplemented with 10% fetal bovine serum). Without both of these mediums present in the device, the cells would be unable to easily adhere to the PDMS. As long as the culture is changed within the device so that the cells have access to nutrients, the cellular culture exhibits the expected activity. [29]
This same paper tested three different types of sterilization methods for the device: an ethanol solution, using ethylene oxide, and autoclaving for twenty minutes. It found that with the ethanol solution, four kinds of solutions had to be used for proper sterilization and cleaning of the device, and reported that using this many fluids had a high risk of contamination due to having to connect and remove tubes from the device constantly [29]. For the ethylene oxide sterilization method, the microfluidic device was placed in a chamber in which gaseous ethylene oxide was present, and then the chamber’s pressure was continuously moduled. The paper found that this technique caused the plasma bonding between the two PDMS layers to deteriorate, and thus the device could not be used [29].
Cons of PDMS in Cell Culture
A separate study looked at two potential problems with using PDMS for cell culture: uncured oligomers from the elastomer base leaching into the media flowing through the device, which could be toxic for cells, and the PDMS polymer absorbing hydrophobic molecules such as estrogen from the serum into the device. It found that uncured oligomers could be detected in PDMS devices both before and after Soxhlet extraction in ethanol, that these oligomers could also be detected in the plasma membranes of cells cultured within PDMS for 24 hours, that hydrophobic molecules such as estrogen were much more likely (a ratio of 9:1) to diffuse into the surrounding PDMS than into cells, and that pretreating the PDMS with a serum or pre-absorbing estrogen into the device did not prevent estrogen from diffusing into the device [30]. The paper also discusses previous techniques used to remove these uncrosslinked oligomers, which are present even after extensive curing at high temperatures over long periods of time, such as Soxhlet extraction, extractions in organic solvents, and longer baking times. It is worth noting that the solvent used in this paper, ethanol, is a poor choice, as PDMS is much less soluble in ethanol than it is in more organic solvents, such as toluene. However, solvents such as toluene are quite toxic, and must be extensively removed from the PDMS prior to cell culture.
Prior to using ethanol to remove these uncrosslinked oligomers, the paper tested to see if they would diffuse into solution. It found that when water, the base solvent for most culture media, was incubated for a twenty four hour period in the microfluidic device, uncrosslinked oligomers were found to be present in the water via mass spectrometry. The paper made a point of mentioning that this is could invalidate the supposed biological inertness and biocompatibility of PDMS, as the interactions that could occur between these uncrosslinked oligomers and components of culture media have, as well as interactions between these oligomers and cells, have yet to be studied in depth [30]. However, the paper also points out that at the time of its publication, there had been no direct published evidence correlating uncrosslinked PDMS oligomers and cell stress [30].
One of the main pros of PDMS is that it is highly permeable, which lets oxygen diffuse through for aerobic cell culture. However, the same properties that allow for oxygen diffusion can also lead to the diffusion of water vapor, which can cause culture mediums to lose water content upon flowing through the device [31]. Additionally, as briefly discussed in the prior paragraphs, hydrophobic molecules such as hormones can be absorbed by the PDMS, which is an especially big problem when these molecules are only present in very small concentrations in the culture medium. Additionally, it is difficult to predict how much of these molecules the PDMS will absorb, due to the variance of pH and ions in complex media [31]. This absorption is also a serious problem for using PDMS as in cell culture devices because it can absorb molecules necessary for cellular signaling [33]. This can also have ramifications in drug screening, especially when the exact quantity of drug being used is of paramount importance [33].
Anaerobic Cell Culture in PDMS
Due to the oxygen permeability of PDMS, one may expect that it could be difficult to culture anaerobic cells in PDMS-based microfluidic devices. However, one paper demonstrated that the dissolved oxygen levels present in the device can be easily modulated to their desired levels for a particular cell culture by flowing a mixture of oxygen and nitrogen through dedicated gas channels in the device that are close to the fluid filled channels. Due to diffusion, this technique is able to regulate the oxygen concentration within the device with a high degree of control. Within these channels, modulating the relative flow rates of oxygen and nitrogen can be used to finely tune the oxygen concentration, generating local varied concentrations of oxygen within the device, and thus allowing for the culture of cells that are both anaerobic and aerobic within the same device (in different channels) [34].
