BME100 f2013:W900 Group4 L3
| Home People Lab Write-Up 1 | Lab Write-Up 2 | Lab Write-Up 3 Lab Write-Up 4 | Lab Write-Up 5 | Lab Write-Up 6 Course Logistics For Instructors Photos Wiki Editing Help | ||||||
|
OUR TEAM
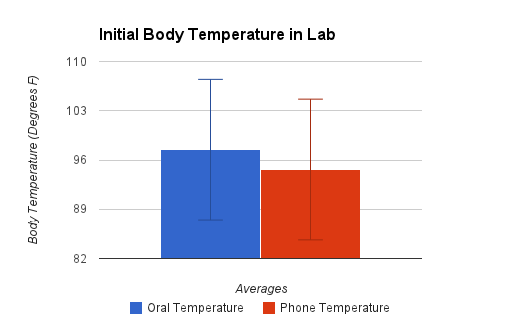
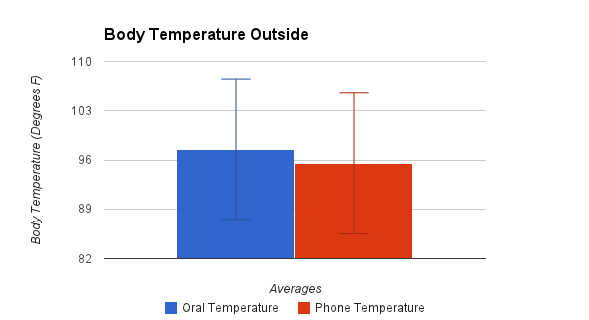
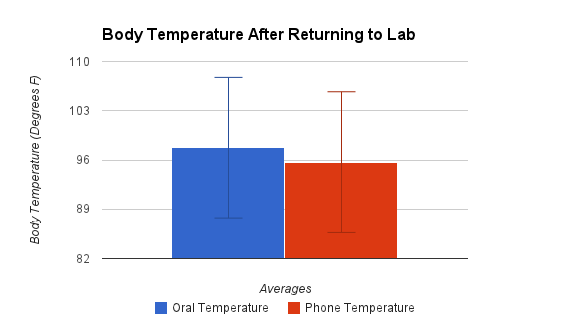
LAB 3A WRITE-UPDescriptive StatisticsIn order to evaluate an Iphone app, Vitals Monitor, which records temperature through an external sensor, the lab groups recorded temperature readings every five minutes first inside in order to get a base reading and to verify signal between the sensor and the Iphone. The groups then proceeded to take temperature readings every five minutes outside, and then upon returning inside again. These temperature readings were performed using both the Iphone sensor as well as an oral thermometer, which served as a control. For the initial inside readings, the groups each measured a total of five temperature values and the average came out to be 97.46 degrees F with a standard deviation of 1.485 degrees F for the oral thermometer and an average of 94.65 degrees F with a standard deviation of 3.748 degrees F for the Iphone sensor. Upon moving outside after issues described in the summary, twelve temperature readings were recorded every five minutes. The average and standard deviation for the oral and Iphone sensors respectively was 97.497 +/- 1.838 degrees F and 95.55 +/- 1.485 degrees F. After finishing outside recordings, the groups made their way back inside and a final set of five temperature readings was made every five minutes, again using both the oral and Iphone sensors. The average and standard deviation for the oral thermometer was found to be 97.743 +/- 0.566 degrees F and the average and standard deviation for the Iphone sensor was found to be 95.7 +/- 1.697 degrees F. The p-value results for a t-test comparing the inside readings for each sensor prior to going outside was found to be 9.02695E-26. The p-value comparing the results for the outside temperature readings for each sensor was found to be 1.43722E-39. The p-value comparing the temperature readings after coming back inside for each sensor was found to be 1.05598E-25.
