Dialysis, by Kyle Reed and Brian Kennedy
Background
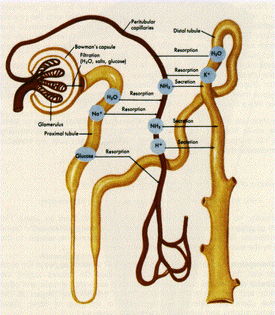
The kidneys are essential organs, playing vital roles in both the urinary and endocrine systems. They maintain the chemical and water balance of the body with the help of nephrons, which are the functional units of the kidney that remove waste from the blood. Nephrons accomplish this through filtration and both active and passive transport; each kidney has approximately 1 million nephrons. Figure 1 shows a nephron and the processes that occur [1][2][3].
It is important to note that the blood enters the nephron at the glomerulus, which filters solutes up to 60,000 Da in size. The glomerular filtration rate (GFR) for an average person is roughly 125 mL/min, or 180 liters/day. The resulting fluid and solutes then enter the renal tubes, where different types of transport occurs [1][2].
In the proximal tube (first part of the renal tube), water is reabsorbed back into the blood stream: around 178 liters/day. Other substances are also reabsorbed, such as sodium and glucose. Glucose is always fully recovered while sodium is regulated; depending on the electrolyte concentration within the bloodstream sodium is either reabsorbed or secreted [1].
The substances that were not filtered out in the glomerulus, like hydrogen and potassium ions, ammonia, and certain drugs, enter the peritubular capillaries. These components are then secreted into the distal tubule (second part of the renal tube). The toxins are then sent to the bladder with the ~1% of water that wasn't reabsorbed [1].
The kidney also has other important functions by sensing the composition of the blood and secreting substances that aid in bone metabolism, red blood cell production, and blood pressure regulation [2].
Renal Failure
Renal failure is when the kidneys are no longer able to function as needed, and can be classified as either acute or chronic. Acute renal failure is characterized by a sudden and unexpected onset, and can be caused by a number of things including a drug overdose, severe dehydration, a physical injury to the kidneys, or even an autoimmune attack. Chronic renal failure is a slower process where the kidneys gradually lose functionality over time. It can be caused by things such as renal cancers, diabetes, and hypertension. Both cases of renal failure require the patient to be treated with dialysis, so that toxins to not accumulate in the bloodstream, therein poisoning the patient.
History of Renal Treatment


1854 - Thomas Graham developed an apparatus that held urine and water separated with a membrane. After several hours, sodium chloride and urea were found to have transported across the membrane. Set the basis for dialysis. [4]
1924 - Georg Haas performed first human hemodialysis on a uremic patient. [4]
1937 - First flat hemodialysis membrane made of cellophane produced. [4]
1940 - Willem Kolff takes interest in acute renal failure. [4]
1943 - Kolff created dialysis machine using sausage casings, washing machine, and orange juice cans. Treated 15 patients with little to no success. [4][5][6][7]
1945 - Kolff treated a 67 year old woman with longer dialysis time and she survived for another seven more years. [5]
1947 - Kolff donates his dialysis machines to other hospitals, allowing other doctors to learn the design of the machine and improve upon it. [5][7]
1948 - First hermodialysis machine constructed in the US to be used at Peter Bent Brigham Hospital. [5]
1954 - First kidney transplant. [7]
1960 - Belding Hibbard Scribner invented the Scribner shunt, preventing the numerous incisions required for dialysis. [7]
1962 - Scribner opened the first outpatient dialysis facility. [7]
2013 - Rat kidney effectively grown through decellularization [16]
2017 - Clinical trials of artificial kidney expected to commence. [17]
Current Dialysis Technology
Present day renal failure treatments are not perfect solutions to renal failure because they does not replace the kidney’s compromised endocrine functions. The kidney produces erythropoietin and calcitriol, hormones that play a vital role in the formation of red/white blood cells and bone formation, respectively, and these functions cannot be mimicked through dialysis. There are two types of dialysis used to treat renal failure: hemodialysis and peritoneal dialysis. Hemodialysis is performed on about 85% of patients, with the remainder being peritoneal dialysis [2][15].
Hemodialysis
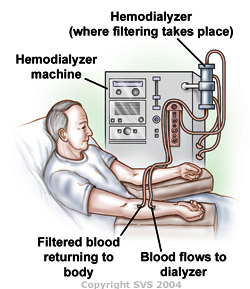
Hemodialysis involves direct dialysis of the blood. Blood is removed from the patient and pumped through a machine (dialyser) that acts as an artificial kidney, removing toxins and impurities before injecting the cleaned blood back into the patient. Because the dialysis machine is not part of the patient's body, anti-coagulates need to be mixed in with the patient's blood. The blood is accessed with the help from either a catheter, an arteriovenous (AV) fistula, or an AV graft; fistulas are more common. An AV fistula is where a patient's artery is directly connected to their vein due to a surgical procedure. This allows for high blood flow, and leads to fewer complications and infections than other methods of access like grafts and catheters [2].
