Artificial Vertebrae, by Andy Kim, Daniel Kosteva, Matthew McNulty
Motivation
The vertebral column is an essential structure in the human body. The column protects the spinal cord, a key component of the central nervous system. The protection comes in the form of shielding from impact, pinching, and other sources of trauma. Beyond protection, vertebrae provide sites of attachment for muscles, ligaments, and bones, specifically for ribs in the thoracic curve, all of which work in synchronization to allow mobility and structural stability for the body. [1]
Artificial vertebrae provide an alternative to traditional spinal fusion. Spinal fusion is the process of fusing multiple vertebrae together in order to immobilize a vertebra that is causing pain by abnormal motion. The motivation for development of artificial vertebrae is to replace human vertebrae injured due to fractures, tumors, and disease. These conditions affect the structure and decrease stability of the vertebral body (column) as a whole, as well as affecting the vertebra’s height. [25]
There are many medical issues involving the vertebral column, including scoliosis, kyphosis, disc inflammation and slippage, and degenerative diseases such as arthritis. [1] Implications from such conditions, along with damage from fractures and tumors, can yield severely damaged vertebrae. Artificial vertebrae would provide such patients a normal, healthy life. [2]
Background
Vertebral column
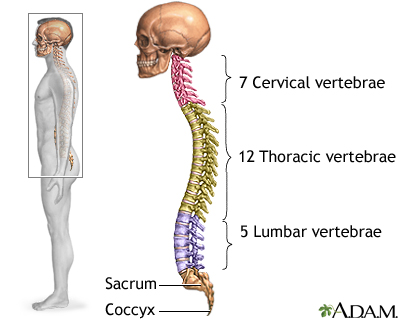
Adult humans generally possess 33 vertebrae, 24 articulating and 9 fused, which compose the vertebral column. The column itself is defined in five regions. [3, 27] From top to bottom:
- cervical curve - 7 articulating vertebrae making up the neck
- thoracic curve - 12 articulating vertebrae in the chest with ribs attached
- lumbar curve - 5 articulating vertebrae supporting torso and head weight [4]
- sacral curve - 5 vertebrae that fuse with age caged in the pelvis
- coccyx - 4 vertebrae fused with age remnant of a vestigial tail [3, 27]
Individual Vertebra
Individual vertebra differ significantly depending on the region of origin in the vertebral column. However, there are general structural characteristics of individual vertebra that enable full function.
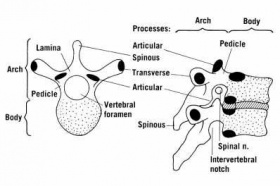
Each individual vertebrae is made up of a core of low density, cancellous bone enclosed by a shell of stiffer, more dense cortical bone. [26]
The vertebral body is the largest structure of the vertebra. It serves as the main weight bearing area, taking about 80% of the load while standing. As so, the vertebral body increases in size each vertebra from the head down. The body also provides attachment for the cushioning discs between the vertebrae. The anterior body additionally gives protection to the spinal cord. [5]
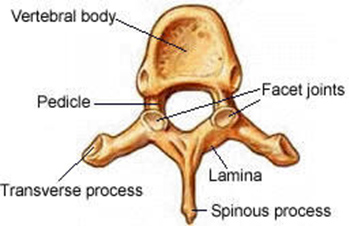
The pedicles are two projections from the posterior vertebral body that provide side protection to the spinal cord. The pedicles help form the spinal canal as well as bridge the body to the rest of the vertebra. [5]
The lamina are flat plates that form the spinal canal and provide further support and protection for the spinal cord. [6]
The spinous process is a projection perpendicular to the lamina. Each spinous process is connected by ligaments to those above and below it in the vertebral column as well as being the site for important muscle connections necessary for movement and stability. These are the noticeable bumps you can feel running your hand down your spine. [6]
The transverse processes extend out towards the sides of the vertebra and provide additional attachment sites for ligaments and back muscles. These are normally absent in the cervical curve. If present, they often impair nerve roots and cause pain. [5]
The facet joints interlock with those above and below it to provide stability and at the same time mobility. Each vertebra possesses four facet joints, two superior and two inferior. The interlocking facet joints are surrounded by a synovial capsule to prevent grinding. [5]
The spinal canal is made up from various parts of the vertebra. The canal is a bony tunnel that surrounds the spinal cord and nerve roots for protection.