Results
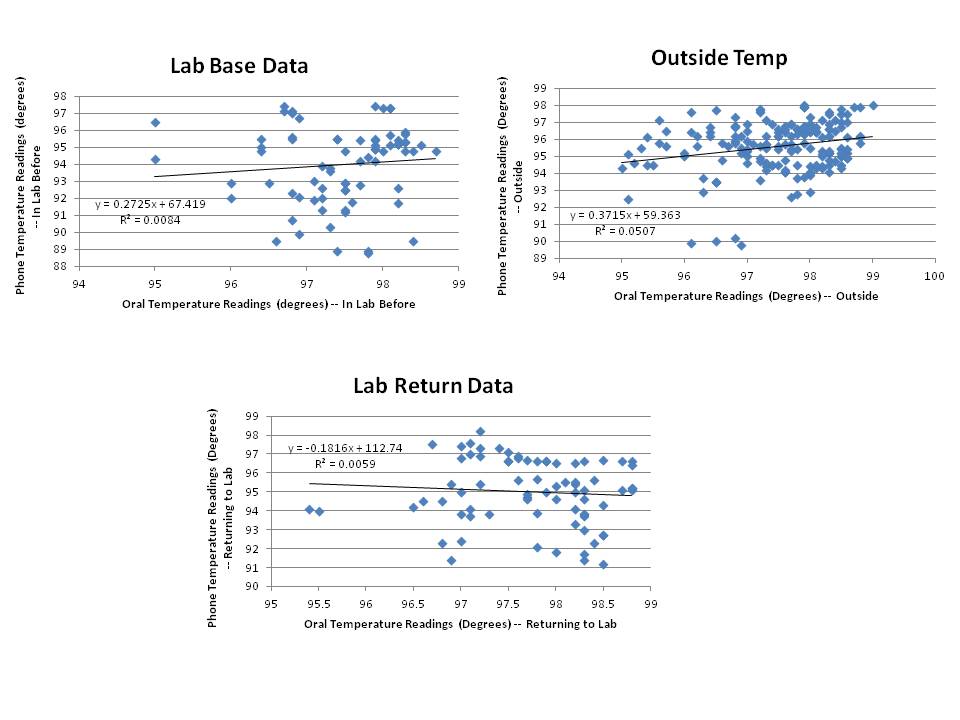
Analysis & Inferential StatisticsDue to the fact that the data showed p-values across the board that were less than 0.05, it can be inferred that the recordings being retrieved by the oral thermometer are statistically similar to the recordings given by the underarm sensor. Although the data is statistically significant according to the t-test probability values, a further analysis of the linear regression can be seen in the plots below. The r-values determined from the linear regression are 0.0084 for the temperatures in the lab prior to going outside, 0.0507 for the outside temperatures and 0.0059 upon returning to lab. These values are much closer to 0 than they are to 1 which indicates that the correlation between the oral and underarm temperature readings is weak even if it statistically significant. When applied to the entire population, it could potentially be inferred that there would be weak statistical significance between the two sets of data under each of the conditions; however, it should be noted that with a larger data set, there may be some variation and correction to the current data especially considering some of the complications in connecting to the device.
Summary/DiscussionThe sensor had a lot of difficulty in functioning properly. The device was erratic and the signal easily broke when distance was created between the phone and the sensor. It also took several readings in the initial stages of recording data to reach a reasonable body temperature for an adult human. Interference between devices was common. Our group had to combine with another group because our iPhone was registering the Bluetooth for another group's device, and refused to pick up our own. Adding a cord connection from the iPhone jack to the sensor could create a direct connection and fix many of the problems associated with the wireless aspect of the device--the trade off to this would would be a loss of mobility. Our results, however, were fairly accurate. The t test p values were almost negligible, showing that our results were statistically significant. The r-values determined from the linear regression indicated that, although statistically significant, the correlation between the oral and underarm sensors was weak. Ignoring the Bluetooth and interference problems, the device recorded body temperature fairly well. With the oral thermometer being used as the accurate form of measurement, that would still be the recommended method of temperature measurement due to the low r-values when associated with the underarm sensor.