Blood is pumped into the dialysis machine at a rate of 50 to 500 mL/min, depending on the patient's renal condition. Once in the dialyser, the blood is pumped into a chamber where the dialysis fluid (dialysate) is flowing counter-currently, separated from the blood stream by a synthetic membrane. Hydrostatic pressure and concentration gradients cause the majority of uremic toxins in the blood to flow across the membrane and into the dialysis fluid. The purified blood is then fed back into the patient. The dialysis fluid flow can be done in either a batch or continuous manner, but either way the procedure needs to be closely monitored. Any error in the mixing will cause the wrong concentration gradients to form for the patient. On average, patients who require hemodialysis need to get their blood purified three times a week, with 3-5 hour sessions [2].
Peritoneal Dialysis
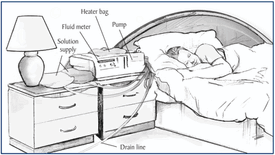
Unlike hemodialysis, peritoneal dialysis occurs in the peritoneal cavity. Surrounding the cavity is the peritoneum, which is a thin membrane that forms a closed sac around the abdominal organs. The patient has a permanent cannula or catheter in place, which allows dialysate to flow in and out of the cavity. The peritoneum allows transfer of solutes from the blood, and after a certain time has passed, the dialysate will flow out of the cavity and into a drain pipe. This form of dialysis is not as efficient as hemodialysis, with the dialysis cycle to take around 30 minutes and the entire process to last 8 to 12 hours [2].
Although less effective than hemodialysis, many prefer peritoneal dialysis because this process occurs in the comfort of one's own home. Due to the procedure length, it is usually done at night when the patient is asleep. Another advantage is that the patient's blood never comes into contact with a foreign source, taking anti-coagulates out of the equation. There are a few disadvantages with the this type of dialysis however. The peritoneum is very sensitive, and peritonitis can be caused if something were to go wrong with the cannula, catheter, or dialysate itself. Also, permanently having a catheter on your body can greatly limit the patient's range of activities, such as going to the pool or taking baths [2].
Automated Peritoneal Dialysis
Automated peritoneal dialysis (APD) is a type of PD in which a machine manages the dialysis fluid exchange while the patient sleeps. This typically involves 3-10 cycles per night, depending on patient’s health. This is a less obtrusive form of treatment, allowing the patient to live his or her life without lengthy appointments multiple times per week. However, difficulties sleeping has been reported by many receivers of APD treatment [14].
Continuous Ambulatory Peritoneal Dialysis
Continuous ambulatory peritoneal dialysis (CAPD) is PD in which 2 liters of fluid are kept in the abdomen at all times, and the patient exchanges the fluid 4-6 times per day. Like APD, this method of treatment is beneficial in that it does not require visits to a dialysis facility.
Future of Dialysis
Nephron Regeneration
Human nephrons can only regenerate partially; we are not able to grow new ones. Fish are able to grow new nephrons however, and zebrafish have been extensively studied in order to attempt to emulate their kidney cells' ability to self-replicate. Research has found that zebrafish kidneys likely contain self-renewing nephron stem/progenitor cells. Future research into this field might allow scientists to restore nephron functionality in humans [10].
Kidneys from Decellularized Tissue
Researchers at Massachusetts General Hospital have grown a functioning rat kidney, with the future hopes of using this technology to provide organ replacements to human patients with end stage renal failure. The kidney was able to produce urine in vitro as well as in vivo for a short amount of time [16].
For the technique being developed, donor tissue is decellularized before being used to grow a new kidney. The idea behind decellularization is to strip the donor tissue of the cells that would make it trigger an immune response in a transplant patient. The cells are washed off using a variety of bases, leaving behind a scaffold of structural proteins. The kidney scaffold is then seeded with a mixture of the patient's stem cells, which are hoped to differentiate into functioning kidney tissues [16].
Next step is to scale-up into larger animals. If successful in larger animals, then clinical trials can proceed. In the UK, their more permissive regulations and socialized healthcare system will allow for faster development and testing than in the United States, and could be a viable treatment option in as little as 5 years [16].
Artificial Kidney

There has been long debate about whether the technology would be created that will allow humans to bypass dialysis and "wear" an artificial kidney that is cheap in the near future [11]. Researchers at the University of California San Francisco (USCF) are looking to develop such a device. A prototype artificial kidney that requires no power source has been developed. The device filters blood using advanced silicon nanoporous membranes, which are more efficient than conventional polymer membranes used in contemporary dialysis settings. The device also contains a bioreactor that houses engineered renal tubular cells. These cells are hoped to replace kidney functions like the maintenance of water and electrolyte levels in the blood. It is hoped to eventually have an operational lifetime of around a decade [17].
