Glucose sensor
Motivation

Glucose sensors have been in use since the 1960's in order to test the blood glucose levels in patients with diabetes mellitus, which is the most popular endocrine disorder of carbohydrate metabolism. Globally, the disease is a dominant source of mortality, especially in most of the developed countries. Cited by WHO (The World Health Organization), 171 million of people around the world had diabietes and predicted to reach 366 million by 2030. A published research announced the number of 6.4% of adults among 20-76 years old affected by diabetes in 2010, that is 285 million individuals. And this statistic will boost to 7.7%, that is 439 million by 2030. Inactive lifestyle mixed with unpleasant eating routine and the rising cases of obesity is determined to be the primary explanation for such upsurge.
Diabetes patients who require insulin, that being all patients with Type 1 diabetes and many with Type 2, need to closely monitor their blood glucose levels to prevent them from going into either hyperglycemia (blood sugar too high) or hypoglymecia (too low). Type 1 diabetics have a defect in their pancreas that causes the pancreas to stop producing insulin, which makes insulin injections a must for Type 1 diabetics. Because of the complete lack of insulin created by their body, Type 1 diabetics will often have to test their blood glucose levels over ten times a day. On the other hand Type 2 diabetics produce insulin but it is often inefficient because of insulin resistance or some other deficiency. As their bodies actually do produce some insulin they do not have to check their blood glucose levels as often, only having to use a glucose sensor between one and four times a day. The two types of glucose sensors that are currently in use today are the blood glucose meter, which is a small handheld device which is used to manually monitor glucose levels, and the continuous glucose monitor, which is used to automatically monitor glucose levels.
History
- Pre-1960’s - Urine strips, first invented by Parisian chemist Jules Maumené, was produced in industrial scale by the company Boehringer Mannheim, known as Roche, in 1960.
- 1962 - First glucose enzyme electrode, created by Leland Clark and Ann Lyons, based on a thin layer of glucose oxidase (GOx) on an oxygen electrode.
- 1965 - First test strips using blood, called Dextrostix, developed by Ernie Adams and produced by Ames Company primarily for doctor's offices [1]
- 1971 - Ames Reflectance Meter, created by Anton H. Clemens, is patented and used in American hospitals in the 1970s [1]
- 1972 - Ames Eyetone Meter, developed by a Japanese company Kyoto Daiichi, is patented in the United States by Ames Company [1]
- 1970’s - Design of continuous glucose monitors begin
- 1980’s - Glucometer and Accuchek, lower cost home glucose meter, sold in home market [2]
- 1996 - Continuous Glucose Monitors first used in a clinical trial by medical technology firm MiniMed in the United States.
- 1990's-2000's - Continuous Glucose Monitors are sold in home market by DexCom, MiniMed, etc.
- 2006 - First continuous glucose monitoring via a device implanted under the skin is released
Blood Glucose Meter
Development History
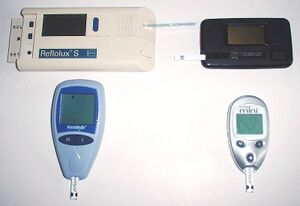
The blood glucose meter is the most common and one of the oldest methods of blood glucose monitoring. The first blood glucose meter was patented in 1971 by Anton H. Clemens and sold by the company Ames under the name, the Ames Reflectance Meter (AMR) [1]. The Ames Reflectance Meter was a heavy piece of equipment, being around three pounds and had a tendency to break down, specifically in regards to the battery leaking. The Ames Reflectance Meter was followed up the following year with the Ames Eyetone Meter (AER) [1], which was a lighter and more effective model. Both of these two original models utilized the Dextrostix, which was also created by Ames. Both of these meters by Ames saw extended use throughout doctor’s offices, but did not see much home use because of the price, $600 for the AMR and $300 for the AER, and the various problems each had [3]. It was not until the 1980’s when glucose meters truly became common in the home market. During this period both the Glucometer and the Accuchek were produced, both of which are the basis for the modern blood glucose meter [2].