Scale-Up of PDMS in Microfluidic Cell Culture
In a later study, the same group described previously for their work with Hepatocarcinoma liver cells demonstrated that these same cells clustered and self organized within a PDMS bioreactor designed for cultures on a larger scale. They successfully created a microfluidic bioreactor made out of ten sheets of PDMS that had comparable output to that of industrial macroscale bioreactors [32]. To do so, an oxygen chamber was inserted between the PDMS layers, to ensure proper oxygen diffusion within the device. The device was constructed via replica molding using a negative master, and the PDMS layers were aligned through optical microscopy. No measurements were made with respect to uncrosslinked oligomers appearing in the cell. Prior to culture, the device was sterilized via autoclave, after which all microfluidic channels are coated with a collagen solution, which was then rinsed with excess PBS prior to the addition of cells and the cell culture media [32].
Alternative Materials for Microfluidic Cell Culture
Due to the cons discussed above, it is possible that PDMS is not the best material to use in microfluidic cell culture, despite the positive properties associated with it. One alternative is photocurable perfluoropolyethers (PFPEs), which are fluoropolymers that are liquids at room temperature but can be photocured for applications in microfluidics. PFPEs are fluorinated, carbon based polyethers that do not have hydrogens present in the material. Some of the benefits associated with these materials are low surface energy, a low Young's Modulus, high gas permeability similar to that of PDMS, low toxicity, and resistance to chemicals that cause PDMS to swell and deform [33]. Fluorinated PDMS is also an option, although this is more expensive than regular PDMS and has yet to be studied in a microfluidic cell culture environment. A third alternative is a polymer called cyclic olefin copolymer (COC), which is a mixture of two different polymers and therefore has highly tunable properties. This polymer is sold commercially under the name Topas, and is approved by the Food and Drug Administration as biocompatible [33].
Motivation Behind Microfluidic Cell Culture
As discussed in the above sections, two dimensional cell cultures are unable to give accurate models of how cells differentiate in vivo, nor to predict the effect that drugs will have in vivo. In the past, scientists have therefore turned to animal testing as a more accurate prediction method, but besides the ethical issues associated with it, animal testing is not necessarily a good predictor for how humans will react to a drug [12]. In fact, only 13.8 % of all tested drugs actually end up successful in clinical trials and are approved by the FDA [18]. Because of this, there has been a push over the last few decades to create an accurate prediction mechanism for how drugs will interact with and affect humans. Many three dimensional cell culture techniques have been developed, but these have their drawbacks. They are unable to account for variation in organoid size and shape, and are unstable over long periods of time. Many are also unable to model tissue - tissue interfaces, and cells within these models are not usually exposed to the mechanical forces and cues that they would feel in the body. These cues play a critical role in organ development, structure, and function, and it has been very difficult to accurately create an organ model that properly mimics morphogenesis, or the act of cells differentiating and self assembling into complex organs and organoids [13],[14].
Recent developments in the field however, have led to major advances in organ and organoid modeling. These advances have incredibly powerful applications, such as in personalized medicine, drug development, and understanding how diseases affect humans at the cellular level.
Organ-On-A-Chip
The concept of an organ-on-a-chip is something that has been developed over the last two decades, and has broad based applications. Organs-on-chips are essentially cultured cells living in microfluidic devices that are able to model the physiological function of tissues and organs with remarkable accuracy. They are not organoids; organs-on-chips have minimal functional units for simplicity, and are not perfect models of in vivo organs. That being said, however, they are one of the most accurate prediction mechanisms currently known for studying disease progression, how drugs interact with diseases, and how organs develop and grow as cells differentiate.They can range in complexity from single chamber units that contain only one type of cultured cell that can be used to model one tissue type, to multiple channels connected via membrane which are able to model tissue interfaces. Recently, the concept of linking together multiple organs-on-chips has been used to model more complicated organ systems as well.
