Recreating the Tumor Microenvironment
Introduction-Modeling Tumor Death: Microfluidics and Biomimetic Tumor Spheroids
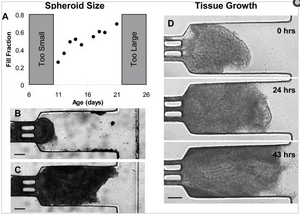
Cancer accounts for the highest cause of death in economically developed countries [1]. As a result, a substantial amount of effort has been focused on developing novel therapies to treat the disease. Unfortunately, drug efficacy is only tested with high throughput monolayer cell death assays, which do not account for transport barriers encountered in vivo [2–4]. Microfluidic devices can model in vivo tumor biology (figure 1) while maintaining the high throughput capacity of monolayer cell death assays.
Overview of Cancer Pathology
Cancer follows the following distinct path: Benign growth, Infiltrative growth, vascularization, and finally metastasis. Initially, premalignant masses grow in a benign manner and are confined to a distinct area of the respective organ. After this phase of growth, many tumors cells remodel the extracellular matrix and become increasingly invasive. These tumor cells commonly enter lymphatic vessels and colonize near and distant lymph nodes. In the later stages of the disease, primary tumor cells break off from the main mass, enter blood vessels and colonize distant organs. This metastasis of cancer cells leads to organ failure and eventual death [5,6].
Current High Throughput Drug Testing Methods
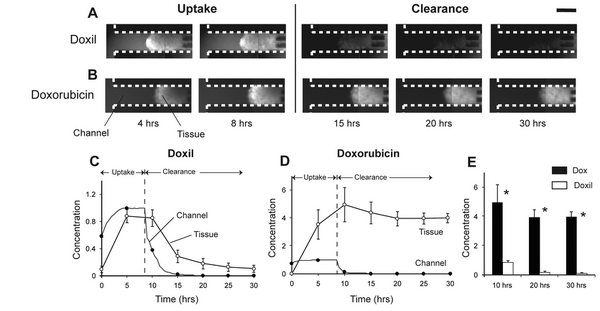
Cancer cells have been taken from patients, immortalized or conditionally reprogrammed and cultured in monolayer reliably [7]. This is the main reason why monolayer cell culture assays are commonly used to test cancer therapies in high throughput. Out of all the drugs that are screened, less than 5% of drugs make it through pre-clinical trials and of those, only 10% make it through clinical trials [8,9]. Monolayer assays do not account for important transport limitations imposed on in vivo tumors [3,4]. This poses a problem because larger molecules have difficulty penetrating and treating tumor cores, which are the most drug resistant regions. Unlike microfluidic devices, monolayer assays cannot properly assess drug efficacy within the drug resistant quiescent and necrotic regions of tumors which contributes to cancer relapse [4]. The heterogeneous nature of tumors and significant transport barriers demonstrates a need for improving high throughput drug testing that mimics in vivo conditions (figure 2) [10].
Role of Microfluidics in Cancer Research Abroad
With the numerous advantages of microfluidics becoming fully realized, researcher labs have embraced microfluidics for a diverse range of applications specific to cancer research. The applications of microfluidics for cancer research can be categorized into four general groups: cell sorting (isolation of cancer cells), controlled generation (from seed to harvest), drug screening, and modeling. In some capacity, there is overlap between the groups as is shown is later examples. With advent of tumor spheroids as a means for improved in vitro modeling, microfluidic applications have shifted towards production and screening of these spheroids.