Overview
A blood glucose meter is a computerized device for calculating glucose level in blood. Originally, the device had three main parts, the lancet, the meter itself, and the test strip. The lancet is fairly simply in design, with a double edged needle-like blade with a plastic handle and a protective plastic cap. Test strips are about one inch in length and contain a glucose oxidase coating which allows the system to read the glucose levels in the blood. These meters are fairly easy to use and understand. The steps involved are:
1. Wash hands.
2. Place a clean test strip in the meter.
3. Sterilize area of finger being used with alcohol wipe.
4. Prick sterilized area with a new lancet and safely dispose.
5. Gently put pressure on finger to produce blood and place on strip.
6. Wait for reading then safely dispose of test strip.
Recent advances
- 'reduce in size and waiting time', only need a tiny drop of blood for the meter, original size reduce from 30 to 0.3 μI, original test times reduce from 2 minutes to 5 seconds ( modern meter are normally under 15 seconds)
- 'multi-test function', a few devices practice with multiple test strips by compiling in a cartridge or a disc
- 'varying in testing site', other than finger, now blood could be taken from palm or forearm, which is painfree and give those finger tips relaxation in case of aching. However, blood flow at these sites are usually less dense, accordingly lead to inaccuracy when sugar level in blood adjusts.
- 'digitalize meters', latest versions of the device is offered with a software that data can be downloaded and sync with computers. This method helps improving health management and diabetes control significantly
- 'no-code systems, result in avoidance of 'mis-coding'. Some machines use 'auto-coding' method, which individually code each strip to the device. Others produced only with a 'single code'.
Continuous Glucose Monitoring System
Overview
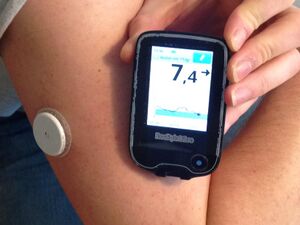
A continuous glucose monitor serves the same basic function as a blood glucose meter, in that it is designed to measure the glucose levels in the blood. The difference however is rather than manually read the blood glucose level once, a continuous glucose monitoring system automatically measured and displays the blood glucose level [10]. A continuous glucose monitor can spit out glucose readings every 5 minutes to every minute and is capable of alerting the patient using an alarm if the blood glucose levels are either too high or too low. This makes it much more versatile than the standard blood glucose meter, which can only be used a certain number of times each day.
A continuous glucose monitor is implanted into the skin, generally in the abdomen. Thereafter the monitor can be kept in the body for up to six days before it must be replaced. Then they link the monitor to an external transmitter that also wirelessly connect with a receiver. This receiver has a screen to demonstrate glucose levels in real time and monitor rising as well as falling trends. [11]
However, these monitors have been found to not be as reliable or accurate as manual blood glucose meters. Firstly, continuous glucose monitor occasionally require an extra item call "finger stick" because the device have to calibrated with a blood glucose measurement. Secondly, the measurement of glucose level in blood using continuous glucose monitor have a lag time, consequence in a false value [13][14]. For these reasons, the device is not as widespread as manual blood glucose monitor. Also, continuous glucose monitors are not covered by most health insurance providers which makes them much more difficult for most people to acquire. Because they are difficult to obtain continuous glucose monitors are used to test for trends in blood glucose levels and blood sugar levels rather to monitor blood glucose levels on a day to day basis. [4]
Availability

In the market, there are three continuous glucose monitor on sale. The first one is from Dexcom company, called CGMS (Continuous Glucose Monitor Systems) with two different versions G4 and G5 [12]. Dexcom CGMS G4 works through radio frequency and need an external receiver. On the other hand, Dexcom G5 makes use of Bluetooth to transmit data directly from nearby cellphone, but currently only accept Apple's iPhone. Minimed Paradigm RTS by Medtronic is the second one that connected with a transmitter size of a coin to estimate interstitial to a receiver every 5 minutes. Abbott Laboratories made the third CMGS, named FreeStyle Navigator. Although the demand of these devices are usually tremendous, espcially in developed countries, the price stil exceed the standard affordability level.