Cell Culture Within Organs-On-Chips
Most organs-on-chips are made using soft lithography, in a manner very similar to most microfluidic devices. Polydimethylsiloxane, or PDMS, is poured onto an etched silica substrate, so that the inverse of the pattern on the substrate is stamped into the PDMS. The PDMS is then removed from the silica chip and bound to a glass substrate, creating microfluidic channels within the PDMS for fluid flow. The surface of the microfluidic channels within the device are then coated with proteins found in the extracellular matrix such as laminin, as these proteins promote the adhesion of anchorage dependent cells to substrates. These proteins therefore act as ‘binding sites’ for the cells. Cells are then flowed through the channel so that they are able to adhere to the ‘ECM substrate,’ and culture medium is then continuously passed through the channel, so that the cells have a constant food source [16].
Major Benefits of Organs-On-Chips
One extremely important benefit of organs-on-chips is that they are able to incorporate physical forces, such as shear stress, mechanical compression, and cyclic strain, as well as provide easy analysis of how the organ responds. An example of this is that an organ-on-a-chip used to model the lung can use stresses to model breathing, which is a critical part of how the lung functions, and therefore plays a very important role in the environment that cells in the lung experience [15]. An example of this is shown in Figure 6, where vacuum channels on either side of the chip allow the lung to “breathe.”

PDMS is also a clear material, which allows for high resolution imaging of cellular responses to various stimuli and changes in the environment. Additionally, flow in microfluidic devices is laminar, which allows for the generation of physical and chemical gradients [14]. This is extremely powerful and has broad reaching applications within cells, allowing for the control and analysis of tissue formation and cell differentiation. Additionally, exterior stresses can be controlled independently of these gradients, which can further modulate the cell’s environment and make the organ-on-a-chip as realistic a model as possible [14].
Another important aspect is that porous substrates can be added to the devices that have the ability to act as a barrier between two channels, allowing for the analysis of barriers between tissues. Using this method, one can create tissue-tissue interfaces which are able to model the interactions of vascular endothelium and parenchymal tissues, which are an extremely important component of almost all organs [17].
Organs-On-Chips In Series
One major advancement in this field is the concept of linking together multiple organs-on-chips in order to model larger organ systems, such as the gastrointestinal tract. Multiple organs-on-chips can be linked through sequential transfers of a common blood substitute done robotically via their endothelium lined channels. For example, by linking chips that model gut, liver and kidney function, first pass drug absorption and metabolism can be pharmacokinetically modeled [18]. In fact, in January of 2020, a DARPA funded project based out of the Wyss Institute at Harvard University introduced the concept of a body-on-a-chip, which is able to model the interactions between ten different organs, as shown in the schematic in Figure 7. This could theoretically be used to monitor how drugs affect the entire body, and could be used for high throughput screening of drugs in the future. Additionally, if the ten different organs-on-chips used had cells grown from a particular patient, they could be used to test how a specific patient will react to different types of treatment, allowing for quick, inexpensive testing of many different drugs on a single individual at once if experiments are run in parallel. This has the potential to lead to major advances in personalized medicine.

Conclusion
Current drug testing techniques are relatively inaccurate, and so it can take years for potentially life saving drugs to come to market. Additionally, current drug testing techniques require animal testing prior to entering clinical trials, which is ethically questionable at best, and is not a good predictor of how drugs will affect humans. Cell culture in microfluidic devices has the potential to fix this problem, allowing for accurate, high throughput, and inexpensive drug screening. These techniques can also be used to study disease progression and treatment mechanisms, which could lead to major therapeutic advances in a variety of fields. Although this is a relatively new technique, it shows large amounts of promise as an accurate model for the human body.
