Artificial Skin, by Katie Geldart
Introduction

The term artificial skin is used to describe any material used to replace (permanently or temporarily) or to mimic the dermal and epidermal layers of the skin. The primary current application of artificial skin is for the treatment of skin loss or damage on burn patients. Alternatively however, artificial skin is now being used in some places to treat patients with skin diseases, such as diabetic foot ulcers, and severe scarring [1]. Labs have also developed in vitro skin samples for the use of cosmetic and medical testing. This provides a cheaper and more ethical approach for testing surface reactions to topical treatments [1].
The most important goals of current artificial skin technologies are to provide protection from infection, dehydration, and protein loss after severe skin loss or damage. Each year, over 2 million people in the United States are treated for burns [2]. Advances in artificial skin and skin grafting techniques have drastically improved the chances of survival for burn patients [2]. Infection and dehydration are two of the most dangerous conditions imposed by skin loss. After an accident, irreparably damaged skin layers must be removed to prevent bacterial growth. Artificial skin materials allow the area to be sealed quickly to prevent fluid loss and bacteria from entering through the wound. Integra is a brand of artificial skin commonly used in medical facilities today.
Anatomical Overview of Skin
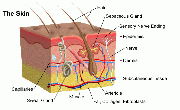
Human skin is comprised of two primary layers, the dermis and the epidermis. A diagram of a typical section of human skin is shown here. The epidermis is comprised of keratinocytes of varying levels of differentiation. As can be seen in the figure, the epidermis contains no blood vessels meaning transport of nutrients to the epidermis occurs from the dermis below [2]. While the primary role of the epidermis is to provide an outer protective layer, the dermis contains several structures important to skin function. Hair follicles, sweat and oil glands, and nerves are all found within the dermis [2]. Additionally, epithelial keratinocytes originate from within this layer. Because of these supporting roles, depth of damage to the dermis is a determining factor in the skin’s ability to heal. Current artificial skin techniques for burn treatment typically provide a scaffolding to promote regeneration of the dermis. An autograft is then performed to replace the epidermis. Alternatively, artificial skin has been made to replace both layers of the skin as in the case of certain small wound and foot ulcer treatments. This will be discussed further in the “Current Medical Procedures” section.
Developmental History of Artificial Skin
3000-2500BC, India: Skin is allegedly transplanted by Hindus from the buttocks to repair mutilated ears and noses.
1442, Italy: An allogenous skin graft was performed by Branca de Branca who used a man’s arm skin to transplant the nose of the man’s slave onto himself.
1597, Italy: Branca’s methods were published by Tagliacozzi.
1804, Italy: First successful autograph in sheep, done by Baronio.
1823, Germany: Full thickness autologous skin grafts were successfully performed by Bunger. Done by transplanting skin from the patient’s thigh to their nose, a procedure inspired by the original Indian records.
1869, Switzerland: First epidermic pinch graft by Reverdin.
1871, England: Pollock proposes skin grafts for burn treatment.
1875, Scotland: Full-thickness skin grafts become an official clinical practice.
1886, Germany: Thin split-thickness skin grafts used by Thierch.
1970’s, United States: Cryopreserved skin used for human allografts, viable epithelial sheets grown in vitro by Rheinwalk and Green.
1979, United States: Burke and Yannas successfully test the first artificial skin (Integra) on a patient [1].
1981, United States: Cultured epithelial grafts used in burn patients.
1998, United States: First tissue engineered skin (Apligraf) is approved by the FDA.
2001, United States: Dermagraft, Orcel, Composite Cultured Skin are FDA approved [4].
2002, United States: Integra is FDA approved for treatment of severe burns [4].
- All time points provided by reference [3]unless otherwise noted
Current Treatment Options
Skin Grafts
Skin grafts are required for patients with skin damage that is too significant for self-repair. As stated before, one of the primary requirements for artificial skin is for the treatment of severe burn victims. There are three levels of burns; 1st, 2nd, and 3rd degree burns. A first degree burn only affects the epidermis whereas a second degree burn extends downward into the dermis. Third degree burns go through the epidermis, dermis, and the hypodermis. A “severe burn” is classified as either a 2nd covering over 10% of the body or 3rd degree burn covering over 1% of the body [2]. In either of these scenarios a skin graft will most likely be required for the area to heal. Skin grafts are also often done on patients with ulcers, skin loss from cancer removal, and plastic surgery [1].