Cell Sorting
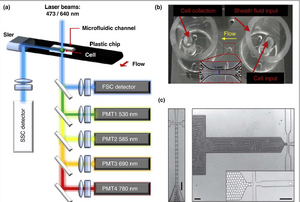
Cell sorting through microfluidics allows for single cell analysis using traditional methods, most notably flow cytometry. Being able to separate different cells is critical for accurate drug screening, medical diagnostics, and cancer cell assays[11]. Because micro-sorters possess the capability to sort by a wide range of characteristics (size, charge, shape, binding affinity, etc), they can be installed into virtual any microfluidic device that requires sorting of particles, in this case cancer cells [11]. Once cells are sorted out, fluorescently activated cell sorting (FACS) has proven to be a powerful tool for analyzing cancer cells. Depending on the fluorescent labels being used, FACS can show cell death (stages of apoptosis or necrosis), drug diffusion and permeation, and protein location [11]. This is illustrated in Figure 3. Other modes of cell sorting exist such as Raman activated cell sorting (RACS) and fluorescence activated droplet sorting (FADS), which carry their own benefits in terms of chemistry and throughput efficiency [11].
Cell sorting has also used to isolate circulating tumors cells in large blood samples [12]. The ability to isolate, harvest, and analyze circulating tumors cells creates opportunity to better understand metastasis and other cancer mechanisms. In 2007, a collaborative research team successfully isolating circulating tumors cells by precisely washing blood through a filter of posts that were treated with antibodies specific to the target cancer cells [12]. By precisely flow blood through the micro post filter under laminar flow conditions, the device was able to isolate tumors cells from the sample medium [12].
Tumor Spheroid Production

Precise 4D(Space-time) laminar flow control, biocompability, and relatively low cost-effectiveness have made microfluidics an ideal application in the culturing, forming, and harvesting of 3D tumor spheroids [11]. In recent years, the methods for tumor formation in a microfluidic device has increased with the advent of tumor spheroids as a viable means for modeling [11]. The two primary modes of tumor production depend on sufficient mixing of a cell suspension to generate natural clustering or forced spheroid growth through geometric confinements (concave interfacial boundaries) as found in poly-hydroxyethyl methacrylate or hanging droplets [11]. (Tumor on Chips)
Very recently, a collaborative research based in Taiwan was able to seed, culture, form, and remove tumor spheroids from a two-layer device through simple laminar flow of seeded medium (in the top layer) over microwells(in the bottom layer) [13]. To temper the parabolic nature of flow through the channel, seeded medium was manually pumped at flow rates over 100 microliters per minute [13]. The wells were filled with seeded due to gravity [13]. Geometry of the wells was proven to generate consistency is tumor spheroid size and shape [13].
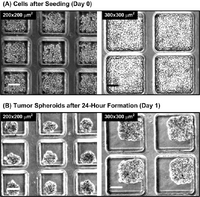
Research has been done to successfully form tumor spheroids by hanging drop method, a process of allowing gravity and liquid-air tension to form droplets containing cancer cells[11]. These cells grow and aggregate within the liquid droplets to spherical shapes. The uniformity of the spheroids proves inadequate for reliable testing, as spheroid size has shown great effect on drug efficacy[14]. The precise spatiotemporal control on fluid at the microscale has been used to produce droplets of reliably uniform size and shape on the nanometer and micron scale [11,13,14]. This capability was employed using an intersection of cross-flow streams [14]. As the bisecting aqueous stream enters the intersection, the faster continuous stream applies a shearing force on the stream head, essentially cutting off a plug of fluid [14]. These plugs are spherically in shape and consistent in diameter because of the flow control within the device [14].
As mentioned, the common materials used for microfluidic devices are often compatible with living cells. Polyethylene glycol (PEG) and polydimethylsiloxane (PDMS) are the primary materials being used due to their aversion for protein and cell adhesion [11]. Through the use of photolithography, a well-established method of generating silicon masks for PDMS molding allows for low cost, rapid manufacturing of devices for testing. Within this vein, certain considerations must be made in terms of treating the microfluidic device to improve cell viability. In cases where tumor spheroids are being readily cultured and formed within the device, devices are often sterilized with deionized water, UV light, or ethanol to avoid contamination [11,14].
Modeling
While three-dimensional tumor spheroids have been shown to provide improved in vitro modeling, work has been done to design microfluidic channels to better replicate tissue vascularity and also to mimic important interfacial cell-to-cell or cell-to-intracellular matrix regions. In the pursuit of understanding cancer metastasis mechanisms, microfluidic devices are designed to replicate these regions, which allows for analysis of biological activity occurring at the microscale that couldn’t be observed in vitro otherwise.