History

- 1902 – experimented with steel rods and wire anchored to spine with autographs. [7]
- 1911 – Robert Hibbs performed first formal spinal fusion operation. [7]
- 1931 – Hibbs modifies the operation to achieve 20% success rate after performing 360 cases of spinal fusion. [7]
- 1950 - Improvements in post-operative treatment and success rates (Joseph Risser creates frame that applies pressure to rib cage and allows for immediate correction of spinal alignment after surgery and allows patients to be mobile).
- 1955 – Paul Harrington developed Harrington distraction instrument to straighten the spine and hold in place during spinal fusion operation. [7]
- 1966 - Harrington invents pedicle screws. [32]
- 1977 – George Bagby creates the “Bagby Basket”, a perforated stainless steel cylinder for stabilizing the cervical spine of horses. The operation with the cylinder yielded 20% death rate. [8]
- 1984 – Cortrel and Dubousset develop segmental instrumentation system. It used two crosslinking rods for correction. [7]
- 1992 - Prof. Jurgen harms invents Harm’s cage. [32]
- 1996 – FDA approves redesigned titanium “Bagby Basket” for human use. [8]
- 1997 – First expandable thoracolumbar corpectomy cages approved in Europe. [25, 8]
- 1998 - First expandable cervical cages approved for use in patients in Europe. [25]
- 1998-present - New materials for expandable cages (PEEK), improved mechanical stability, studies on bone cement such as PMMA.
Health Issues
Artificial vertebrae can be used to replace malfunctioning or severely damaged vertebrae. The main causes for replacement are fracturing, tumors, and degenerative diseases.
Fractures
Fracturing of the vertebral column is classified as either a burst, compression, or flexion-distraction fracture. The more common and less severe fracturing, compression fractures, are the collapse of a vertebra due to an axial load, as the vertebral column is part of the axial skeleton. [28] This can be caused by weakening of the vertebra, such as falling on the buttocks or ejection from an ejection seat of a jet fighter. As the vertebral body carries the majority of the load of the vertebra, compression fractures intuitively collapse the anterior vertebra (vertebral body) while The posterior section may remain intact depending on the energy level and severity of the load being applied. [28] The thoracic curve is the most likely region for compression fracturing to occur as it supports a great deal of the axial load. [9] In addition to being caused by traumas, compression fractures can be brought on by weakening of the vertebra due to osteoporosis. Osteoporosis is a disease that reduces bone mineral density; the cancellous bone in the vertebrae is thus weakened and more susceptible to fractures. [26]
Burst fracturing, accounting for 17% of spinal fractures, is a break from high-energy axial load causing the vertebra to shatter on impact. Burst fractures are more severe and often occur in the thoracolumbar regions. They are associated with both anterior and posterior damage and often result in kyphosis, or curving of the spine [29]. Neurological damage, occuring in 30% of cases, furthers mobility hindrance to the patient. As opposed to compression fracturing, burst fracturing damages the entire vertebral structure, not just the body. [10]
Flexion-distraction fracturing is caused from the spinal column being flexed in a way that causes one or more vertebrae to snap, in essence it is pulled apart. . This often occurs with force to the chest. As so, this type of fracturing is most common in a head-on car crash where the upper body is launched forward while the lower body is held in place by a lap seat belt. [12]
Tumors
Spinal tumors are rare but pose a great threat to the integrity of the spinal structure. These tumors often originate in other locations throughout the body and metastasize, most often lymphatically spread, to the spinal column. [6] This means that the tumors on the spinal column are often composed of abnormal cells of a different region of the body that had entered the blood stream from a primary tumor and reached the spinal column. [11] Their surgical removal often compromises the strength and function of the vertebral column. [23]
Degenerative Diseases
Degenerative diseases can be cause in itself for the need of artificial vertebrae but are often the root of a complication, such as with osteoporosis increasing the likelyhood of fracturing. There is a large variety of degenerative diseases affecting the spinal column and several are listed below with a brief description.
