Remote Patient Monitoring
Remote Patient Monitoring
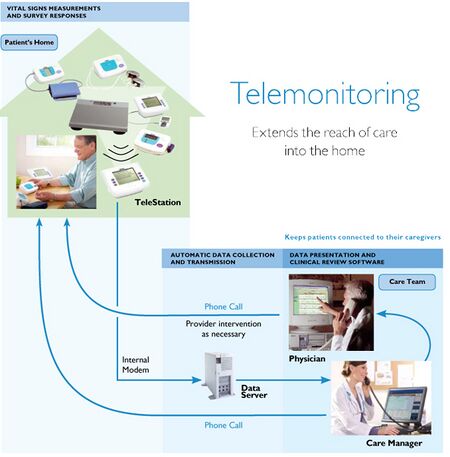
Remote patient monitoring (RPM) is a broad term used to describe monitoring patients health outside of a clinical setting. Through this technique, health officials can monitor chronic diseases of a patient at their residence. This type of monitoring ideally relieves the health care system of many unnecessary hospitalizations and time spent in hospital stays. Meanwhile it provides the patient with the care and attention on as needed basis. This gives comfort not only to the patient but to the family of the patient. This health care system requires a degree of compliance from the patient and understanding of certain diagnostics. Although integrative systems can be set up that will eliminate most if not all of the steps patients must take in independent health care. The type of monitoring system(s) are also dependent on the condition of the patient and chronic illnesses they possess. Current RPM are limited in health care settings because of monetary obstacles, the scope of the technological shift, as well as ineffectiveness shown for RPM in trial settings. A large scale randomized control trial was conducted in the United Kingdom that showed significant decreases in hospital stays, but progress decreased quickly when the program ended.
Remote patient monitoring has shown promising results for cost reduction in numerous studies. Currently the U.S. spends over $1 trillion in health care, where Medicare and Medicaid make up the majority of these costs [4]. As people continue to live longer, chronic conditions become more prominent for health costs. The idea is that remote patient monitoring has the ability to reduce the incidences and hospitalizations for chronic illness patients by giving them the support they need at home. There are considerable obstacles associated with the current infrastructure in the health care system, but it will become more apparent as the rate of chronic illnesses such as Alzheimer's and chronic heart failure increase.
Recently, venture capitalists in the United States have shown an interest in RPM devices. As a result of the Affordable Care Act, there has been a greater shift towards applications that reduce hospital time and remote patient monitoring has shown potential for the market. It is important to note that the technology for the integration of these devices has been there, it is the application of them on a larger scale that has been stagnate.
Terminology
- Telehealth: Telehealth is a broad term used to describe provision of current health care services through integration and use of technologies. This term encompasses both Telecare and Telemedicine and allows for cross-coordination between the patient and health consultants[6].
- Telecare: Telecare is the technology used for patients to allow them to self monitor themselves and give them appropriate feedback. This includes devices that monitor the patients health like glucose monitors and blood pressure recorders. Most monitoring devices are continuous and will provide up to date monitoring for the most effective diagnosis.
- Telemedicine: Telemedicine refers to the use of telecommunications to improve current health services and practices. This is the use of electronic media to transfer information back and forth between a patient at home and health care professionals.
- Peripheral: Devices that are external of the body and have the capability of being connected to screen or other electronic monitoring device.
Technologies and Devices
There are many different technologies and devices currently used for remote patient monitoring. These devices help the patient monitor their health and can make adjustments and give feedback to the patients via an injection or alarm, respectively. The most common measurements follow a protocol to measure and transmit data. A sensor is connected to a wireless media to measure some physical measurement. This data is stored on a patients' device for self monitoring and also sent to a centralized data repository for analysis by health care professionals. A diagnostic application software has a controller that will perform appropriate tasks or alert the patient or health professional of any severe condition. The amount of sensors and degree of storage and data transfer is dependent on the severity and recurrence of the patients conditions.