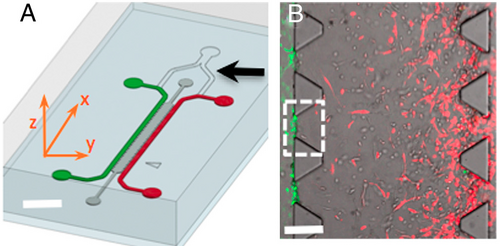
Zervantonakis et al, and researchers from departments within the Massachusetts Institute of Technology replicated the tumor tissue – endothelium interface to analyze and model how tumors cells successfully enter the blood stream1 [5]. The device consists of a three-channel composition with the channels running parallel and connected at the sides1 [5]. In the other channels, endothelial cells and cancer cells are seeded respectively with a hydrogel extracellular matrix in between [15]. As such, experiments can be done to observe how tumor cells respond in real time to changes in microenvironment – adjustments to gradients of nutrients and oxygen or stimulation from spikes in growth factors15. Additionally, reasoning for the dependence of a damaged blood or lymphatic vessel to promote cell entry into the blood stream can be made due to the design of the endothelial channel [15].
Drug Screening
In many cases, the three previously described applications are paired with drug screening to test drug efficacy, cell death, cell diameter reduction, cell membrane integrity, diffusion properties of drugs, among many other important results of drug testing [11,14–17]. In projects previously mentioned, a common theme of experimentation was to analyze tumor spheroids and monolayer cell cultures after introducing anti-cancer drugs into the systems. The Tawain group that used gravity-packed wells for tumor spheroid production tested three drugs and observed cell diameter and membrane integrity through microscope imagery and fluorescence activated cell sorting respectively [13]. Sabhachandani et al ran two drugs through continuously flowing medium past packed microdroplet-formed spheroids [14]. As proof-of-concept, both groups were able to confirm a significant difference in cell death between two-dimensional monolayer cell cultures and three-dimensional tumor spheroids [13,14]. Microfluidic devices can be designed to recreate the tumor microenvironment in vitro. The devices can accurately mimic transport barriers [10] and the heterogeneous nature of tumors. Fluid flow in both tumor microvasculature and microfluidic devices is laminar. In addition, tumor spheroids can be positioned within the devices to form actively dividing, quiescent and necrotic tissue which resembles in vivo conditions [4]. Due to nutrient gradients present in tumor-on-a-chip devices, cells residing on the tumor interior are nutrient deprived and undergo necrosis while media exposed cells actively divide. This spatial heterogeneity within in vitro tumors improves drug efficacy and transport modelling due to the system’s in vivo resemblance (figure 2) [10].
Using fluorescent modifications, like FITC, and microscopy, chemotherapeutic treatment can be spatiotemporally modelled for a variety of drugs with a microfluidic device. This experimental data can be used in Fick’s law of diffusion to calculate the effective diffusion constant which describes a drugs transport efficacy. The simplified Fick’s law used for tumor transport modelling is as follows:
[math]\displaystyle{ \frac{\partial C_A}{\partial t}+v\bigtriangledown C_A=D_A \bigtriangledown^2 C_A+R_A }[/math] (1)
With the following boundary conditions:
[math]\displaystyle{ \frac{\partial C_A}{\partial z}|_{z=1}=0 }[/math] (2)
[math]\displaystyle{ \frac{\partial C_A}{\partial z}|_{z=0}=e^{-kt} }[/math] (3)
[math]\displaystyle{ \frac{\partial C_A}{\partial r}|_{r=0}=0 }[/math] (4)
[math]\displaystyle{ \frac{\partial C_A}{\partial r}|_{r=1}=0 }[/math] (5)
And the following initial condition:
[math]\displaystyle{ \frac{\partial C_A}{\partial t}|_{z=0}=C_A0 }[/math] (6)
The boundary conditions (2), (4) and (5) are all no flux boundary conditions due to either cylindrical symmetry or because the tumor is in contact with an impermeable wall and boundary condition (3) pertains to the half life of drug in the media that is contact with the tumor surface. The reaction term of the drug accounts for drug binding and metabolism within a tumor cell and will usually be a negative term.