Spinal stenosis is a narrowing of the spinal canal by a build up of tissue. This can eventually compress nerves and the spinal cord. [13]
Osteoporosis reduces bone mineral density and deteriorates bone structure. This results in weaker bones more prone to fracturing. [14] 700,000 cases of compression fractures in the spine are due to osteoporosis alone in the United States each year. [9]
Artificial Vertebrae

The most current form of artificial vertebrae is a vertebral body replacement cage. These vertebral body replacements, almost always made of titanium, can either have non-expandable or expandable cages. [25] In the case of non-expandable cages, the cage must be produced with exact size, angular orientation and dimensions that the patient requires. Expandable cages offer advantages in that they can be inserted and expanded to the optimal size and orientation while in place that theoretically insures a tight fit and minimizes the size of the surgical opening. [15] However, they are, in most cases, considerably more expensive to produce. [25] Several studies have shown that the biomechanical stability of newly developed expandable cages is about equal to that of both non-expandable cages, as well as that of older types of vertebral body replacements, such as mesh cages, Harm’s cage, and bone grafts. [24] A study in 2004 showed that in a comparison of expandable and non-expandable cages there were no significant differences in biomechanical properties. [16] More importantly, it showed that variations in design of expandable cages (from company to company) did not have an effect in biomechanical stability, as they all employed the same basic design structure. Although results were unclear, this study seemed to find that expandable cages do increase the effect of stress shielding; this could potentially result in less favorable long term outcomes in patients with expandable cages. [25] However, there have yet to be extensive long term studies on the expandable cages. [15]
An additional study was done in 2007 using a Synex brand implant in vertebral body replacement surgery; specifically a titanium Synex telescopic expansion cage was used along with additional stabilization. [24] This study used the implant in 14 cases of an acute fracture, 4 cases of posttraumatic kyphosis, and 2 cases of skeletal disorders due to a tumor. [24] No fatalities or infections were reported, and there was no displacement or release of the implant found throughout the study. The correction of kyphosis was significant; it was found to be corrected up to 2 degrees in patients with posterior stabilization, and up to 5 degrees in patients with anterior stabilization. One exceptional case showed a correction of 10 degrees in a patient with anterior stabilization. [24] However, this study concluded that the use of these cages in cancer patients was controversial due to their high price and the shorter expected survival time frame of these patients. Synex was later forced to recall many of their expandable cage designs in 2009 after multiple cases of malfunctioning and failing vertebral body replacements. [23]
A recent study, carried out in 2011, found that expandable cages have advantages over traditional mesh implants as well as structural allografts. This study looked at single and multiple vertebrectomy in the thoracic and lumbar regions of the vertebral column due to tumors, trauma, and infection [31]. After 12 months a significant improvement was found in kyphosis, spinal alignment, and general back pain among patients. [9] A full follow up 31 months after the operations found that height restoration due to the expandable cages was on par with that found from more traditional treatments and that there were no negative effects in the form of infection or mechanical failure. [31] This study concluded that expandable intervertebral body strut grafts are a legitimate, safe treatment in human spinal surgery and vertebrectomy. [31]
While titanium is the primary cage material, Polyether-etherketone (PEEK), a hard radiolucent plastic, is gaining popularity. Radio marker dots can be used for surgeons to help guide the surgery in cage placement. It has an elasticity modulus close to that of bone, 3.6Gpa. X-ray imaging can also by used for positioning during the surgery with this material. [22]
Determination of Mechanical Behavior
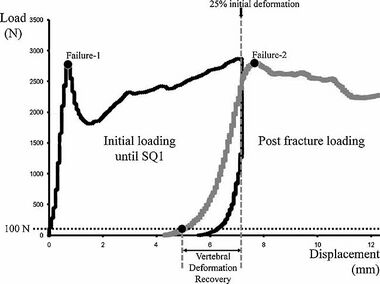
A 2011 study simulated the mechanical behavior of a vertebra pre-fracture and post-fracture. This study used only a vertebra from a cadaver to simulate a compression fracture which typically occurs with osteoporosis. The vertebrae used in testing were cut separate from any soft tissue and the test was conducted explicitly on the vertebral body. Typical pre-fracture loads were found to be averaged at 2615 N with a ± 1136 N standard deviation. Post-fracture, the failure load was found to be around 10% less, or 2285 ± 970 N. The fracture that was determined best to use was a mild fracture, listed as SQ1, which is defined as 25% deformity. After the deformity had taken place, the bone was allowed a rest time of 30 minutes before being tested under the exact same conditions to simulate post-fracture conditions. This study only recently characterized these mechanical properties of the vertebral body. When making an artificial vertebra, it would not only be important to replicate these results, but it would also be important to remember the flaws associated with an isolated study like this. [33]
