BME100 f2013:W1200 Group17 L3
| Home People Lab Write-Up 1 | Lab Write-Up 2 | Lab Write-Up 3 Lab Write-Up 4 | Lab Write-Up 5 | Lab Write-Up 6 Course Logistics For Instructors Photos Wiki Editing Help | |||||||
|
OUR TEAM
LAB 3A WRITE-UPDescriptive StatisticsContributed by Sonia Malek, Kevin Luong, Jason Yang, Andrew Prindle
ResultsContributed by Sonia Malek, Kevin Luong, Jason Yang, Andrew Prindle
AnalysisContributed by Sonia Malek, Kevin Luong, Jason Yang, Andrew Prindle
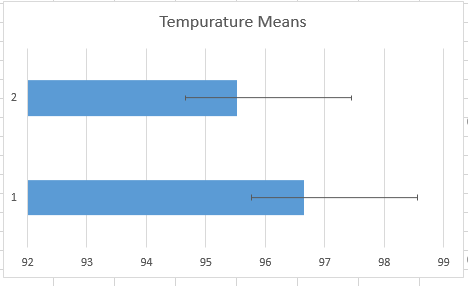
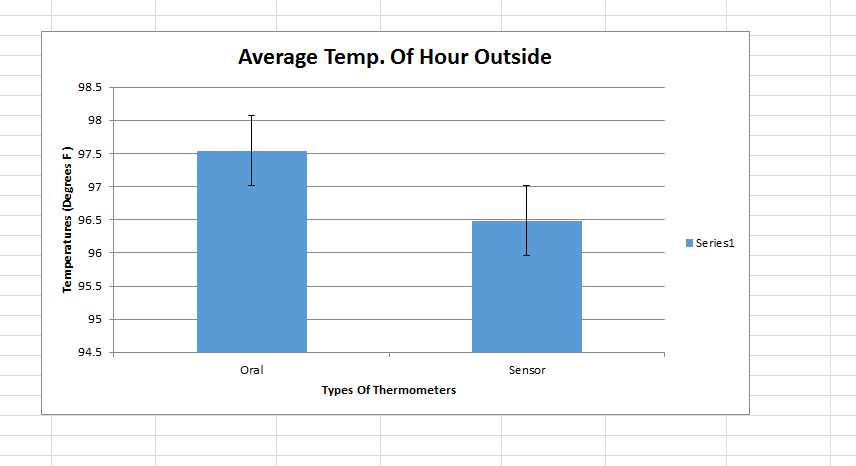
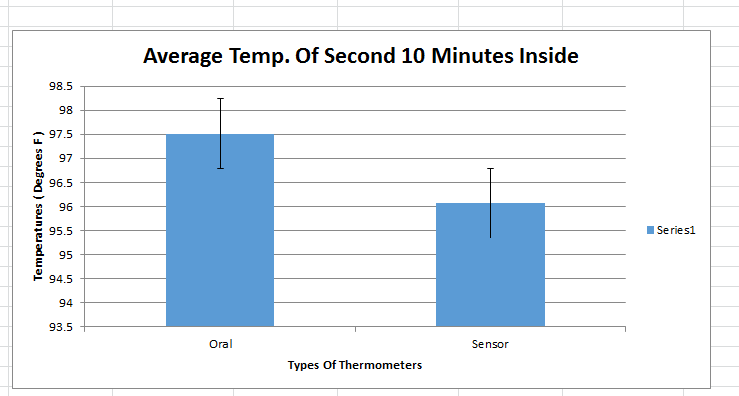
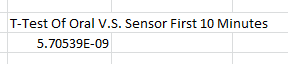
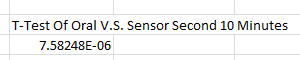
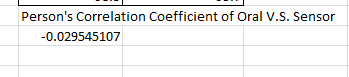
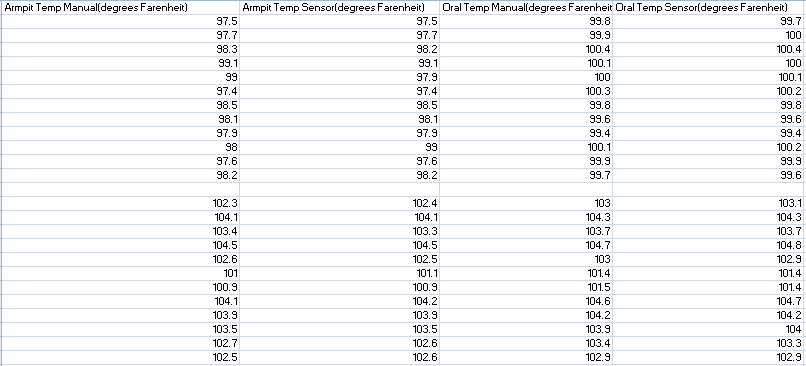
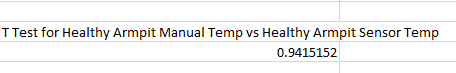
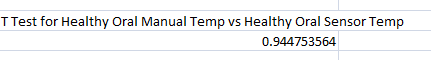
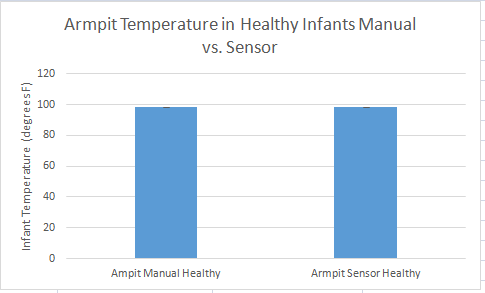
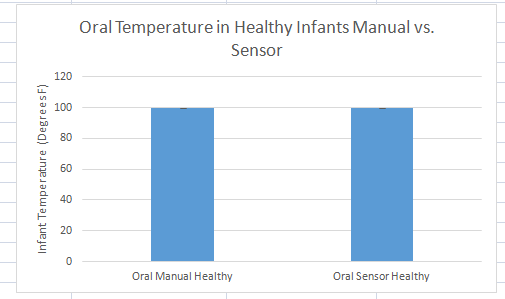
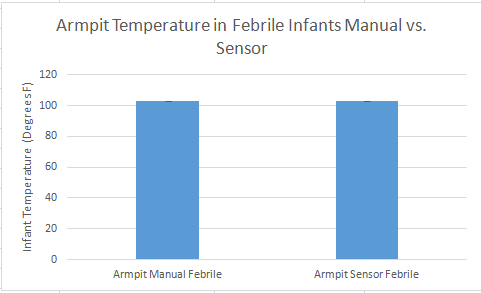
Summary/DiscussionThe goal of this experiment was to test the performance of the Raiing Wireless Thermometer. This includes analyzing device's ease of use, the speed with which it recorded data, and the accuracy and consistency of the temperatures it recorded. Overall, the Raiing thermometer was easy to set up and simple to operate. The device was paired with a bluetooth phone and operational within 15 minutes. Device quality is an issue, however, with 5 of the 18 purchased thermometers failing on the first day of use. Another device (group 17's) recorded data for the first 45 minutes of the experiement and then lost connection with the bluetooth device. The device was slow to report accurate data. It took over 15 minutes for the device to begin reporting data within a physiologic range. In order to test the accuracy and validity of the data, the temperature readings were compared to oral thermometer reading taken at the same time. Both indoor and outdoor conditions were tested. 5 readings, each two minutes apart, were initially taken indoors. After this an additional 12 readings were taken outdoors, each five minutes apart. Finally, the subject returned indoors and another 5 readings were taken in two minute increments. The data of 12 test subjects were aggregated and analyzed. We took the averages and standard deviations for both the oral and senor data sets in each of the three time periods. We noticed that the data