Experimental data acquired from a tumor-on-a-chip model can be fit to a discretized version of (1) and an effective diffusion constant can be calculated. The calculated diffusion constant will give an indication of how easily a drug penetrates into a tumor. For large drugs, like antibodies, examining drug diffusion into tumors is useful because it provides answers about how well quiescent and necrotic tissue are treated when dosed with macromolecular therapies. These studies have not been performed to date and can provide valuable information about biologic dosing regimens.
Tumor-on-a-chip drug testing must be expandable to allow for high throughput screening. In order to make microfluidic drug testing scalable, the technology must be automated and allow for stringent flow control within a multichannel device. This can be achieved through the use of multilayered, valved microfluidics. To make this device compatible with high throughput screening, automation is required. This can be achieved through the use of programmable pneumatic actuators coupled with valve control channel networks.
Microfluidic Valve Control
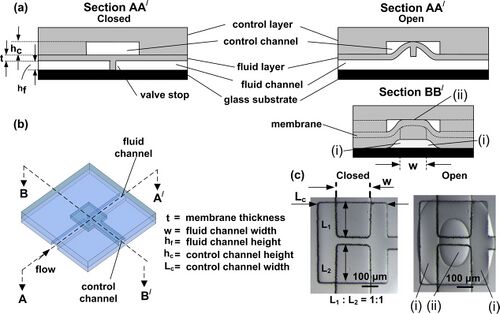
For a microfluidic system to function properly, valve structure and control plays an important role in flow control. In this specific case, tumors are being flowed through a main channel where, depending on the specific combinations of opened and closed valves, each will be directed to individual chambers for packing. Preliminary designs provide proof-of-concept for the final large-scale system; before additionally complexities can be added, the basic system must be able to govern flow control through valving so that tumors can be packing successfully and efficiently. Therefore, it is important to ensure the valve structures are designed properly at the outset. In the following section, design considerations and challenges for tumor packing will be discussed. The proposed preliminary design simultaneously improves upon a preceding system for tumor packing and provides a foundation for a scaled-out high volume system. Previously, the Forbes Lab at the UMass Amherst used a microfluidic system, which contained three main channels in parallel. Between the three main channels, four smaller perpendicular channels are placed on each side on the central main channel. To pack the tumor spheroids, the valve located at the end of the main center channel is closed through pressure actuation with the main channels, left and right, being left open. With an applied syringe vacuum, fluid containing the tumors is pulled through the left and right main channels. Ideally, the tumor spheroids “catch” on the perpendicular side channels each tumor will be held in place by posts located in the side channels. In reality though, there are a host of problems with the system. Two or more tumors can pack into side channels. Tumors can flow down to the end of the center channel and accumulate. The frequency of tumors catching the side channels is incredibly low. Our proposed preliminary design, while simple, should be much more effective at packing due to valve structure and channel design for the fluid and control layer. Rather than having three channels, the design in reduced to one main input channel and a parallel output channel with perpendicular channels connecting the two. Importantly, the control layer contains four channels which lie atop the side channels. Above the area to the right of the well posts, each valve channel ends with a square slab. Through this simple design, four actuate-to-open valves are formed for controlling fluid passing from the input to the output channels.
