Degradable Sutures, by Cody Siroka
Background
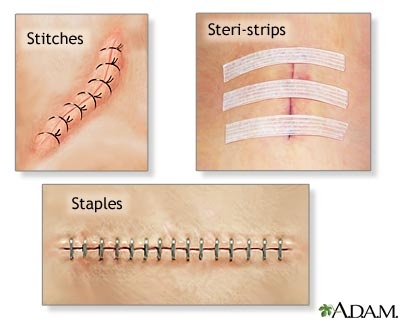
Sutures, or stitches, are a type of medical device used to close wounds and restore tissue alignment during the healing process after surgery or trauma. [1] Degradable, or absorbable sutures can be broken down by the human body without the need for external removal, and are characterized by their loss of 50% or more of their tensile strength within four weeks after implementation. [2] Degradable sutures can be made from both synthetic polymers and natural sources. Sterility is important during both the manufacture and usage of these devices to minimize the event of infection as a result of the introduction of foreign materials into the body.
The specific type of suture used in treatment is selected with respect to tissue subject to treatment. Some important aspects of consideration during treatment include the necessary structural integrity and tensile strength, toxicity, and scar formation. Sutures have been implemented in practice for thousands of years, and are attributed to a market of about $1.3 billion annually. They are the most widely used method to close wounds in practice. [1]
Suture Classification
The Food and Drug Administration (FDA) regulates the production of sutures because their usage within the body classifies them as medical instruments or devices. There are three classes of sutures:
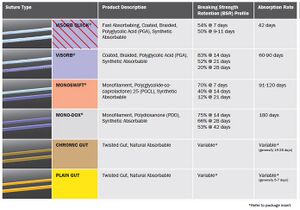
Class I Silk or synthetic fibers, monofilament
Class II Cotton or linen fibers, or coated synthetic or natural fibers
Class III Metal wire, monofilament or multifilament
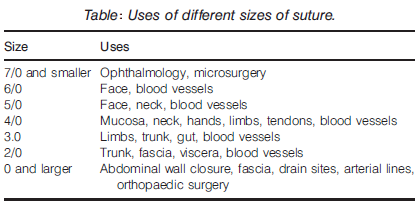
Sutures are also classified based on strand diameter, which helps to denote their application.
History
Some noteworthy events listed in the development and usage in sutures as they occurred chronologically throughout history. Only major or significant events are listed.
3500 BCE – The use of sutures is found in Egyptian scrolls for medical intervention using materials such as animal hairs, vegetable fibers, and linen. [9]
500 BCE – A written, detailed account of sutures found in Sushrita Samhita.
30 CE – Roman medical journalist Aurelius Corneliun Celsus discussed the use of sutures in De Re Medicina. [7]
131–211 CE – The greek Claudius Galen described the use of chorda (catgut) as suture material. [1], [4],[7]
300 CE – The greek Antyllus used chorda material for surgeries, including traumatic aneuyrsms. [1]
700 CE – The use of dried sheep intestine as suture material is found in Vagbhataratha Kaumudi and similar works. [1]
1500 CE – The French Ambroise Pare´ performs multiple surguries for vascular ligatures using linen strips and silk. [1],[7]
1860 CE – Joseph Lister proposes catgut sutures [1],[7] and proves their utility.
1908 CE – The start of manufacture of sterile catgut. [10]
1935 CE – The first non-degradable suture becomes a commercial product available in the medical industry. [10]
1950 CE – Sterilization through radiation becomes well established and is applicable in the use of sutures. [10]
1970 CE – The first absorbable synthetic suture is created and used in the medical industry.[10]
Motivation
Sutures are important in promoting the healing process in damaged tissue and preventing further complications. Degradable sutures are useful in many wound closing applications, especially when the wound is minor. It is important that the best possible suture material is chosen based on the type of wound, bodily location, and other factors. For example, to minimize potential scarring where cosmetic implications are considerable, the smallest suture materials are generally chosen. The materials used to manufacture these sutures dictate the type of immune response, biocompatibility, and mechanical properties, consequently influencing wound treatment.
