Tony Atala: Artificial Bladder by Krishnendu Saha
Anthony Atala, M.D. is the Director of the Wake Forest Institute for Regenerative Medicine and Professor and Chair of the Department of Urology at Wake Forest School of Medicine and one of the leading scientists in the fields of tissue engineering and regenerative medicine.

Short Biography
Dr. Atala graduated from University of Miami with Psychology major and completed a medical degree in urology from University of Louisville. He pursued a fellowship at Children's Hospital Boston, Massachusetts (affiliated with Harvard Medical School) and started his independent career at the same institute developing artificial organs for humans. In 1999, his team reported the successful creation and transplantation of artificial urinary bladder in beagle dogs that showed excellent functional capabilities in terms of retaining urine and normal elastic properties [1]. After serving as the Director of the Laboratory for Tissue Engineering and Cellular Therapeutics at Children's Hospital Boston, Dr. Atala later moved to Wake Forest Baptist Medical Center in North Carolina and continued his seminal work of lab-grown organs. In 2006, his team reported succesful transplantation of engineered bladder in humans without any major complications. The patients were monitored for 5 years after surgery to determine long-term efects [2]. As of 2013, he is the W. H. Boyce Professor and Director of the Wake Forest Institute of Regenerative Medicine.
Major Accomplishments
- Developed and successfully transplanted lab-grown artificial urinary bladder using patients urothelial cells.
- Harvested amniotic fluid stem cells (AFS cells) from pregnant women, avoiding the ethical issues regarding the embryonic stem cells (ESCs).These cells are easier to culture and unlike ESCs they do not form teratoma. AFS cells are also pluripotent, thereby can differentiate into various tissue types and have tremendous potential for future regenerative medicine.
Awards and Honors
Dr. Atala have received numerous prestigious awards including-
- Christopher Columbus Foundation Award
- The World Technology Award in Health and Medicine
- Samuel D. Gross Prize
- Barringer Medal
- Gold Cytoscope award
In 2007, his work on artificial bladder was listed as Time Magazine's top 10 medical breakthroughs and No. 1 Top Science story by Discover Magazine. In 2009, U.S. News and World Reports featured Dr. Atala as one of the 14 pioneers of medical progress in the 21st century. Dr. Atala serves as editor and associate editor in many peer-reviewed journals including Stem Cells-Translational Medicine, Current Stem Cell Research, and Tissue Engineering and Regenerative Medicine. He is also editors of numerous books in the area of regenerative medicine and urology. He published more than 300 journal articles and applied for or received over 200 national and international patents. He were also invited to give TED lecture on artificially-grown organs.
Artificial Bladder
Motivation
- The need for artificial bladders is brought about by a scarcity of donor organs to treat a large number of various bladder diseases such as:
- Bladder Cancer
- Urinary Incontinence (UI)
- Estimated new cases and deaths from bladder cancer in the United States in 2013 [4]:
- New cases: 72,570
- Deaths: 15,210
According to National Institute for Continence UI affects 200 million people worldwide including 25 million adult Americans who suffer from transient and chronic UI [5]. Therefore artificial bladder will have a potential market and can improve human life and function.
Brief Timeline
- 1996: Bladder shaped mold was created and was seeded with urothelial cells on the inside and muscle cells on the outside.
- 1998: Lab-grown bladder successfully transplanted into dogs. After one year, article published in Nature Biotechnology reporting that the bladder was fully functional for 11 months.
- 1999: Artificial bladders grown from patient's own cells were implanted into 7 volunteers between the ages of 4 and 19. All the patients were suffering from spina bifida, a birth defect that that leads to hardening of bladder tissue, building high pressure and damaging the kidney.
- 2003: The patent for the process was licensed to Tengion Inc. A company dedicated to providing solutions through regenerative medicine. Dr. Atala is said to be the scientific founder of Tengion.
- 2006: British medical journal the Lancet reported for the first time artificial organs have been successfully implanted in humans. This was 7 years after the original implantation back in 1999 and the report stated the volunteers were healthy and leading normal lives.