These channels will remain closed until a vacuum is applied to the channel, resulting in a lifting of the valve. Thus, all four channels are closed by default. Using supportive lab devices such as Elveflow and MUX Quake, programmable logic allows for automated vacuum/pressure control in the control layer, which results in precise opening of desired channels. Furthermore, as tumor spheroids flow down the input channel, the fluid will flow through the one side channel open. In sequence, the first valve will remain open until one tumor is secure in the well before closing. Then, the next valve in the line will open. The end result should be one tumor secure in each well. There exists one actuate-to-close valve at the end of the input channel, which remains closed due to applied pressure in the control layer for the duration of the tumor packing process. The design considerations of the system that impact the valve function the most are membrane thickness, channel width and depth, and shape. The depth and width of the side channels are explicit due to the average size of the tumor spheroids in use. Too small a channel, the tumor wont enter. Too large a channel, fluid flow could shear the tumor past the posts, destroying the spheroid. Therefore, the shape of the valve is the primary point of focus. One system was designed using a standard rectangle as the valve. Due to the depth of the fluid layer channel, however, the weight of the valve can result in sagging, as well, as stickiness between the fluid layer and valve. The weight of the valve may result in a partially-opened channel when vacuum is applied. Additionally, the valves must be strong enough to withstand fluid flow pressures. The second system contains chevron (V-shaped) valves of equal width to their rectangular counterparts. The important feature is that chevron valves contain a failpoint, making them easier to lift from the fluid layer for a completely open channel.
Goals of The Project
The primary objective is to create a microfluidic system capable of packing tumor spheroids using laminar flow control with the assistance of an automated pneumatic valve system. The improved microfluidic device will significantly reduce packing time leading to higher rates of experimentation and decreased turnover time between experiments. As a secondary objective, the system will feature complementary analysis and automation from fluorescence microscopy (Zen) and a systems pressure controller (Elveflow: MUX Quake + OB1). Through channel design in combination with scale-out methods, the device will allow for high throughput drug screening and improved modeling of in vitro tumors.
Synergistic Combination of Modular Lab Tools
In regards to the secondary objective, analysis of experimental results will be improved by automation of certain features within the fluorescence microscope and valve controller. While this aspect of the project increases complexity and demands more user knowledge and experience, the end result is a reduction in manual user operation time. Thus, the chance of user error is decreased and similarly consistency in data collection is improved. This type of system, which utilizes multiple lab devices, is common in cancer research and biological research as a whole; however, the level of desired automation is not as common. In theory, the end goal would be the creation of an umbrella program that unites all modular devices through a uniform programming language (i.e Python, Matlab, Java). This program will be able to run an experiment automatically from tumor packing to data collection and analysis with integrated logic checkpoints requiring binary user input. Moreover, to facilitate both project goals, the Forbes Lab and Perry Lab have purchased a computer-controlled valve actuation system, Mux Quake Valve and OB1 Flow Control System, created by Elveflow. The use of “plug-and-play’ modular devices is a boon for microfluidic applications, as the devices required little set-up time and provide a host of capabilities for flow control within a device. To learn more about these devices, clink the links below:
MUX – Microfluidic Flow Switch Matrices
OB1 – Microfluidic Flow Control System
Scalability of Tumor-On-A-Chip Based Drug Screening
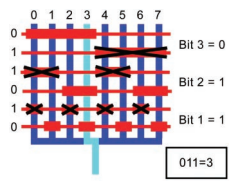
Scaling out can be achieved by creating a binary, multiplexed system which can selectively target single flow channels. The purpose of scaling out is to create a high throughput device, which can handle many tumor spheroids, as well as distribute them into specific channels. Building a high throughput microfluidic system can be a difficult task if the particular device requires selective valve control, but multiplexed systems offer a structured method to accomplish selective valve control. A multiplexed The multiplexed valving system operates using a binary pattern, where n fluid channels are controlled using 2 log2 n control channels. This limits the specific number of controllable channels within a device to be within a binary domain, however, achieving a multiplexed system allows a more organized microfluidic device.
A flow system similar to that on Figure X can be developed to release tumor spheroids into specific channels. A MUX Quake Valve System will be implemented and operated via code written in Python. Devices will be made with 128 flow channels and different 14 valve layers, this will allow handling of tumor spheroids to be conducted in a high throughput manner.