LAB 3B WRITE-UPTarget Population and Need
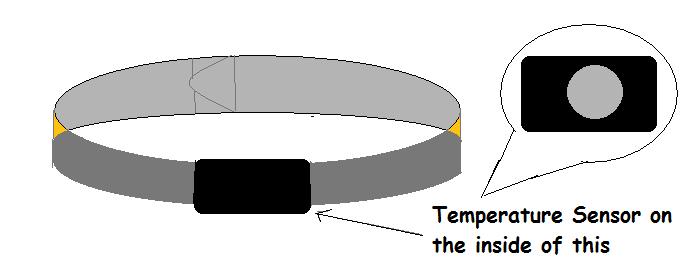
However, a recent innovation has potential to change the way doctors handle their patients after treatment. The HotWaist is designed to monitor body temperature of a patient by being strapped to the upper abdomen in a nonrestrictive, comfortable way and consistently monitors thermal changes in the patients body. Coupled with a wifi connection, the Hotwaist gives doctors the ability to monitor the patient in the comfort of the patients home, which is proven to be the best place for recovery due to its comfortable, familiar setting. The HotWaist is here to make a drastic change in the way outpatient care is conducted. Device DesignThe Hot Waist is a sensor disguised as a waste band that can that can be used to determine body temperature and heart rate. It is made out of an adjustable elastic band that can be worn around comfortably without any restrictions. The sensor is able to connect to a cellular device that acts as a private mobile hot spot that is only able to be discovered by searching for it and entering a password to ensure readings that is undisturbed by other signals or people. The device features various themes that people may use to set their own fashion statement for a more satisfying experience using the Hot Waist. The band is placed around the upper abdomen is made to calibrate to the environment by taking the actual temperature of the surroundings and adapt to that temperature giving the Hot Waist an accurate temperature reading rather than the temperature on the body, under the shirt, and the surrounding environment. The band is wrapped with a special material that is able to stretch to any body size and and protect the mechanics from damage from sweat, accidental hits, and other detrimental events that can cause the