User:Johnsy/Lipoprotein Modelling/Cholesterol Homeostasis
Control of Cholesterol
Contol of the levels of cholesterol (intracellularlly and extracellularly) occurs through three different ways.
- Regulation of HMG-CoA reductase activity
- Regulation of LDL receptor synthesis
- Regulation of the esterification and removal of free cholesterol
The formation of new cholesterol from Acetyl-CoA or similar derivatives is commonly known as the de novo pathway as it utilizes fundamental building blocks such as acetyl-CoA instead of using preexisitng sterols and modifying side chains. Since HMG-CoA reductase is the rate limiting step of cholesterol biosynthesis, it is the main enzyme targeted first when controlling cholesterol biosynthesis. This control is achieved by two different methods. First, short-term regulation arises by allosteric inhibition of the enzyme, either competitively or non-competitively as well as covalent modification via phosphorylation at specific sites. Second, long-term regulatin is achieved by controlling the amount or concentration of enzyme in the cell. Long term feedback regulation of HMG-CoA reductase is the primary means of controlling the amount of enzyme in the cell. Negative feedback resulting from high or low levels of mevalonolactone (an intermediate that forms mevalonate) and LDL-cholesterol determines the levels of transcription of the gene responsible for HMG-CoA.
LDL intake is also another way of controlling the amount of cholesterol intracellularlly and extracellularly. LDL intake into the cell is regulated by receptors whose surface concentration is governed by the the intracellular levels of cholesterol. High concentrations of cholesterol supress the production and exposure of receptors while low concentrations of cholesterol act to enhance the production and exposure of receptors at the cell surface. LDL receptors are recycled, so this can method can act as both a short-term and long-term method of controlling the level of cholesterol and maintaining homeostasis. LDL receptor activity is responsible for controlling the homeostasis of cholesterol in the blood stream. The serum concentration of LDL depends on the rate tha tliver removes IDL from the circulation, which in turn depends on the number of functioning LDL receptors on the liver cell surface. Approximatley 75% of the LDL cleared from the plasma is removed by the liver and 25% by extra-hepatic tissues. Of this, 70% is cleared via LDL receptors, while the remaining 30% is cleared via non-receptor mediated pathways not regulated by cellular cholesterol levels.
Regulation of the esterification of cholesterol is governed by the enzyme acyl-CoA:cholesterol acyltransferase (ACAT). This enzyme is in turn regulated by reversible phosphorylation and by long-term control via protein synthesis methods. Increasing the activity of ACAT will augment the conversion of cholesterol to cholesterol esters, which can be stored in the cell.
Sterol Regulatory Element (SRE)
Transcription of HMG-CoA reductase and other enzymes on the biosynthetic pathway of cholesterol are regulated by the sterol regulatory element (SRE), the promotor where the transcription factor (in this case, SREBP) binds. This is the main method by which long term regulation of HMG-CoA reductase is controlled. Under normal conditions when cholesterol is present in sufficient quantities within the cell, the sterol regulatory element binding protein (SREBP) can be found as in integral membrane protein on the endoplasmic reticulum and nuclear membrane. When cholesterol levels are diminished, the SREBP is cleaved releasing it into the cytoplasm where it subsequently enters the nucleus via the nuclear pores to attach to the SRE and hence initiate transcription of the genes responsible for the biosynthesis of cholesterol.
HMG-CoA Reductase (Istvan el al, 2000)
Regulation of HMG-CoA Reductase (HMGR)
Regulation is achieved by three main mechanisms
- Transcription and Translation of HMGR - the transcription and translation level of HMGR increases when concentrations of mevalonate pathway intermediates and products are low
- Degradation of HMGR - when these intermediates and products of the mevalonate pathway are high, HMGR degradation is increased leading to a lower concentration of enzyme within the cell
- Phosphorylation - action of the enzyme is aided by phosphorylation at serine residue 872 (S872). Phosphorylation at this site is controlled by AMP-activated protein kinases as well as HMG-CoA phosphorylase
Catalytic Activity
The catalytic portion of HMGR is a known tetramer. The enzyme itself has a membrane domain contaning a sterol sensing domain responsible for the enhanced degradation of HMGR in response to increased concentrations of oxysterols. The degradation rate of HMGR (and hence the rate at which the enzyme becomes inactive) is also dependent upon the dissociation of the tetrameric domains. Cleavage into monomers results in the increased accessibility of HMGR to protease cleavage and inactivation of the enzyme.