Usage and Injury Recover
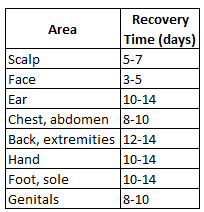
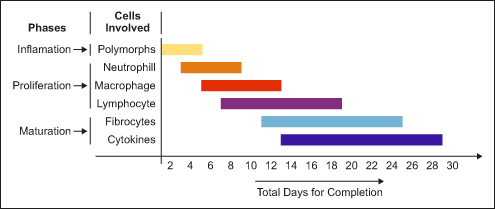
Lacerations to the skin are a common occurrence in which the use of absorbable sutures may be considered. Any, or all layers of the skin – epidermis, dermis, subcutaneous layer, and the deep fascia are all of concern in the event of damage to the skin. The deeper an injury, the more likely sutures will be considered for treatment. Internally, sutures are also used, such as in oral surgery, depending on the size of laceration and probability of complication. As with any injury, the wound must avoid becoming infected, and ideally have as minimal scarring as possible. For external wounds, it is common practice to cover the wound in an antibiotic with a wound bandage. [11] There are several overlapping phases involved in wound healing, and the proper use of sutures can help speed the process. The appropriate use of sutures will shorten the amount of time that the body will need for each phase.
Suture Materials
Degradable suture materials can be either organic or synthetic. There are many types of materials which have been used over course of their development that are absorbed by the human body. Absorbable sutures tend to be reserved for use inside the body underneath the skin as they are prone to leave a more pronounce scar upon absorption. When later removal poses potential difficulty, their use may be exhausted. For synthetic materials, it is desirable that there is no toxicity associated with its usage, is metabolized fully, long-lasting shelf life, easy to manipulate, and is sterilizable. Many factors affect the performance of a synthetic material, which consequently yields variations among molecular weight, molecular weight distribution, hydrophobicity, and crystallinity. [8] One dozen catgut suture of 18", 23mm 1/2 circle reverse cutting costs $27.30, and one dozen of mono synthetic sutures of 18", 3/8 circle reverse cutting costs $68.52. [12]
This list encompasses the most commonly used materials today.
Natural
Catgut
Derived from the walls of animal intestines, including sheep, goat, and cattle, among other animals. It is from the submucosal layer in sheep, or the serosal layer in cattle, found within the small intestine. [1] As it is a material derived from a natural source, it is subject to variations among the material’s chemical structure, which can cause weak points within the material due to the potential lack of uniformity. For this reason, catgut is manufactured in a multifilament fashion to ensure integrity during use. Catgut loses strength rapidly following implementation; approximately 60% of its tensile strength is lost following the first week (4), and continues to diminish until it is broken down by the body completely. Chromic salt coatings on the catgut can prolong the strength of the material and minimize adsorption time. The mechanism by which the degradation of catgut occurs is by proteolytic enzymes found in phagocytes, wherein macrophages, lymphocytes, and other cells accumulate to replace areas within the suture, and eventually, dense accumulations of macrophages replace the suture fully.
Reconstituted Collagen (RC)
Used exclusively for microsurgery, RC is similar to catgut in that it is prepared from an animal source, but differs in its “polymorphic, aggregated form.” (5) This type of material is from long flexor tendons of cattle, and is processed and extruded into coagulated fibrils, and treated with chromic salts.
Synthetic
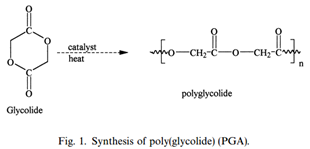
Polyglycolic Acid (PGA)

Synthetic homopolymer of glycolic acid in a braided multifilament. PGA has a uniform chemical structure, produced by the reaction of glycolic acid with glycolide to create linear polymer chains. The monomer of glycolide is created from the dimerization of glycolic acid in a ring opening polymerization, which does not occur in most organic solvents. The polymer is then processed in particular methods to create suture material with the desired physical properties, where it is subject to heat treatment. The homopolymer must be braided into a multifilament because PGA fibers are otherwise too stiff and strong for usage. The synthetic material is more uniform than its naturally-derived counterparts, and is broken down in the body by hydrolysis. PGA maintains 55% of its initial tensile strength 2 weeks after implementation [4], lose all strength by 4 weeks, and are fully absorbed after 4-6 months [8].