sensor and the transmitter to be put into jeopardy. Since the Hot Waist emits a private wi-fi signal that can only be discovered by entering a code into the device that will receive the recordings, it will be a better rate of connection for reading the data. The starting price is at $60 and is worth the higher price when being put up against an oral thermometer and the Bluetooth sensor accompanied with the app. The Hot Waist is sold in stores and available for shipping. It is sold in a hard plastic case that can be reused and altered for other uses.
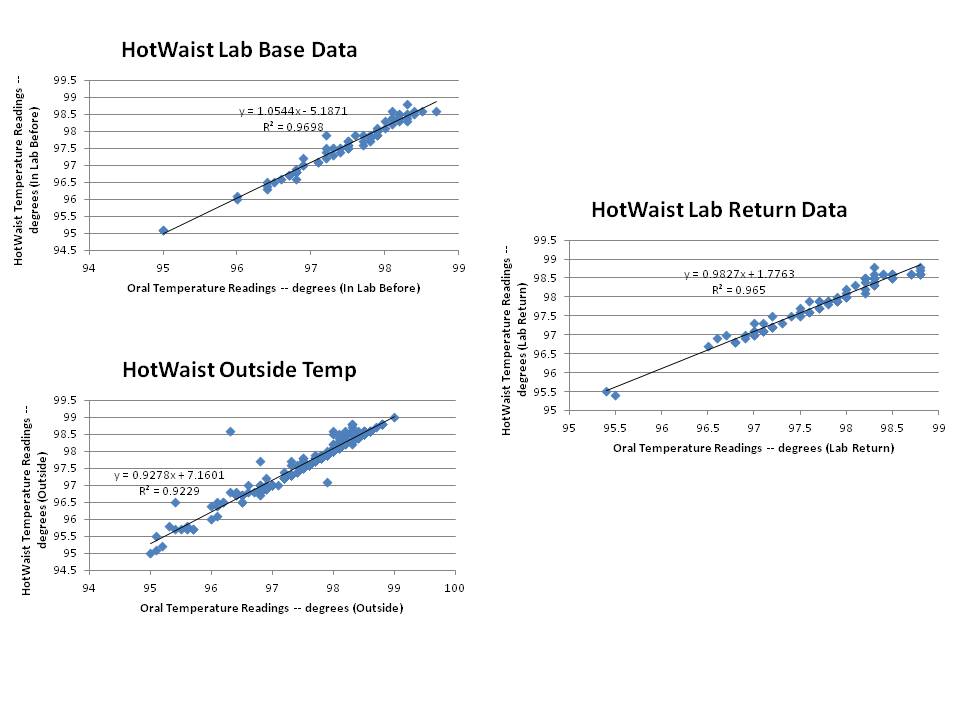
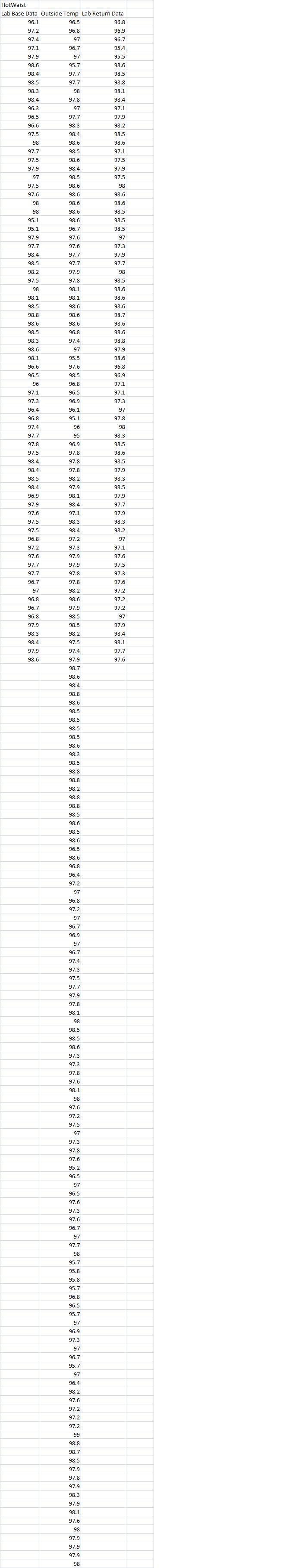
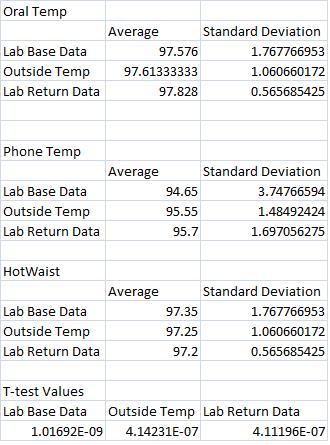
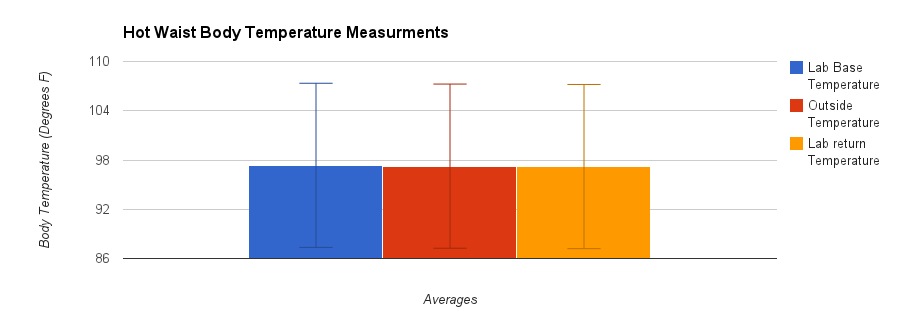
Inferential StatisticsBased on the data recorded from the HotWaist band, there is much more accuracy when compared to the underarm, Bluetooth sensor. When placed in a linear regression model with the underarm sensor, the r-values were very close to 0 showing that there was only a very low correlation between the oral temperature (the accurate model) and the underarm sensor. The HotWaist r-values show a very high correlation between the two which can lead to the inference that it will more accurately read temperature than the underarm sensor. The p-values found at the bottom of the data set also show that the readings for the oral thermometer and the HotWaist are statistically similar to one another as they are all below the alpha value of 0.05. As a result, for constant temperature measurement for an outpatient, the HotWaist is equally as accurate as an oral thermometer and more convenient because the patient can simply place the band around their waist and have temperature measurements being recorded discretely and on even intervals without having to remember to check using the oral thermometer.
Graph | ||||||