References
1. Halldorsson, S., Lucumi, E., Gómez-Sjöberg, R., & Fleming, R. M. T. (2015). Advantages and challenges of microfluidic cell culture in polydimethylsiloxane devices. Biosensors and Bioelectronics, 63, 218–231. https://doi.org/10.1016/j.bios.2014.07.029
2. Sun, T., Jackson, S., Haycock, J. W., & MacNeil, S. (2006). Culture of skin cells in 3D rather than 2D improves their ability to survive exposure to cytotoxic agents. Journal of Biotechnology, 122(3), 372–381. https://doi.org/10.1016/j.jbiotec.2005.12.021
3. Wu, M.-H., Huang, S.-B., & Lee, G.-B. (2010). Microfluidic cell culture systems for drug research. Lab on a Chip, 10(8), 939. https://doi.org/10.1039/b921695b
4. Prestwich, G. D. (2008). Evaluating Drug Efficacy and Toxicology in Three Dimensions: Using Synthetic Extracellular Matrices in Drug Discovery. Accounts of Chemical Research, 41(1), 139–148. https://doi.org/10.1021/ar7000827
5. Bhadriraju, K., & Chen, C. S. (2002). Engineering cellular microenvironments to improve cell-based drug testing. Drug Discovery Today, 7(11), 612–620. https://doi.org/10.1016/s1359-6446(02)02273-0
6. Nichol, J. W., & Khademhosseini, A. (2009). Modular tissue engineering: engineering biological tissues from the bottom up. Soft Matter, 5(7), 1312. https://doi.org/10.1039/b814285h
7. Rosa, A. L., & Beloti, M. M. (2003). Rat bone marrow cell response to titanium and titanium alloy with different surface roughness. Clinical Oral Implants Research, 14(1), 43–48. https://doi.org/10.1034/j.1600-0501.2003.140106.x
8. Khorasani, M. ., & Mirzadeh, H. (2004). BHK cells behaviour on laser treated polydimethylsiloxane surface. Colloids and Surfaces B: Biointerfaces, 35(1), 67–71. https://doi.org/10.1016/j.colsurfb.2004.01.011
9. Mata, A., Boehm, C., Fleischman, A. J., Muschler, G., & Roy, S. (2002). Growth of connective tissue progenitor cells on microtextured polydimethylsiloxane surfaces. Journal of Biomedical Materials Research, 62(4), 499–506. https://doi.org/10.1002/jbm.10353
10. Peterson, S. L., McDonald, A., Gourley, P. L., & Sasaki, D. Y. (2004). Poly(dimethylsiloxane) thin films as biocompatible coatings for microfluidic devices: Cell culture and flow studies with glial cells. Journal of Biomedical Materials Research, 72A(1), 10–18. https://doi.org/10.1002/jbm.a.30166
11. Webb, K., Hlady, V., & Tresco, P. A. (1998). Relative importance of surface wettability and charged functional groups on NIH 3T3 fibroblast attachment, spreading, and cytoskeletal organization. Journal of Biomedical Materials Research, 41(3), 422–430. https://doi.org/10.1002/(sici)1097-4636(19980905)41:3<422::aid-jbm12>3.0.co;2-k
12. Greek, Ray, and Andre Menache. “Systematic reviews of animal models: methodology versus epistemology.” International journal of medical sciences vol. 10,3 (2013): 206-21. https://doi.org/10.7150/ijms.5529
13. Mammoto, T., Mammoto, A. & Ingber, D.E. Mechanobiology and developmental control. Annu. Rev. Cell Dev. Biol. 29, 27–61 (2013). httpsL//doi.org/10.1146/annurev-cellbio-101512-122340.
14. Ingber, D.E. Mechanobiology and diseases of mechanotransduction. Ann. Med. 35, 564–577 (2003). https://doi.org/10.1080/07853890310016333
15. Bhatia SN, Ingber DE. Microfluidic organs-on-chips. Nat Biotechnol. 2014;32:760–772. https://doi.org/10.1038/nbt.2989.