The scalability of a multiplexed system allows for a robust level of design capabilities, and devices could be designed to handle more or less tumors, depending on the experiment. This method is more beneficial to currently used methods because the micro scale nature of these devices result in reduced materials cost and smaller volumes used. Scaling these experiments out will also allow for a much more efficient and less time consuming experiment to be conducted.
References
1. Jemal, A., Bray, F. & Ferlay, J. Global Cancer Statistics: 2011. CA Cancer J Clin 49, 1,33–64 (1999).[1]
2. Neuži, P., Giselbrecht, S., Länge, K., Huang, T. J. & Manz, A. Revisiting lab-on-a-chip technology for drug discovery. Nat. Rev. Drug Discov. 11, 620–32 (2012). [2]
3. Toley, B. J., Ganz, D. E., Walsh, C. L. & Forbes, N. S. Microfluidic device for recreating a tumor microenvironment in vitro. J. Vis. Exp. 5–9 (2011). doi:10.3791/2425 [3]
4. Walsh, C. L. et al. A multipurpose microfluidic device designed to mimic microenvironment gradients and develop targeted cancer therapeutics. Lab Chip 9, 545–554 (2009).[4]
5. Hanahan, D. The Hallmarks of Cancer. Cell 100, 57–70 (2000).[5]
6. Hanahan, D. & Weinberg, R. A. Hallmarks of cancer: The next generation. Cell 144, 646–674 (2011).[6]
7. Liu, X. et al. ROCK inhibitor and feeder cells induce the conditional reprogramming of epithelial cells. Am. J. Pathol. 180, 599–607 (2012).[7]
8. DiMasi, J. a, Reichert, J. M., Feldman, L. & Malins, a. Clinical approval success rates for investigational cancer drugs. Clin. Pharmacol. Ther. 94, 329–35 (2013). [8]
9. Hay, M., Thomas, D. W., Craighead, J. L., Economides, C. & Rosenthal, J. Clinical development success rates for investigational drugs. Nat. Biotechnol. 32, 40–51 (2014).[9]
10. Toley, B. J., Tropeano Lovatt, Z. G., Harrington, J. L. & Forbes, N. S. Microfluidic technique to measure intratumoral transport and calculate drug efficacy shows that binding is essential for doxorubicin and release hampers Doxil. Integr. Biol. (Camb). 5, 1184–96 (2013).[10]
11. Wlodkowic, D. & Cooper, J. M. Tumors on chips: Oncology meets microfluidics. Curr. Opin. Chem. Biol. 14, 556–567 (2010).[11]
12. Nagrath, S. et al. Isolation of rare circulating tumour cells in cancer patients by microchip technology. Nature 450, 1235–9 (2007).[12]
13. Patra, B., Peng, C.-C., Liao, W.-H., Lee, C.-H. & Tung, Y.-C. Drug testing and flow cytometry analysis on a large number of uniform sized tumor spheroids using a microfluidic device. Sci. Rep. 6, 21061 (2016).[13]
14. Sabhachandani, P. et al. Generation and Functional Assessment of 3D Multicellular Spheroids in Droplet Based Microfluidics Platform. Lab Chip 16, 497–505 (2015).[14]
15. Zervantonakis, I. K. et al. Three-dimensional microfluidic model for tumor cell intravasation and endothelial barrier function. Proc. Natl. Acad. Sci. 109, 13515–13520 (2012).[15]
16. Hirschhaeuser, F. et al. Multicellular tumor spheroids: An underestimated tool is catching up again. J. Biotechnol. 148, 3–15 (2010).[16]
17. Miller, O. J. et al. High-resolution dose – response screening using droplet-based microfluidics. Proc. Natl. Acad. Sci. 109, 378–83 (2012).[17]
18. Mohan, R. et al. Design considerations for elastomeric normally closed microfluidic valves. Sensors Actuators, B Chem. 160, 1216–1223 (2011).[18]
19. Thorsen, T. Microfluidic Large-Scale Integration. Science (80-. ). 298, 580–584 (2002).[19]