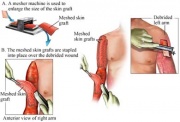
The skin required for a skin graft can be obtained from three sources; the patient themselves (autograft), another human (allograft), or from animals such as pigs or cows (xenografts)[2]. Allografts and xenografts can only be used as temporary wound coverings as they are typically rejected within 7 to 10 days or 3 to 5 days respectively [2]. There are two primary types of autografts; split-thickness grafts and full-thickness grafts. Split thickness grafts take only a part of the dermis and the epidermis from the donor site to transplant to the wound site. This is beneficial in that the donor site remains somewhat intact however, because the transplanted tissue does not contain all of the original glands and hair follicles, split-thickness grafts typically leave noticeable differences in skin color and texture. Full–thickness skin grafts take out the entire dermis and epidermis layers from the donor site but they look more natural in the wound site and often provide improved skin flexibility compared to the STSG. For this reason, FTSG are commonly used for hand and facial skin graft procedures. There are several draw backs to autographs, the first of which is the removal of donor skin from another part of the body. Needless to say, both STSG and FTSG procedures leave scarring in both the donor and wound sites. Additionally, when skin is removed from one area to place in another, both areas must be given treatment to allow proper healing. Even more concerning however is the lack of availability of these donor skin sites for patients suffering from extremely large areas of skin loss. This is where artificial skin has truly made a difference.
Artificial Skin Treatments

Since 2001, a total of 4 skin repair devices have been FDA approved. These include Dermagraf, Orcel, Integra, and Composite Cultured Skin [4]. Dermagraft and Apligraf (FDA approved 1998) are used for the treatment of foot ulcers and contain living cells. Orcel is used to cover and aid in wound progression, specifically in donor sites on burn patients. Composite Cultured Skin is specifically for children with recessive dystrophic epidermolysis bullosa and also contain living cells. Integra is the only one of these treatments currently FDA approved for treatment of severe burn areas. Integra is comprised of shark cartilage and bovine collagen [4].
In the most common procedures using artificial skin for skin repair patients, the damaged dermis is removed and a layer of artificial skin is placed over the wound. When using Integra, the collagen matrix provides a scaffold onto which dermal cells begin to grow. Once blood vessels sufficiently vascularize the neo-dermis, the layer of silicon covering the matrix is removed and autologous epidermal cells are spread over the neo-dermis. Glycosaminoglycan within the matrix signals for cells to begin producing their own collagen and over time, a natural ECM replaces the artificial layer [2]. Orcel is actually a biolayered cellular matrix that contains both dermal and epidermal cells. This means that if the cells are able to vascularize and take to the area, only one surgical treatment is required. The cells within Dermagraf, Apligraf, and Orcel aid in speeding up the healing process by secreting growth factors and proteins native to skin tissue. This promotes regeneration of skin in the wound.
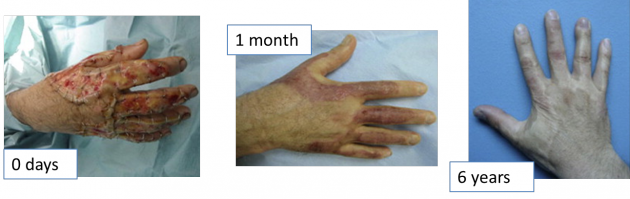
Complications and Risks
Infection and immunological rejection are the two of the most common and detrimental risks involved in skin repair therapies. Lack of vascularization to the implanted skin or skin cells can lead to cell death which provides a breeding ground for bacteria. This would especially be problematic in procedures using either full-thickness skin grafts or bilayered cellular matrices as portions of these tissues remain longer without blood supply. For severe burn patients who do not have enough skin remaining for autografts, allografts are often the only choice for a source of epidermal skin. In these cases immunological rejection is extremely common. In addition to infection and rejection, fluid buildup between the wound site and the transplanted skin can prevent the skin from “taking”. If this occurs, the procedure must be repeated. Skin adhesion is also a problem when using Integra if the epidermis does not fuse correctly to the neo-dermis.