Poly(lactide-co-glycolide) (PLG)
Result of the copolymerization of two monomers, lactide and glycolide. Different stereoisomers of these monomers yield changes in physical properties. Glycolide has a tendency to be amorphous due to the disruption in the regularity of the polymer chain with the combination of another monomer. Similarly, other materials such as trimethylene carbonate can be combined with PGA to create materials with changes in flexibility, and absorption time. [8]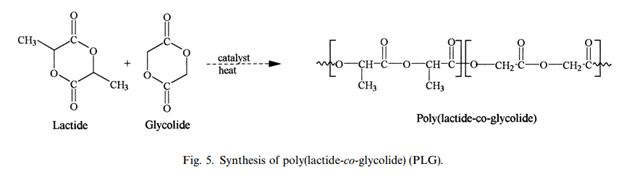
Polyglycan 910
Synthetic heteropolymer of 90% glycolide, and 10% lactide. This type of material is more pliable than other synthetics. The production of polyglycan utilizes a catalyst, where the materials are melted and extruded into fibers and treated. The degradation of polyglycan is by hydrolysis. Coatings may be used to improve handling of the material. The retention of tensile strength is comparable to that of PGA, where polyglycan may be a bit greater [4].
Polydioxanone (PDS)
Synthetic homopolymer, prepared through the polymerization of the monomer paradioxanone, which is melt excluded into a monofilament. The synthetic material is again broken down by hydrolysis. Two weeks after implementation, it retains approbimately 70% of its initial tensile strength [4], and maintains its strength quite well compared to other materials, which implies that this material is preferred for wounds which are closed with tension.
Future of Degradable Sutures
Wound closure technology has some developments with means of closure other than physical sutures. One example is laser welding, in which laser energy is manipulated to seal open wounds in a manner similar to cauterization. The process is fast, yields no immune response due to foreign particles in the body, and is free of water. The treatment, however, can lead to thermal injury. As a means to combat this, laser soldering, which uses similar technology and means to close wounds has also been studied. Using an albumin solder, animal testing has proven positive results to spot treat wounds in temperature controlled conditions, which produced skin recovery with similar tensile strength to that of sutured cuts. [8] Many studies exist in literature for these laser technologies in both animal and human subjects. However, clinical studies are somewhat limited, but there is much potential for their usage in practice.
References
[1] Pillai, CK and Sharma, CP. 'Review paper: absorbable polymeric surgical sutures: chemistry, production, properties, biodegradability, and performance." J Biomater Appl. 2010 Nov;25(4):291-366. doi: 10.1177/0885328210384890. Epub 2010 Oct 22. <http://jba.sagepub.com/content/25/4/291.full.pdf+html>
[2] Murtha AP, Kaplan AL, Paglia MJ, Mills BB, Feldstein ML, Ruff GL. Evaluation of a novel technique for wound closure using a barbed suture. Plast Reconstr Surg. 2006;117(6):1769-80.
[3] Pravin, KRD; Phadke, Shweta, and Rumde, Amita. "Using Trends of Evolution to Direct Wound Treatments." The Triz Journal. Oct 2007. <http://www.triz-journal.com/using-trends-of-evolution-to-direct-wound-treatments/>
[4] Roenigk, Randall K., John L. Ratz, and Henry H. Roenigk. Roenigk's Dermatologic Surgery: Current Techniques in Procedural Dermatology. New York: Informa Healthcare, 2007. Print.
[5] Dumitriu, Severian. Polymeric Biomaterials, Revised and Expanded. Boca Raton, FL: CRC, 2013. Print.
[6] Beidas, Omar E. "General Surgery Suture Needles." General Surgery Suture Needles. Ed. Vikram Kate. Medscape, 23 July 2013. Web. <http://emedicine.medscape.com/article/2044501-overview>.
[7] Mackenzie, David. "The History of Sutures." Medical History 17.02 (1973): 158-68. Print.
[8] Middleton, John C., and Arthur J. Tipton. "Synthetic Biodegradable Polymers as Orthopedic Devices." Biomaterials 21.23 (2000): 2335-346. Web.
[9] UT Southwestern Medical Center. "Hydrogen Peroxide Could Cause Absorbable Sutures To Come Apart, Researchers Report." ScienceDaily. ScienceDaily, 5 August 2007. <www.sciencedaily.com/releases/2007/07/070731085507.htm>.
[10] Prodivet Pharmaceuticals. "The History of Surgical Thread." <http://www.prodivet.com/en-GB/Products/Surgical-threads/The-history-of-surgical-thread.aspx>. Accessed 10 Feb 2015.
[11] DeLemos, David. "Closure of Skin Wounds with Sutures." Closure of Skin Wounds with Sutures. Ed. Anne M. Stack and Allan B. Wolfson. UpToDate, n.d. Web. 12 Feb. 2015. <http://www.uptodate.com/contents/closure-of-skin-wounds-with-sutures>.
[12] Havel Brand Sutures. http://www.havels.com/