One of the issues associated with load bearing studies such as the one listed in 2011 is that they isolate the specific bone without regarding the tissue or other bones around it. Muscle will help share some of the load in an actual body as well as other vertebra. Along with other vertebra, intervertebral discs will also decrease the amount of load on one individual vertebra by controlling the compression. There is also the physical makeup of the vertebrae as well. The architecture can have a large impact on how the vertebra reacts to force. Another physical characteristic to consider is the bone mineral density. Each person is different and their bone density and vertebrae shape are no exception. Along the curve of someone’s back, vertebrae change as well. Making an artificial vertebra has to take these factors into consideration and as a result can only be made to fit one specific person. [34]
Vertebrae Replacement Surgery
Artificial vertebrae provide an alternative to traditional spinal fusion. Spinal fusion is the process of fusing multiple vertebrae together in order to immobilize a vertebra that is causing pain due to abnormal motion from kyphosis. This process normally involves the use of a structural bone allograft. [29] Using a combination of an artificial vertebrae with a bone autograft decreases the risk of transmitting infectious disease that is present when using a bone allograft. [29]
The procedure begins with an incision on the left side of the upper abdomen and the spine is approached from the front for best access to the vertebral body. Fractured bone and the discs above and below the target vertebral body(ies) are removed carefully. A metal (titanium) cage filled with bone graft material is then inserted to replace the removed area. The bone graft is essential in growing bone around the cage for long term stability. Screws are then inserted with plates into the vertebral bodies adjacent to the replacement cage. A metal rod is attached on both plates for support and stabilty while the bone grows. The incision is then closed to complete the surgery. A back brace is often required in the 3-6 months of recovery time that it takes for the bone to fully grow. [21]
Vertebrael structures can be replaced with bone grafts, both autologous and allogenic, or with implants known as corpectomy cages (corpectomy is the surgical removal of a part of the vertebral body, either a whole vertebra or a part of one). [25] The most common type of bone graft used is “autologous tricortical iliac crest” bone graft. Autologous or allogenic grafts are also taken from the fibula, ribs, tibia, or femur. [25]
Insertion of artificial vertebrae is done under complete anesthesia. This implant is usually made up of a perforated cylinder and has two threaded endplates. In most cases the endplates have large spikes that help to stabilize the cylindrical implant, which has several perforations that are useful for the insertion of the bone graft. In severe cases of kyphosis the best results are often obtained using a combination of replacement artificial vertebrae and other forms of spinal fixation such as artificial intervertebral discs and various spinal plate and rod systems. [23, 30]
Issues
The biggest issue with vertebral body replacement is the potential for collapse. In such a case, the orientation and/or height of the replacement can be compromised. The failure of a single vertebra in turn may generate spinal instability which can lead to neurological damage as well as irregular spinal curvature and reduced mobility along with associated pains [23]. Other challenges include the dimensions and logistics behind full vertebral body replacements, the characterization of these properties and the individuality of each case scenario. [34]
In June 2007, the company Synthes gained rank as one of three top companies in spinal devices worldwide. This was largely due to the distribution of the Ti Synex II Central Body Replacement. Two years later, several patient reports revealing the device's tendency to collapse brought the FDA to issue a recall. On top of the recall, Synthes was also indicted on charges of illegal testing of bone cement products. The FDA gave warnings that the bone cement was highly dangerous and studies showed it sometimes caused blood clots. [23, 2]
Alternatives
Vertebral body replacement with artificial vertebrae is not the only technique addressing spinal column injuries. Prominently, there is spinal fusion, vertebroplasty/kyphoplasty and vertebral body stenting that are currently undergoing many clinical trials.
Spinal Fusion
Spinal fusion is a welding of painful vertebrae together. The source of the pain must be precisely located for this surgical procedure. The procedure fuses the vertebrae to prevent movement and thus prevent the symptoms of the issue from arising. The fusion reduces spinal flexibility, ranging from slightly to greatly depending on the extent of fusion. The spinal fusion itself requires a bone graft to stimulate bone growth. Autografts, bone grafts harvested from the patient, allograts, using cadaver bone, along with the use of several biomaterials comprise the main bone grafting options. Screws and metal rods are additionally used for initial fixation while the bone grows as in the artificial vertebrae procedure. The procedure costs in the range of $90,000.