Sterol Regulatory Elements
HMGR's sterol sensing domain is similar to domains found at other proteins such as SCAP. Although the actual activity of SCAP is ambiguous, it is known that this protein cycles between the endoplasmic reticulum and the golgi body. SCAP influences the transport of SREBPs to post-ER compartments where the transcription factor becomes mature and activated.
Active Site of HMGR
The active site of HMGR contains two binding pockets for HMG-CoA and NADP+, the two substrates necessary to produce mevalonate from HMG-CoA. Phosphorylation occurs at S872 and the phosphorylation by AMP-activated protein kinase and HMG-CoA phosphorylase is thought to activate the enzyme.
Statin Action on HMGR
The cyclic group of statins is thought to attach to the binding pocket for NADP+ by mimicing the nicotinamide ring. Statins are thought to also inhibit the enzyme by exploiting the HMG-CoA binding pocket as well. Thus, it can be inferred that the action of statins constitutes competitive inhibition to HMGR.
Enterohepatic Circulation
Approximately 97% of the bile acids and 50% of the cholesterol is reabsorbed and returned to the liver via the portal circulation to be recycled. The secretion and resabsorption of bile acids and cholesterol provides a route for cholesterol excretion as well as homeostatic control over the cholesterol and bile acid levels via negative feedback. Reabsorbed cholesterol regulates the activity of HMG-CoA reductase while reabsorbed bile acid regulates the activity of 7-α-hydroxylase, the rate determining enzyme responsible for the conversion of cholesterol to bile acids.
Reverse Cholesterol Transport
Reverse cholesterol transport is the process by which HDL particles take up free cholesterol, esterify it, and transfer it to triglyceride rich lipoproteins for transport to the liver for disposal. This pathway may account for the protective role of HDL against cardiovascular disease.
Pathways for Cholesterol & Lipid Transport

- Exogenous Pathway - This pathway is marked by the transport of cholesterol and fatty acids from the intestine to the liver. First, intestinal cells package the triglycerides and cholesterol ester into chylomicrons for transport. The chylomicrons acquire the E apoprotein in the blood from HDL while lipoprotein lipase (LPL) hydrolyzes the core triglycerides converting the chylomicron to an HDL particle. CETP exchanges the triglycerides with cholesterol ester and the resulting remnant becomes an IDL particle. The IDL particle is recognized and taken up by Apo E receptors on liver cells.
- Endogenous Pathway - This pathway is marked by release of VLDL from the liver made up of excess triglycerides and are packaged with cholesterol, cholesterol ester, phospholipid, and B-100, C and E apoproteins. The VLDL interacts with LPL and exchanges lipid with HDL to form a cholesterol ester-rich IDL. These remnants can be taken up by LDL receptors or udnergo further delipidation by hepatic lipase (HL) and loss of Apo E to form LDL particles. These LDL particles are then removed from the circulation by LDL receptors in either the liver or extra-hepatic tissues.
Lipid Regulation
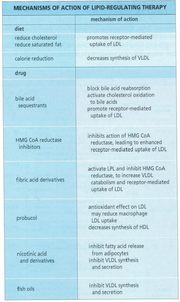
Two main methods of regulating lipids have proven effective. The first method involves diet regulation by reducing choelsterol, saturated fat, and calorie intake. The second method involves the use of drugs which act on different pathways as shown in Figure 2.
Abnormalities in Control
High blood cholesterol (Hypercholesterolemia)
High blood cholesterol arises from two known metabolic irregularities.
- Genetic reasons - Familial Hypercholesterolemia (FH)
- Consumption of a high cholesterol diet
Familial Hypercholesterolemia is an autosomal dominant (Feher 1997) trait. Homozygotes for this disorder lack functional LDL receptors, so the cells cannot take up any LDL or IDL. This results in plasma cholesterol levels up to five times higher than average. Heterozygotes have half of the normal number of functional LDL receptors and thus only haev plasma cholesterol levels about twice the average.
Ingestion of a high cholesterol diet has a similar, but less extreme, effect as FH. Since cholesterol levels in the cell are already saturated, no more LDL receptors are made and presented on the cell surface, resulting in the high level of LDL in the blood plasma.
Methods for reversing the conditions of high blood cholesterol besides maintaining a low cholesterol diet are:
- Ingestion of resins that bind the bile acid and prevent recycling of the cholesterol
- Treatment with competitive inhibitors of HMG-CoA reductase to decrease the rate of cholesterol biosynthesis.