Injectable Biomaterials by Sydney Foster
Biomaterials are characterized by their bio-mimetic nature which allows any of these synthetic or naturally derived compounds and structures to be used in the process of replacement or reconstruction of tissues like muscle, bone or even highly differentiated cells like in the spinal column or retinas.[1][2][3]
Injection allows for the precise control of volume of material and allows for easy on the fly filling of space that is unconventionally shaped. Unfortunately injection does not provide full controllability of material composition and until robotics and viewing techniques sufficiently advance, pinpoint accuracy is limited. Because material reliance and toughness are important for structural implants, injectable materials need to harden in situ. While other methods, like surgery or prefabricated replacement can offer a higher degree of specification in regards to patient specific uses, injection offers faster, less intrusive, technically more accurate application of matrix based therapies. Such delicate application allows for solving problems that are embedded in healthy tissue.[4][2][5]
Composition
Many biocompatible materials are available for use in the medical industry today, and many more are on their way. Three classes of injectable biomaterials exist, which have their specific uses for repairing the defects or damages incurred sustained during past trauma. While application methods, namely combination of material with activating agent and injection, are the same for the three classes; their chemical composition and physical properties are varied.[4][2][5][6]
Hydrogel
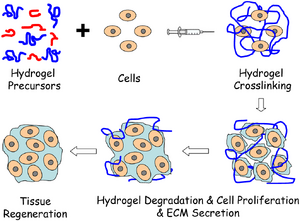
Hydrogels are crosslinked polymer matrices with water included in the 3D space surrounding the polymer backbone of the gel constiuents. The polymers can respond to changes in pH, temperature and pressure by changing size. Different types of molecules, like many organics, can be occluded in the structures and released as the gel degrades. Several methods for inducing crosslinking in hydrogels exist, while the greatest challenge remains finding a method of cross linking in precise increments utilizing an initiator or crosslinker that is bio compatible or does not induce cell death at relevant concentrations.Some molecules can be used to incresae entanglement as a form of pseudo crosslinking, but this is hard to achieve and not as effective as increasing actual crosslinking in the polymer.[1][7][8]
Ceramic
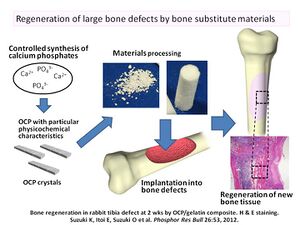
Commonly composed of calcium phosphate, sometimes calcium sulfate, these injectable materials use non thermogenic curing to solidify in situ. These inorganic compounds are extremely biocompatible and because of their miniral composition can be absorbed and used by the body to build viable ECM. Due to the brittle nature of the crystals, these cements can not be used for load bearing fixations or regenerations and are solely used for cosmetic regeneration, like repairing areas around previous fractures or filling in imperfections in teeth.[4][2]
Acrylic
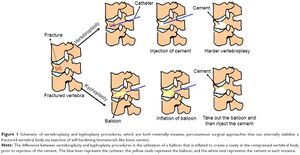
These cements are polymers based on acrylic compounds. Often curing is started with free radical generations via initiator compound and the process uses radical chain addition to finish solidifying the injected material. These cements are stronger than spongy or cancellous bone and can be used to fix joints or repair load bearing bones.[4][2]
Methodology
Hydrogels, ceramics and acrylics can be purchased ready made, and autologous cells are cultured from the patient. Many companies also sell purified growth factors and binding proteins which can be mixed into hydrogel materials for slow release into the surrounding tissue.
Applications is straight forward, requiring that all ingredients be mixed and then quickly injected into the area of concern. Taking too long can cause poor molding of the gel or cement to the area which has the potential of causing damage to the surrounding tissue. Hydrogel mixtures usually have biologics added just prior to mixing in the crosslinking agent. Some hydrogels are thixotropic and do not require crosslinking to maintain toughness.[7][3][4]
It may be difficult to tell exactly how much fluid is being injected and where it is being distributed. Commonly as biomaterials are mixed with a radio opaque agent that allows operators to observe with EM radiation where the material is being injected in the tissue.
Robotics are being developed for significantly improved control over injection rate, angle, and location.[2]
Demand
Because injectable biomaterials cater to repairing or slowing tissue degeneration caused by disease, age and trauma there is a great general demand for these technologies. This demand can be cosmetic, preventative or reactive. Specifically there are over 700,000 cases of vertebral compression fractures yearly caused by osteoporosis alone, fixing these fractures is the main demand for acrylic cements.[4] Researchers are currently discovering just how versatile this technology is when incorporated with cell autologous cell implantation.[3]
Cell implantaion in matrices can be used to treat all range of minor defects, and could potentially be used in utero where they are smallest.[2]
History
1892 Dressman: Plaster of Paris for Bone filling
1941 Kleinschmitt: Acrylic cement for cranial repair
1959 Charnley: Acrylic cement for hip replacement
1970’s examined for cell encapsulation/wound care
2000’s pre/clinical trials for wound healing, joint regeneration, retinal cell regeneration
References
[1] Lee, K.Y.; Mooney, D.J. (2001) Hydrogels for tissue engineering. Chem. Rev. 101, 1869–1879.[1]
[2] Spector, M & Lim TC.(2016). Injectable biomaterials: a perspective on the next wave of injectable therapeutics Biomed. Mater. 11 dx.doi.org/10.1088/1748-6041/11/1/014110[2]
[3] Ballios B G & Cooke M J & van der Kooy D & Shoichet M S (2010) A hydrogel-based stem cell delivery system to treat retinal degenerative diseases Biomaterials 31 2555–64[3]
[5] Discher D E & Janmey P & Wang Y L (2005) Tissue cells feel and respond to the stiffness of their substrate Science 310 1139–43[4]
[4] Lopez, A (2014) Injectable Biomaterials for Spinal Applications, Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Science and Technology (1114)[5]
[6] Macaya D & Ng K K & Spector M (2011) Injectable collagen-genipin gel for the treatment of spinal cord injury: in vitro studies Adv. Funct. Mater. 21 4788–97[6]
[7] Hou, Q.P. & De Bank, P.A. & Shakesheff, K.M.(2004) Injectable scaffolds for tissue regeneration. J. Mater. Chem. 14, 1915–1923.[7]
[8] Marra, K & Tan, H (2010) Injectable, Biodegradable Hydrogels for Tissue Engineering
Applications Materials. 3, 1746-1767[8]
Images:
2: http://www.rpip.tohoku.ac.jp/seeds/uploads/seed-178-3-en.jpg?1417755900
3: https://www.dovepress.com/cr_data/article_fulltext/s85000/85037/img/IJN-85037-F01