Disadvantages of bone grafts include the chance of infection, nerve damage, blood clots, and most significantly, recurring symptoms. The fusion does not irradicate the issue but merely immobilizes the affected area and so the original symptoms in some patients have reemerged. [17]
Vertebroplasty & Kyphoplasty
In vertebroplasty, bone cement, typically PMMA(polymehtyl methacrylate), is injected into a fractured vertebra through a hole in the skin to stabilize the fracture. Kyphoplasty, a variation of vertebroplasty, injects bone cement into fractured vertebra after creating a void with a small balloon so as to correct the height and angle of kyphosis. The small balloon is inflated with fluid so as to adjust the height of the vertebrae that is causing pain. The procedures are both minimally invasive. Due to the relative gentle procedure, this is often the choice treatment for patients with compression fractures through osteoporosis or those unable or unwilling to undergo a more drastic alternative. The procedure costs in the range of $3,000 - $16,000. [18]
While a viable alternative, vertebroplasty and kyphoplasty are not for the young and healthy due to a lack of long term information with the cement. In addition, two randomized and blinded studies found no benefit for patients with osteoporosis-related fractures. [19] This caused many to stir in the industry as elderly patients with osteoporosis are also the main target for this treatment, wherein lies the potential issue. Currently, Vertebroplasty is the main subject of research in the field of artificial vertebrae. Its effectiveness, having been called into question, is under serious assessment. One study, recently concluded in 2014 is considering the possibility that bed rest might be the best thing for these patients. [35]
Vertebral Body Stenting
Vertebral body stenting is the use of a stent, or an expandable scaffold, to increase the height of the vertebrae prior to the injection of the cement. It is another form of vertebroplasty, which, is thought to be better because there is no loss of height from the deflation of the balloon in Kyphoplasty. An ongoing study is currently assessing the effectiveness of this as well. [36] Another study, published in 2013 found that there was 'no beneficial effect' of using stenting over Kyphoplasty, which may indicate that the placebo effect also occurs in this form of vertbroplasty. [37]
Future Directions
Many spinal surgeons are agreeing that the future methodology in dealing with spinal injury will focus on improving mobility, specificity, and how invasive the procedure is. As the mortality rate and complications decrease, a device yielding unimpaired mobility is necessary. Long term case studies reveal potential issues and faults with using a standard artificial vertebral replacement. This so, special replacements will arise to target niche audiences and specific ailments. Regarding the surgical procedures, the less taxing the procedure, the larger the perspective benefit. Specifically, elder patients are currently deterred frequently from surgical procedures in fear of the steep recovery and proceed with nonsurgical methods. [20]
References
- [1]”What is the Vertebral Column?” wiseGEEK. Accessed Feb. 2013<http://www.wisegeek.com/what-is-the-vertebral-column.htm>
- [2]”Vertebral Body Replacement – Synex II Complications and Side Effects.” Ceatus Media Group LLC. 2009. Feb 2013 <http://www.mediafact.com/synthes-recall/vertebral-body-replacement.html>
- [3]Joseph, Thomas N. “Skeletal Spine.” MedlinePlus, April 2012. Web. Feb 2013. <http://www.nlm.nih.gov/medlineplus/ency/imagepages/1116.htm>
- [4]”Lumbar Spine (Lower Back) Anatomy and Function.” HealthPages.org. Web. Feb 2013 <http://healthpages.org/anatomy-function/lumbar-spine-lower-back-structure-function/>
- [5]”Vertebrae of the Spine.” Cedars-Sinal, 2012. Web. Feb 2013 <http://www.cedars-sinai.edu/Patients/Programs-and-Services/Spine-Center/Anatomy-of-the-Spine/Vertebrae-of-the-Spine.aspx>