Currently, small prototypes have been successful in animal hosts (pigs, sheep, and rodents) for short periods of time, and the next step is the construction of larger prototypes for eventual clinical trials. The first clinical trials for this device are planned for 2017, and the device itself is on an accelerated track for FDA approval [12][17]. (See source for video on the device).
Impact
It is apparent that the the research approaches described above could have a dramatic impact on the lives of patients suffering from chronic or acute renal failure. Whether it be allowing them to regrow an entire kidney, or have an artificial one instead, kidney engineering can allow people to live their lives without the worries of having to spend countless hours near a dialysis machine to survive. However, these technologies could prove to be even more important for those that are not even able to have dialysis due to financial restrictions.
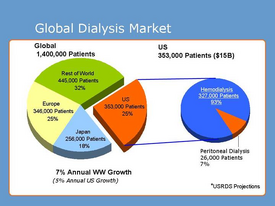
Figure 7 shows the global market for dialysis as of January 2013. The "Rest of World" portion has been amplified with the growing market in India. Currently, there are 52,000 Indian patients on dialysis, but this is nowhere near the amount of people that require it. While dialysis in India costs 4 to 33 percent of the cost in the U.S., more than 90 percent of the 230,000 that develop chronic kidney failure each year are unable to acquire treatment [13].
References
[1] Space Biomedical Research Institute. http://home.bway.net/rjnoonan/humans_in_space/fluid.html (accessed February 6, 2013).
[2] Ratner, B.D.; Hoffman, A.S.; Schoen, F.J.; Lemons, J.E. Biomaterials Science: An Introduction to Materials in Medicine, 2nd ed.; Elsevier Academic Press: San Diego, 2004; pp. 514-518.
[3] Saltzman, W. Tissue Engineering: Principles for the Design of Replacement Organs and Tissues; Oxford: New York, 2004; pp. 387-391.
[4] Advanced Renal Education Program. http://www.advancedrenaleducation.com/Hemodialysis/HistoryofHemodialysis/tabid/177/Default.aspx (accessed February 6, 2013).
[5] The Kidney Doctor. http://www.thekidneydoctor.org/2012/02/remembering-willem-kolff.html (accessed February 6, 2013).
[6] $100 Dialysis. http://100dialysis.wordpress.com/2012/01/24/a-brave-beginning/ (accessed February 6, 2013).
[7] DaVita. http://www.davita.com/kidney-disease/dialysis/motivational/the-history-of-dialysis/e/197 (accessed February 6, 2013).
[8] VascularWeb. http://www.vascularweb.org/vascularhealth/Pages/dialysis-access.aspx (accessed February 6, 2013).
[9] National Kidney and Urologic Diseases Information Clearinghouse. http://kidney.niddk.nih.gov/kudiseases/pubs/peritoneal/
[10] Diep, C.Q.; Ma, D.; Deo, R.C.; Holm, T.M.; Naylor, R.W.; Arora, N.; Wingert, R.A.; Bollig, F.; Djordjevic, G.; Lichman, B.; Zhu, H.; Ikenaga, T.; Ono, F.; Englert, C.; Cowan, C.A.; Hukriede, N.A.; Handin, R.I.; Davidson, A.J. Identification of adult nephron progenitors capable of kidney regeneration in zerbrafish. Nature. 2011, 470, 95-100.
[11] Ronco, C.; Davenport, A.; Gura, V. A wearable artificial kidney: dream or reality?. Nature Clinical Practice. 2008, 4, 604-605.
[12] medGadget. http://www.medgadget.com/2012/11/an-implantable-artificial-kidney-interview-with-ucsfs-dr-shuvo-roy.html (accessed February 6, 2013).
[13] The Kidney Doctor. http://www.thekidneydoctor.org/2013/01/global-nephrology-dialysis-in-india.html (accessed February 6, 2013).
[14] Crowley, LV (2009). An Introduction to Human Disease: Pathology and Pathophysiology Correlations. Jones & Bartlett Publishers. pp. 507–509.
[15] Brundage D. Renal Disorders. St. Louis, MO: Mosby; 1992.
[16] Birchall, Martin. "Artificial Kidney Transplants 'in Five Years'" Interview. BBC Radio 4's Today Programme. BBC. London, 15 Apr. 2013. Radio.
[17] "Device - School of Pharmacy." Device - School of Pharmacy. http://pharmacy.ucsf.edu/kidney-project/., n.d. Web. 05 Feb. 2014.