Future Research
Research is currently underway on a continuous closed-loop drug delivery system that can be implanted under the skin. The idea behind this system is to be able to read the blood glucose levels and then automatically dispense insulin into the body without human assistance. They are small, approximately 1 inch in length and less than 0.25 inch in diameter. These systems are in the preliminary research stage involving animal testing and have not yet shown the ability to be viable for more than a few days. [7]
Non-invasive Glucose Monitor
There are currently several efforts to patent a non-invasive glucose monitor, that is a monitor without the need to carry on the blood glucose analysis with a drop of blood. That is to say, the patient will be free from pain. Beforehand, there is the GlucoWatch G2 Biographer created by Cygnus Inc., which is a non-invasive glucose meter approved by U.S FDA, showed up in the market. The device used electric fields to draw out body fluid for exmination, but couldn't deal with perspiration at analysis area. Therefore, it is no longer available because of these mal-functions and also have lots of drawbacks.
Most of the the non-invasive glucose monitors in progress are Continuous Glucose Monitor System. They provide with additional data to experimental targets between the finger stick, blood glucose analysis and real time period where no finger stick assessment is applicable. [9]
Digital Era
Put forth by the astounding development of digital technology, glucose meters with cellular data transmitting capacity are available. An E-tech award invention and displayed at the 2010 CTIA International Wireless Expo, from Telcar Inc., was able to process the information from a medical caregiver and collected instant guidance from the caregiver on the meter's screen. Still, it is presently undergoing laboratories testing.
Some of CGM systems available under combination with cell phone, can be named as "Glugophones", are provided in three versons: an adaptor for iPhone, add-on pack for LG versions of UX5000, VX5200, and LX350, in addition with add-on pack for Motorola Razr cell phone. In the U.S, they are provided only by AT&T and Verizon.
Contact lenses, which are able to adjust glucose levels and notify users when glucose level exceed cetain thresholds, are presented by Google in the early 2014 [8].
References
- [1] "Ames Reflectance Meter and Dextrostix." Web. 05 Apr. 2012. [1].
- [2] "Blood Glucose Meter History." BG Meter History.... Insight into the History of Blood Glucose Monitors. Web. 05 Apr. 2012. [2].
- [3] "History of Blood Glucose Meters." David Mendosa: A Writer About Diabetes. Web. 05 Apr. 2012. [3].
- [4] "National Diabetes InformationClearinghouse (NDIC)." Continuous Glucose Monitoring. Web. 05 Apr. 2012. [4].
- [5] Oliver, N. S., C. Toumazou, A. E. G. Cass, and D. G. Johnston. "Glucose Sensors: A Review of Current and Emerging Technology." Diabetic Medicine 26.3 (2009): 197-210. Print.[5]
- [6] "Continuous Glucose Monitor." Blood Glucose Monitor & Ing. Web. 05 Apr. 2012. [6].
- [7] Gordijo et al. (2010). "Nanotechnology-Enabled Closed Loop Insulin Delivery Device: In Vitro and In Vivo Evaluation of Glucose-Regulated Insulin Release for Diabetes Control” Advanced Functional Materials [7]
- [8] Mendoza, Martha (January 16, 2014). "Google develops contact lens glucose monitor" [8]
- [9] A. Tura, A. Maran, and G. Pacini, “Non-invasive glucose monitoring: Assessment of technologies and devices according to quantitative criterion," Elsevier J. of Diabetes Research and Clinical Practice, vol. 77, no. 6, pp. 16-40, 2007 [9]
- [10] J. Wang (2008). " Electrochemical Glucose Biosensors" Chem. Rev., 2008, 108 (2), pp 814–825. [10]
- [11] Y. Zhao; S. Li; A. Davidson; B. Yang; Q. Wang; Q. Lin (2007). "A MEMS viscometric sensor for continuous glucose monitoring". J. Micromech. Microeng. 17: 2528–2537. [11]
- [12] Dexcome G4 product website. Retrieved 2016-01-30 [12]
- [13] Lipkowski, J., Kolb, D. M., & Alkire, R. C. (2011). Bioelectrochemistry : Fundamentals, Applications and Recent Developments. Weinheim: Wiley-VCH. [13]
- [14] Leigh, Simon; Idris, Iskandar; Collins, Brendan; Granby, Paul; Noble, Max; Parker, Mark (Nov 2015). "Promoting health and reducing costs: a role for reform of self-monitoring of blood glucose provision within the National Health Service". Diabetic Medicine. 33 (5): 681–90. [14]