Ongoing Research
While artificial skin has aided significantly in skin regeneration, there remain several areas for improvement. Currently, a minimum of two surgical treatments are required for severe burn patients using artificial skin. Matriderm is an upcoming treatment for burn victims similar to Integra. Unlike Integra however, the dermis matrix and epidermis cells are able to be put in place in one surgical session [5]. Research is now also being done to attempt to produce bacteria-resistant skin cell cultures that can be used in artificial tissue. Ideally, this would allow in vitro replication of a patient’s own genetically modified skin cells. These cells could them be put into the artificial matrix for bacteria-free growth [6]. Other advances have developed in the application of the cells to the matrices. Dr. Fiona Woods has produced a “spray on skin” called Cellspray [7]. This method takes healthy cells from the patient and creates a suspension culture of the cells. The cells are then distributed by spraying them evenly across the matrix. It is believed that this method will be beneficial because the suspension cell culture can be produced much faster (5 days) than traditional methods which require formation of a sheet of cells (21 days). Though this procedure has not been through clinical trials, it was controversially used on burn victims in conjunction with traditional methods in the Bali bombings in 2004 [7]. Further testing is required before this treatment can officially be deemed successful.

Outside of artificial biological skin, synthetic skin is being developed in hopes of enabling the sensation of touch to non-living structures. Flexible pressure transducers may eventually allow us to create an electronic “skin” with signals to mimic the sense of touch. This has applications in robotics including advanced prosthetic limbs [8].
References
[1] Dantzer, E., Queruel, P., Salinier, L., Palmier, B., & Quinot, J. F. (2001). Integra, a new surgical alternative for the treatment of massive burns. Clinical evaluation of acute and reconstructive surgery: 39 case. Annales De Chirurgie Plastique Esthétique, 46(3), 173-189. http://www.ncbi.nlm.nih.gov/pubmed/11447623
[2] Roos, D. (2012). Skin grafts. Retrieved 02/29, 2012, from http://health.howstuffworks.com/skin-care/information/anatomy/skin-graft.htm
[3] Heman, A. R. (2002). The history of skin grafts. Retrieved 02/29, 2012, from http://findarticles.com/p/articles/mi_m0PDG/is_3_1/ai_110220336/
[4] Recently approved devices. (2009). Retrieved 02/29, 2012, from http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/DeviceApprovalsandClearances/Recently-ApprovedDevices/ucm083520.htm
[5] Haslik, W., Kamolz, L. -., Nathschläger, G., Andel, H., Meissl, G., & Frey, M. (2007). First experiences with the collagen-elastin matrix matriderm® as a dermal substitute in severe burn injuries of the hand. Burns, 33(3), 364-368. http://www.sciencedirect.com/science/article/pii/S0305417906002282
[6] Singer, E. (2007). A better artificial skin. Retrieved 02/29, 2012, from http://www.technologyreview.com/biotech/18059/
[7] Spray on skin. Retrieved 03/01, 2012, from http://www.biotechnology-innovation.com.au/index.html
[8] Boldand, J. J. (2010). Flexible electronics: Within touch of artificial skin. Retrieved 02/29, 2012, from http://www.nature.com/nmat/journal/vaop/ncurrent/full/nmat2861.html
Images
[A] Edmonds, M. How lab-grown skin works. Retrieved 02/29, 2012, from http://science.howstuffworks.com/innovation/everyday-innovations/lab-grown-skin2.htm
[B] Lesson on skin textures. (2010). Retrieved 02/29, 2012, from http://mydelicateskin.com/skin-care/lesson-on-skin-textures
[C] Zeltzer, R. (2009). Skin grafts. Retrieved 02/29, 2012, from http://www.lifescript.com/health/a-z/treatments_a-z/procedures/s/skin_graft.aspx
[D] Apligraf. (1999). Retrieved 02/29, 2012, from http://apligraf.com/patient/what_is_apligraf/how_is_apligraf_applied.html
[E] Cuadra, A., Correa, G., Roa, R., Piñeros, J. L., Norambuena, H., Searle, S., et al. (2012). Functional results of burned hands treated with integra®. Journal of Plastic, Reconstructive & Aesthetic Surgery, 65(2), 228-234.
[F] Boldand, J. J. (2010). Flexible electronics: Within touch of artificial skin. Retrieved 02/29, 2012, from http://www.nature.com/nmat/journal/vaop/ncurrent/full/nmat2861.html