- [6]”Anatomy, The Vertebrae” The Wellington Hospital Capital Neurosurgeons, 2007. Web. Feb 2013 <http://www.thewellingtonneurosurgeryunit.com/spine-anatomy-vertebrae.asp>
- [7]”Scoliosis of the Spine.” Brown University, August 2008. Web. Feb 2013 <http://biomed.brown.edu/Courses/BI108/BI108_2008_Groups/group14/pages/history.html#C>
- [8] “Spine Stabilization With Titanium Cages.” The Burton Report. Web. Feb 2013. <http://www.burtonreport.com/infspine/SurgStabilCage.htm>
- [9] “Spinal Compression Fractures.” Orthogate, July 2006. Web. Feb 2013 <http://www.orthogate.org/patient-education/thoracic-spine/spinal-compression-fractures.html>
- [10]Rajasekaran, S. “Thoracolumbar burst fractures without neurological deficit: the role for conservative treatment.” NCBI, 2010 March; 19(Suppl 1): 40-47. Web. Feb 2013. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2899715/>
- [11] Cashin-Garbutt, A. ”Metastasis – What is Metastasis.” News Medical. Web. Feb 2013. <http://www.news-medical.net/health/Metastasis-What-is-Metastasis.aspx>
- [12]”Fractures of the Thoracic and Lumbar Spine.” OrthoInfo. American Academy of Orthopaedic Surgeons, February 20120. Web. Feb 2013. < http://orthoinfo.aaos.org/topic.cfm?topic=a00368>
- [13] “Degenerative Spine Disease.” Nervous System Diseases, 2008. Web. Feb 2013. <http://www.nervous-system-diseases.com/degenerative-spine-disease.html>
- [14]National Osteoporosis Foundation. Web. Feb 2013. <http://www.nof.org/>
- [15] Thongtrangan, I., Balabhadra, R. S. V., Le, H., Park, J., Kim, D. H. “Vertebral Body Replacement With an Expandable Cage for Reconstruction After Spinal Tumor Resection.” Neurosurg Focus. 2003; 15 (5). Web. Feb 2013. <http://www.medscape.com/viewarticle/465370>
- [16]Pflugmacher, R., Schleicher, P., Schaefer, J., Scholz, M., Ludwig, K., Khodadadyan-Klostermann, C., Haas, N. P., Kandziora, F. “Biomechanical comparison of expandable cages for vertebral body replacement in the thoracolumbar spine.” Spine 2004 July 1;29(13):1413-9 <http://www.ncbi.nlm.nih.gov/pubmed/15223931>
- [17] “Spinal Fusion.” OrthoInfo. American Academy of Orthopaedic Surgeons, 2010. Web. Feb 2013 <http://orthoinfo.aaos.org/topic.cfm?topic=a00348>
- [18] “Vertebroplasty & Kyphoplasty.” RadiologyInfo.org, Radiological Society of North America. Web. Feb 2013. <http://www.radiologyinfo.org/en/info.cfm?pg=vertebro>
- [19]Johnson, J; Rogers, W; Jeffree, RL (2012 Aug). "The controversy over vertebroplasty: an analysis of the debate and proposals for a way forward.". Journal of medical imaging and radiation oncology 56 (4): 449–51.
- [20] “8 Spine Surgeons on the Future of Spinal Fusions.” Spine Review, 2012. Web. Feb 2013 <http://beckersspine.com/spine/item/11899-8-spine-surgeons-on-the-future-of-spinal-fusions>
- [21] http://content.understand.com/Players/Flash/?accountid=f04f261e-d566-4c64-9e9c-a9ffbade9a24&presentationid=82760be2-c0e4-4669-8b47-42db548566a0&languageid=6574fa28-0a40-49af-88c8-3ce366c8c580
- [22] <http://www.medcompare.com/spotlight.asp?spotlightid=128>
- [23] http://www.mediafact.com/synthes-recall/synex-side-effects.html
- [24] Zeman J, Matĕjka J, Belatka J, Vodicka J. [Vertebral body replacement with a
Synex implant]. Rozhl Chir. 2007 May;86(5):263-7. Czech. PubMed PMID: 17634016.
- [25] F. Kandziora, K. J. Schnake, C. K. Klostermann and N. P. Haas. Vertebral body replacement in spine surgery. DER UNFALLCHIRURG
Volume 107, Number 5, 354-371, DOI: 10.1007/s00113-004-0777-z
- [26] David W. L. Hukins and Judith R. Meakin. Relationship Between Structure and Mechanical Function of the Tissues of the Intervertebral Joint. Amer. Zool, (2000) 40(1): doi: 10.1093/icb/40.1.42
- [27] http://www.dartmouth.edu/~humananatomy/part_7/chapter_39.html
- [28] http://www.ipublishing.co.in/jcandsevol1no12010/EIJCSE1001.pdf
- [29] Glenn R. Buttermann, Andrew L. Freeman, Brian P. Beaubien, In vitro biomechanics of an expandable vertebral body replacement with self-adjusting end plates, The Spine Journal, Volume 10, Issue 11, November 2010, Pages 1024-1031, ISSN 1529-9430, 10.1016/j.spinee.2010.08.017.