16. Kane, R.S., Takayama, S., Ostuni, E., Ingber, D.E. & Whitesides, G.M. Patterning proteins and cells using soft lithography. Biomaterials 20, 2363–2376 (1999). https://doi.org/10.1016/s0142-9612(99)00165-9
17. Huh, D. et al. Reconstituting organ-level lung functions on a chip. Science 328, 1662–1668 (2010) https://doi.org/10.1126/science.1188302
18. Herland, A., Maoz, B.M., Das, D. et al. Quantitative prediction of human pharmacokinetic responses to drugs via fluidically coupled vascularized organ chips. Nat Biomed Eng (2020). https://doi.org/10.1038/s41551-019-0498-9
19. Caliari, S. R., & Burdick, J. A. (2016). A practical guide to hydrogels for cell culture. Nature Methods, 13(5), 405–414. https://doi.org/10.1038/nmeth.3839
20. Li, X., Sun, Q., Li, Q., Kawazoe, N., & Chen, G. (2018). Functional Hydrogels With Tunable Structures and Properties for Tissue Engineering Applications. Frontiers in Chemistry, 6. https://doi.org/10.3389/fchem.2018.00499
21. Loebel, C., Rodell, C. B., Chen, M. H., & Burdick, J. A. (2017). Shear-thinning and self-healing hydrogels as injectable therapeutics and for 3D-printing. Nature Protocols, 12(8), 1521–1541. https://doi.org/10.1038/nprot.2017.053
22. Lutolf, M. P., Lauer-Fields, J. L., Schmoekel, H. G., Metters, A. T., Weber, F. E., Fields, G. B., & Hubbell, J. A. (2003). Synthetic matrix metalloproteinase-sensitive hydrogels for the conduction of tissue regeneration: Engineering cell-invasion characteristics. Proceedings of the National Academy of Sciences, 100(9), 5413–5418. https://doi.org/10.1073/pnas.0737381100
23. Moon, J. J., Saik, J. E., Poché, R. A., Leslie-Barbick, J. E., Lee, S.-H., Smith, A. A., Dickinson, M. E., & West, J. L. (2010). Biomimetic hydrogels with pro-angiogenic properties. Biomaterials, 31(14), 3840–3847. https://doi.org/10.1016/j.biomaterials.2010.01.104
24. Edmondson, R., Broglie, J. J., Adcock, A. F., & Yang, L. (2014). Three-Dimensional Cell Culture Systems and Their Applications in Drug Discovery and Cell-Based Biosensors. ASSAY and Drug Development Technologies, 12(4), 207–218. https://doi.org/10.1089/adt.2014.573
25. Breslin, S., & O’Driscoll, L. (2013). Three-dimensional cell culture: the missing link in drug discovery. Drug Discovery Today, 18(5–6), 240–249. https://doi.org/10.1016/j.drudis.2012.10.003
26. Wells, R. G. (2008). The role of matrix stiffness in regulating cell behavior. Hepatology, 47(4), 1394–1400. https://doi.org/10.1002/hep.22193
27. Sun, M., Chi, G., Li, P., Lv, S., Xu, J., Xu, Z., … Li, Y. (2018). Effects of Matrix Stiffness on the Morphology, Adhesion, Proliferation and Osteogenic Differentiation of Mesenchymal Stem Cells. International Journal of Medical Sciences, 15(3), 257–268. https://doi.org/10.7150/ijms.21620
28. Mabry, K. M., Lawrence, R. L., & Anseth, K. S. (2015). Dynamic stiffening of poly(ethylene glycol)-based hydrogels to direct valvular interstitial cell phenotype in a three-dimensional environment. Biomaterials, 49, 47–56. https://doi.org/10.1016/j.biomaterials.2015.01.047
29. Leclerc, E., Sakai, Y. & Fujii, T. Cell Culture in 3-Dimensional Microfluidic Structure of PDMS (polydimethylsiloxane). Biomedical Microdevices 5, 109–114 (2003). https://doi.org/10.1023/A:1024583026925
30. K. J. Regehr, M. Domenech, J. T. Koepsel, K. C. Carver, S. J. Ellison-Zelski, W. L. Murphy, L. A. Schuler, E. T. Alarid, and D. J. Beebe, “Biological implications of polydimethylsiloxane-based microfluidic cell culture,” Lab on a Chip, vol. 9, no. 15, p. 2132, 2009. https://doi.org/10.1039/B903043C
31. M. W. Toepke and D. J. Beebe, “PDMS absorption of small molecules and consequences in microfluidic applications,” Lab on a Chip, vol. 6, no. 12, p. 1484, 2006. https://doi.org/10.1039/B612140C
32. Leclerc, E., Sakai, Y. and Fujii, T. (2004), Microfluidic PDMS (Polydimethylsiloxane) Bioreactor for Large‐Scale Culture of Hepatocytes. Biotechnol Progress, 20: 750-755. https://doi.org/10.1021/bp0300568
33. Rajendrani Mukhopadhyay, “When PDMS isn't the best,” When PDMS isn't the best | Analytical Chemistry. [Online]. Available: https://pubs.acs.org/doi/10.1021/ac071903e. [Accessed: 19-Apr-2020].
34. Anal. Chem. 2009, 81, 14, 5918-5924. Publication Date: June 11, 2009 https://doi.org/10.1021/ac9006864