- 2009: FDA temporarily held up Tengion's lead product candidate 'Neo-Bladder Augment' due to complications in three patients even thoughit had advanced through Phase 2 clinical trials. [11]
- 2010: Tengion submitted phase I clinical trials of 'Neo-Urinary Conduit' that, the company said, would be simpler and faster to produce, and would address a larger market. [9]
- Jan 2013: Tengion announced that it successfully implanted Neo-Urinary Conduit in the seventh patient in the ongoing phase I clinical trial. [9]
- March 2013: Final data collection date for primary outcome measure. Phase 2/3 trials will begin in sometime in 2013. [8]
Making the Bladder
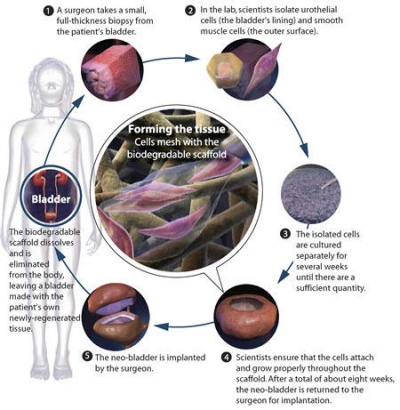
A very small piece of the bladder is cut off from the patient usually smaller than the size of a postage stamp. It is very important that the biopsied bladder piece be free from disease. A biodegradable scaffold is molded in the shape of a bladder, this is after a CT scan has been performed on the patient to check the precise dimensions. The cells obtained from the bladder piece are grown outside the body for 7 to 10 days. These cells are urothelial cells. After that are seeded or 'painted' onto the scaffold. This is now put into and oven like device at body temperature and 95% oxygen for about 6 weeks. After this time the organ is ready to be implanted into the patient.
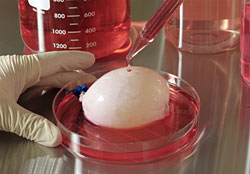
Advantages and Limitations
- Current gold standard for bladder replacements involve the use of tissue grafts from bowel. However, the intestine is designed to absorb nutrients and the bladder is designed to excrete, patients who have this procedure are plagued with many problems including reabsorption of toxins, formation of stones and kidney damage. Moreover, intestinal cells causes the body to absorb calcium, leading to osteoporesis.
- It eliminates the risk of organ rejection because the patient is using cells obtained from their own body.
However, the scientists arose concern that the technology can be challenging to the elderly people who have limited regenerative capacity to obtain sufficient amount cells for the transplantation. One more question remains that for the bladder cancer patients who have malignant urothelial cells. Harvesting and culturing the malignant cells can increase the possibility of malignant cell transplantation back to the body [6]. Steve Chung of Advanced urology Institute of Illionis commented that "Atala and his colleagues should be praised for the milestone they have reached, but further multi-institutional studies are needed with longer follow-up. Until then surgery using intestinal tissue to repair the bladder remians the gold standard." [7] As of 2013, the bladder is not yet approved by FDA.
Funding
- Dr Atala received a $1 million grant from the Department of Defense in 2006 to develop technologies to restore injured limbs of soldiers.
- Tengion announced $40 million dollars initial public offering in 2010. [10]
References
- [1] http://www.nature.com/nbt/journal/v17/n2/full/nbt0299_149.html
- [2] http://dx.doi.org/10.1016/S0140-6736(06)68438-9
- [3] http://biomed.brown.edu/Courses/BI108/BI108_2007_Groups/group10/tissue_engineering.html
- [4] http://www.cancer.gov/cancertopics/types/bladder
- [5] http://www.nafc.org/media/statistics/prevalence-2/
- [6] http://usrexp-sandbox.nature.com/nbt/journal/v17/n2/pdf/nbt0299_133.pdf
- [7] http://www.newscientist.com/article/dn8939-bioengineered-bladders-successful-in-patients.html
- [8] http://www.tengion.com/about/index.cfm
- [9] http://phx.corporate-ir.net/phoenix.zhtml?c=218965&p=irol-newsArticle&ID=1797085&highlight=
- [10] http://articles.latimes.com/2006/apr/04/science/sci-bladder4
- [11] http://www.bizjournals.com/triad/stories/2010/02/15/story9.html?page=all
- [12] http://discovermagazine.com/2007/jan/medicine#.UWXXmrVg_w8