Devices
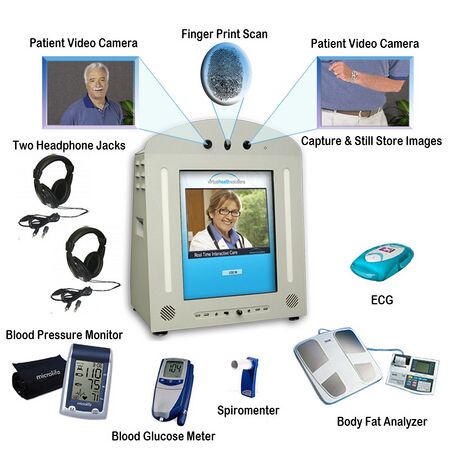
Telehealth
These devices are designed to monitor parameters a doctor would measure for a typical visit. For the purposed of telehealth these devices take measurements intermittently as given by doctor's discretion. This is especially useful in monitoring patients after surgeries to help avoid more frequent visits. It also helps in patients with chronic yet not recently serious long term conditions.
- Monitors: These monitors store visual data and works with peripherals to show patient and health care professional any severity.
- Blood Pressure Monitor: A cuff on the arm used to check blood pressure.
- Pulse Oximeter: Clips to the tip of individual's finger and measures blood oxygen levels and/or heart rate.
- Blood Glucometer: Used to measure blood sugar levels.
Telecare
These devices are for people with social care needs. These devices can communicate be in direct connection with Call Centres and even health care professionals. These products are ideal for patients that are currently under house care.
- Telecare Home Unit: Is a recordable device that also is linked to sensors and is in direct contact with the Call Centre.
- Personal Alarm: A panic button that can alarm Telecare home unit
- Epilepsy sensor: It includes a bed sensor, monitors heart rate and breathing patterns.
- Enuresis Sensor: Helps people who have involuntary urination by detecting when the bed is wet and giving an alarm.
- Fall Detector: A portable detector that can sense when an individual falls.
The devices listed for Telecare are highly personalized and dependent on the patients condition. There are additional house monitors that can measure and detect extreme temperatures, carbon monoxide, water levels, and gas detection. These devices are all either connected to a Call Center or have automatic shut off controls in place when a certain threshold is reached.
Whole System Demonstration in the UK
Program Setup
Since there had been no large scale integrated implementation of RPM, the UK set up a Whole System Demonstration (WSD) to examine the effectiveness. The WSD was a two year project started in 2008 funded by the Department of Health to see how technology can assist in home health care. This was supposedly the largest randomized control trial (RCT) using Telecare and Telehealth to date, with 6191 patients and 238 General Practitioners across three sites[7]. The program had two main goals: to integrate national health care and local social care in an organized and transparent manner. Also, the project aimed to test a large scale Telehealth and Telecare initiative without compromising the health of the patient. This is a sensitive scenario because it requires compliance and action from the patient in some situations. According to the Department of Health, there was a 45% reduction in mortality rates, 20% reduction in emergency admissions, and a 14% reduction in bed days[2]. The results are promising, but there is a degree of reluctance to push forward(Hardy). Each site had its own WSD evaluation team that could monitor the progress. The individuals chosen for the testing were of the same demographic for each site to evaluate the consistency. Expert health care providers helped recommend the best equipment and most cost effective strategy for differing patients conditions. There was a large degree of cross coordination between public and private sectors in initiation and implementation of the systems. The case studies used additional methods to avoid biased interpretation of results. Ultimately they found that not enough patients were recruited for the mixed group who needed attention in both Telecare and Telehealth. This halted the integration between social care and health care and left them largely independent for the entire trial.
Critiques of System
The WSD is a program that has been given a lot of praise by policymakers. Although case studies performed by University of Surrey, Imperial College Business School, among other schools have recognized the difficulty of this system and the ambiguity of whether the program accomplished its goals. The case studies focused on clinical outcomes, economic impacts, experiences, and service delivery for scaling up. This entailed numerous interviews and data analysis performed by the team of researchers to discover the relationship between stakeholders within the program. Ultimately they found a lack of integration in health care and social care. There was a large emphasis on remote patient monitoring and less so on social care practices. The case study found a high degree of WSD staff turnover because the health consultants were only temporary. That means all the progress made in the system was lost because the health professionals that learned the nuances of RPM were lost to layoffs. Ultimately the benefits of the program are largely lost because of the emphasis on meeting protocols of the RCT and less attention paid to implementation of the system. As stated in the case study, "[The researchers] found that in actuality the sites were not ready to implement this level of organizational change within the timeframe given".
