The Wyss Institute for Biologically Inspired Engineering
Overview
The Wyss Institute for Biologically Inspired Engineering
The Wyss Institute was established in 2009 following a $125 million donation to Harvard University by Hansjorg Wyss.[1] The institute was formed with the idea that a multidisciplinary institution could ferment enhanced innovation across multiple industries by maximizing collaboration, building on the Harvard Institute for Biologically Inspired Engineering, created a year prior. It is an alliance between multiple Universities and Hospitals in the Boston area including The Harvard Schools of Medicine, Engineering, and Art Science, The University of Massachusetts Medical Center, Tufts University, Boston University, Boston Children’s Hospital, Brigham and Women’s Hospital, Beth Israel Deaconess Medical Center, Massachusetts General Hospital, the Dana Farber Cancer Institute, and Spaulding Rehabilitation Center. The institute conducts research that spans multiple fields, especially the eight major focus areas: 3D Organ Engineering, Adaptive Material Technologies, Bioinspired Robotics, Biomimetic Microsystems, Immuno-Materials, Living Cellular Devices, Molecular Robotics, and Synthetic Biology, all of which utilize natural organisms and processes as inspiration for emulation in the form of novel technologies. Research groups are led by one of 18 Core Faculty or one of 15 Associate Faculty members, who are supported by undergraduate students, graduate students, post-doctoral fellows, and advanced technology team members. The institute represents one of the first platforms for the simultaneous contribution of physicists, chemists, biologists, engineers, and clinicians towards engineering innovations that address common issues. A business development team and collaborations with other start-ups and corporations allow for the translation of technology into commercialized products.[2]
Notable People
Hansjorg Wyss
Hansjorg Wyss is a Swiss engineer, entrepreneur, and philanthropist who earned a Master’s degree from the Swiss Federal Institute of Technology Zurich and an MBA from Harvard University. Approximately ten years after receiving his MBA in 1965, Wyss was introduced to the biomedical device industry and in 1977 founded the American installation of the Swiss manufacturer, Synthes USA.[3] Under the leadership and direction of Wyss, Synthes USA grew to become the leading producer of devices focusing on the treatment of broken bones and minor traumas. In 2012, Synthes USA was sold to Johnson & Johnson for $20.2 Billion. Wyss is worth approximately $5.5 Billion and has contributed to many charitable endeavors, most notably the $125 million donation given to Harvard University to form the Wyss Institute for Biologically Inspired Engineering in January, 2009.[4] Wyss donated a further $125 million in 2013 to the Institute, which represented the largest individual donation in the history of the University. Other endeavors in which Wyss has been instrumental include the formation of the AO Foundation and the Wyss Foundation, which oversee the large scale management of musculoskeletal surgery and environmental preservation, respectively. [3]
Donald Ingber
Donald Ingber is the Founding Director of the Wyss Institute, named to the position at the time of Hansjorg Wyss’s donation to Harvard in 2009. Ingber received his MD/PhD from Yale University Medical School in 1984 and has worked at Boston Children’s Hospital as a researcher and professor in the Vascular Biology department and as a professor of Bioengineering at Harvard University. Ingber’s work has focused on the importance of mechanical cell properties on structure, function, and cancer formation.[5]
Timeline
- 1977: Hansjorg Wyss founds Synthes USA
- 2005: Provost of Harvard University forms committee to consider a biologically inspired engineering department
- 2008: Creation of the Harvard Institute for Biologically Inspired Engineering, given seed funding by Harvard University
- 2009: Hansjorg Wyss donates $125 million to found the Wyss Institute for Biologically Inspired Engineering
- 2013: Hansjorg Wyss donates an additional $125 million. The Wyss Institute now employs 350 individuals
Tissue Engineering at the Wyss Institute
3D BioPrinting of Vascularized, Heterogeneous Cell-Laden Tissue Constructs
The Kolesky Group at the Wyss Institute has formulated a method to develope three dimensional tissue constructs that are able to incorporate vasculature into cell seeded synthetic extracelluar matrices (ECM). The goal is to create a perfusable construct that avoids regions of necrosis that unvascularized models are vulnerable to.[6]
Vasculature
Pluronic F127 is a copolymer that is composed of two hydrophilic poly(ethylene oxide) components surrounding a hydrophobic poly(propylene oxide) component. Pluronic F127 is unique in that it has the ability to transition from a gelated state above a critical concentration and temperature in aqueous solution (21% by weight, 4 degrees Celcius) to a liquified state in which the poly(propylene oxide) becomes hydrated and the coplymer dissolves in water. The gelated state occurs due to the formation of pluronic F127 micelles . It is printed as a gel and later removed as a liquid when the tissue construct is cooled below the critcal temperature, leaving empty channels. Pluronic F127 is biologically inert and therefore biocompatible with seeded endothelial cells.[6]
ECM
The ECM was formed from denatured collagen with functionalized methacrylate groups which determine the elasticity of the material, known as gelatin methacrylate. Gelatin methacrylate in cell culture media is a liquid above 23 degrees Celcius, but below this temperature forms a gelated ink that becomes more and more elastic with decreasing temperatures. Collagen contains integrin binding motifs that make gelatin methacrylate a viable material to allow for cell migration through the synthetic ECM.[7]
Cell Seeding
The ECM solution was seeded with human neonatal dermal fibroblasts expressing green fluorescent protein. Fibroblasts were incorporated into a gelatin methacrylate cell culture meduim with DMEM and fetal bovine serum (FBS). Human umbilical vein endothelial cells (HUVECs) were incorporated into the hollowed out channels after the copolymer was vaccuumed out via syringe, and incubated on a rocker to promote adhesion to the gelatin channel walls.[6]
Process
The 3D printing process follows the following steps. Each ink is supplied by a 30 micrometer nozzle.