was different and decided to do T-Tests to see whether the differences between the sensor data and oral data were statistically significant. All P-Values were well below the acceptable 0.05 value showing that the sensor and oral data were not the same. We also conducted a Pearson's Correlation Coefficient to see if there was a linear relationship between the two data sets. The 0.02 value showed that there was not. Our data reflects our experience with the Raiing Wireless Thermometer. The product was poorly made, slow to adjust to new environments, inefficient, and produced unreliable data. Contributed by Sonia Malek, Kevin Luong, Jason Yang, Andrew Prindle, Micke Cox
LAB 3B WRITE-UPTarget Population and NeedThe purpose of our device is to use our temperature sensor and accompanying smartphone app as a means for parents to remotely monitor the temperature of their newborn infants. The temperature sensors will be placed into both a thin disposable armband to be placed in the axilla, as well as into a pacifier for oral temperature readings. Temperature readings will be sent via bluetooth to nearby monitor, which then uploads the data wirelessly to the internet so it can be viewed from any smart device and/or computer by logging in to the parents' account on the device's website. This allows parents to check on the temperature of their babies from anywhere in the world. There is significant need and market demand for a device of this sort. Parents are busier than ever, making it difficult oftentimes to keep a constant eye on their sick infants. High fevers in infants, if left untreated, can lead to significant morbidities such as seizures and brain damage. High fevers in infants are an indicator of severe, potentially fatal, underlying illnesses that require medical attention. Early detection of a fever will lead to better, faster treatment of sick newborns. This device and program offers parental peace of mind and helps to provide better neonatal care.
Device Design
This image shows the pacifier component of the BabyTemp as well as the sensor component of the device. The bluetooth thermometer sensor is within the pacifier and is fundamental to the measurement of the baby's temperature. An additional black arm band contains a sensor that aids in the accurate reading of the baby's temperature.
br> Inferential Statistics
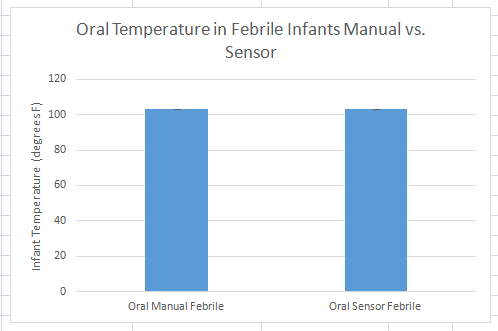
Graph
| |||||||