(http://www.sciencedirect.com/science/article/pii/S1529943010011125)
- [30] http://www.stryker.com/en-us/products/Spine/InterbodyVertebralBodyReplacement/RTF-PLIFmplant/index.htm
- [31] Keshavarzi S, Newman CB, Ciacci JD, Aryan HE. Expandable titanium cages for
thoracolumbar vertebral body replacement: initial clinical experience and review of the literature. Am J Orthop (Belle Mead NJ). 2011 Mar;40(3):E35-9. PubMed PMID: 21720606.
- [32] DePuy Spine. “Spine Fundamentals: Surgical Solutions for Spine Pathologies.” Powerpoint.ceuinstitute.net/presentations/History%20of%20DePuy%20Spine%20and%20Spine%20Surgery%20SBS%20NEW%20101006.ppt
- [33] Wegrzyn, Julien, Jean-Paul Roux, Monique E. Arlot, Stéphanie Boutroy, Nicolas Vilayphiou, Olivier Guyen, Pierre D. Delmas, Roland Chapurlat, and Mary L. Bouxsein. "Determinants of the Mechanical Behavior of Human Lumbar Vertebrae After Simulated Mild Fracture." Journal of Bone and Mineral Research. Wiley Subscription Services, Inc., A Wiley Company, 6 Oct. 2010. Web. 22 Feb. 2016.
- [34] Briggs, Andrew M., Alison M. Greig, John D. Wark, Nicola L. Fazzalari, and Kim L. Bennell. "A Review of Anatomical and Mechanical Factors Affecting Vertebral Body Integrity." International Journal of Medical Sciences. Ivyspring International Publisher, 12 Oct. 2004. Web. 22 Feb. 2016.
- [35] "Comparison of Balloon Kyphoplasty, Vertebroplasty and Conservative Management in Acute Osteoporotic Vertebral Fractures (OSTEO-6)." Comparison of Balloon Kyphoplasty, Vertebroplasty and Conservative Management in Acute Osteoporotic Vertebral Fractures. ClincalTrials.gov, 13 Dec. 2014. Web. 22 Feb. 2016.
- [36] "Study on the Treatment of Osteoporotic Vertebral Fractures Using Vertebral Body Stenting." Study on the Treatment of Osteoporotic Vertebral Fractures Using Vertebral Body Stenting. ClincalTrials.gov, 24 Sept. 2015. Web. 22 Feb. 2016.
- [37] Werner, CM, G. Osterhoff, J. Schlickeiser, R. Jenni, GA Werner, C. Ossendorf, and HP Simmen. "Vertebral Body Stenting versus Kyphoplasty for the Treatment of Osteoporotic Vertebral Compression Fractures: A Randomized Trial." US National Library of Medicine and Nation Institutes of Health. Pubmed.gov, 3 Apr. 2013. Web. 22 Feb. 2016.
Images
- [A] U.S. National Library of Medicine. NIH Medicine Plus, n.d. Web. 22 Feb. 2016. [1]
- [B] Wellington Hospital. HCA Healthcare UK, n.d. Web. 22 Feb. 2016. [2]
- [C] Columbia University Medical Center. Columbia University, n.d. Web. 22 Feb. 2016. [3]
- [D] "Musculoskeletal System and Artificial Replacements." Development and Structural Analysis of a Vertebral Body Replacement. Laborator Biomechaniky Cloveka, n.d. Web. 22 Feb. 2016. [4]
- [E] Wegrzyn, Julien, Jean-Paul Roux, Monique E. Arlot, Stéphanie Boutroy, Nicolas Vilayphiou, Olivier Guyen, Pierre D. Delmas, Roland Chapurlat, and Mary L. Bouxsein. "Determinants of the Mechanical Behavior of Human Lumbar Vertebrae After Simulated Mild Fracture." Journal of Bone and Mineral Research. Wiley Subscription Services, Inc., A Wiley Company, 6 Oct. 2010. Web. 22 Feb. 2016.