Further Studies
The same researchers are performing a further case study on six different UK sites to examine the integrated heatlh care systems and look at the supply chain of technology. Early analysis of the sites leads them to a similar conclusion: the scale up process must be incremental and health care workers should be well adjusted to the processes.
Other Randomized Control Trials
Since RTC's help determine the efficiency and effectiveness in remote patient monitoring it is important that statistical significance can be interpreted from all of the data.
A team of researchers from Australia did a massive peer review of 14 randomized control trials with over 4,000 patients. Their study focused on individuals who have chronic heart failure, had been administered to the hospital recently, and followed a series of other parameters. These parameters were important in their formation of a concrete meta-analysis of the several studies. The team found a slight degree of heterogeneity within the results, but they found positive results. According to their statistical analysis using a random effects model they found a 20% reduction in hospital admissions for CHF as well as a 20% reduction in all cause mortality rates. The team also found no significant difference in the all cause hospital admissions, but this could be due to the lower mortality rates increasing the likelihood of a return to the hospital. Also the study and equipment was largely focused on treatment of CHF so these two factors most likely contribute to the all cause hospital admissions. The team proposed introducing more equipment to compensate for this. These studies did not focus on the costs associated with each system, but did find positive results for increased health quality of life according to the review.
A study performed by the University of California Irvine focused on the costs associated with the program. They had a telemonitoring, telephone, and usual care services set up as individual groups to examine the difference in costs over a 12 month period after admission to the hospital. The study found that readmission costs for patients with heart failure were reduced 86% relative to usual care. This could be a result of insufficient data provided by the low sample size used; there were only 12 patients in each group. It also could be a result of the high costs the University has for hospitalizations relative to normal US non-government hospitals. Equally impressive is how effective the telephone was relative to telemonitoring. Overall, this shows how checking in with patients with chronic illnesses after hospitalization can dramatically reduce costs for readmission.
Emerging Devices

- Smart Mat: BAM labs has an FDA approved sensor mat that is placed under a patients mattress to monitor their presence, heart and breathing rates.
- Independa: This company has created an integrated system for houses for monitoring clinical parameters like blood pressure and glucose , and also sensors that monitor motion, toilet flushing and door opening[5].
- InTouch: Has an FDA approved system to conduct real-time clinical practices with their RP-7i robot. The robot is controlled with a joystick by a physician via a wireless connection and the doctor can make appropriate prescriptions and recommendations for patients in isolated care centers. The team has had the robot sit in on an Argentinian hospital to counsel a surgery[1].
- Vivify: It is a cloud based application that tracks arrival of severe conditions. It includes videoconferencing and customized health care plans[5].
- Sotera: Is an in-hospital device that can give urgent updates to physicians during the day. It can monitors heart rate, ECG’s, blood oxygen levels, skin temperature, etc. in bed and in transport. The device is strapped to patients wrist, with sensors on the chest and arm.
References
- [1]Corley, Anne-Marie."The Reality of Robot Surrogates:How far are we from sending robots into the world in our stead?". IEEE Spectrum 23 Sep. 2009. Web. 10 March 2015.
- [2]Hendy, J., Chrysanthaki, T., Barlow, J., Knapp, M., Rogers, A., Sanders, C., et al. "An organisational analysis of the implementation of telecare and telehealth: The whole systems demonstrator". BMC Health Services Research, 12, 403-407.
- [3]Jerant, A., Azare, R., Nesbitt, T. "Reducing the cost of frequent hosptial admissions for congestive heart failure - A randomized trial of a home telecare intervention". Medical Care. 39,11 (2001): 1234-1235.
- [4]National Center for Health and Statistics. "Health, United States, 2013: With Special Feature on Prescription Drugs". Hyattsville, MD. 2014.
- [5]Rudansky, Alex. "Remote Patient Monitoring: 9 Promising Technologies". Information Week 30 July 2013. Web. 10 March 2015.
- [6]"Telehealth, Telecare, and Telemedicine...What's the Difference". GlobalMed. Web. 10 March 2015.
- [7]"Whole Systems Demonstrators: An Overview of Telecare and Telehealth". Department of Health. Web. 10 March 2015.