- Poly(dimehtyl siloxane) (PDMS) printed along the boundary of the tissue construct
- Unseeded gelatin methacrylate (ECM) is applied to the base of the construct
- Alternating layers of cell-laden gelatin methacrylate and pluronic F127 are dispensed on the ECM (at 22 degrees celcius, so that both are gelated)
- The temperature is reduced to below 4 degrees celcius, and the liquified pluronic F127 is sucked out using a syringe, leaving channels (100-1000 micrometers in diameter)
- a HUVEC medium is introduced and incubated, allowing the cells adhere to the channel walls [6]
Results
Cell staining showed that the HUVECs formed a coherent layer dispersed along the gelatin channel walls and viability increased from 61% to 82% from day 0 to day 7. The viability of the fibroblasts increased from 70% to 81% from day 0 to day 7, which suggests that both cell types were able to successfully proliferate in the tissue construct.[6]
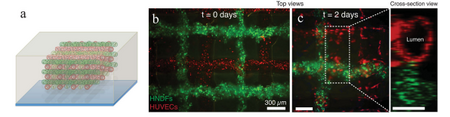
Recent advancements in 3D printing
Instrumented Cardiac Microphysiological Devices via Multimaterial Three-Dimensional Printing
The Lind Group has utilized 3D printing to synthesize micro scale devices that mimick human tissue and provide constant readings of contractile stresses in engineered cardiac tissue. These devices are comprised of six inks derived from soft biocompatible materials that encapsulate a cantelever. The cantelever is displaced with the contractile stresses provided by the engineered cardiac tissue and sends electical messages with the associated pressure changes. This work aims to reduce the need for animal models for the study of tissue function.[8]
Three Dimensional Printing of Thick Vascularized Tissues
The Kolesky Group went on to test the vascularized 3D printed method in an updated chip construct. Human Mesenchymal stem cells (hMSCs) were added to monitor the support of differentiation by the synthetic ECM environment. Permeability testing was done to confirm the confluence of HUVECs on the channel walls. After 6 weeks, the HUVECs maintained their identity and formed lumen, which suggests a decrease in permeability compared with non-adherent gelatin walls. The chip constructs were then perfused with osteogenic differentiation factors: BMP-2, ascorbic acid, and glycerophosphate. Differentiation was confirmed by the staining of osteocalcin in the hMSCs.[9]
References
[1] Hansjorg Wyss Gives $125M to Create Institute (2008). Harvard Gazette.
[2] FAQ (2017). The Wyss Institute.
[3] Hansjorg Wyss, MBA 1965 (2007). Harvard Business School Alumni Stories.
[4] Hansjorg Wyss (2017). Forbes Profile.
[5] Donald E. Ingber, M.D., Ph.D. (2017). Wyss Institute.
[6] Kolesky, D.; Truby, R.; Gladman, A.; Busbee, T.; Homan, K.; Lewis, J.; 3D Bioprinting of Vascularized, Heterogeneous Cell-Laden Tissue Constructs (2014). Advanced Materials. 25, 3124-3130.
[7] Leavesley, D.; Schwartz, M.; Rosenfeld, M.; Cheresh, D.; Integrin B1- and B3-mediatied Endothelial Cell Migration Is Triggered Through Distinct Signaling Mechanisms (1993). The Journal of Cell Biology. 121. 163-170.
[8] Lind, J.; Busbee, T.; Valentine, A.; Pasqualini, F.; Yuan, H.; Yadid, M.; Park, S.; Kotikian, A.; Nesmith, A.; Campbell, P.; Vlassak, J.; Lewis, J.; Parker, K.; Instrumented Cardiac Microphysiological devices via multimaterial three dimensional printing (2016). Nature Materials. 16. 303-308.
[9] Kolesky, D.; Homan, K.; Skylar-Scott, M.; Lewis, J.; Three-Dimensional Bioprinting of Thick Vascularized Tissues (2016). PNAS. 113. 3179-3184.
[10] Chiang, M.; Fan, S.; Generation and Assembly of Cell-Laden Hydrogels on a Digital MicroFluidic Platform (2012). International Conference on Miniaturized Systems for Chemistry and Life Sciences. 16. 575-577.