Artificial Bladder by David Raimondi
Artificial Bladder Background
Definition and Function
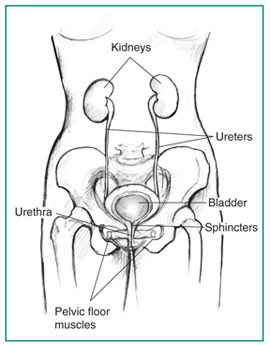
The bladder is situated in the pelvis and is part of the urinary tract. The urinary tract also includes two kidneys, two ureters, and the urethra. It is responsible for removing wastes from the body. After the kidneys filter out the wastes from the blood to make urine, the urine flows to the bladder through the ureters.[1] The bladder stores the urine to allow for voluntary and infrequent urination. It is able to do this because it is lined with muscles in the bladder wall called the detrusor muscle. It also has sphincters (which are circular muscles) at the connection between the bladder and urethra, which keep the urine retained in the bladder. There is one internal sphincter that the body opens and shuts automatically without thinking about it (a.k.a. autonomically).[2] There is also the external sphincter that is controlled by the pudendal nerve from the voluntary nervous system.[2] The detrusor muscle coordinates with the sphincters to control urination.[1] The detrusor muscle relaxes as the bladder fills up with urine. If the bladder is in good health it can hold up to 2 cups (a.k.a. 16 ounces or about 500 mL) of urine comfortably for about 2 to 5 hours.[1] When the bladder is stretched, this signals the parasympathetic nervous system to want to contract the detrusor muscle.[2] To urinate, the brain simultaneously signals the detrusor muscle to tighten and the sphincters to relax.[1] This causes urine to exit the bladder through the urethra normally.
Bladder Diseases that May Cause Bladder Surgery/Replacement
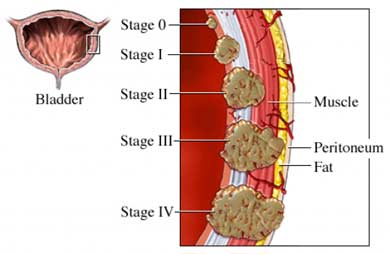
There are a few different diseases that can seriously affect the bladder to the point where it needs to be replaced. Interstitial Cystitis (a.k.a. Pain Bladder Syndrome) is one of these diseases. It is a condition that has symptoms of frequent discomfort or pain in the bladder and surrounding pelvic region. Often another symptom is an urgent and frequent need to urinate. This disease varies widely in symptoms and severity of symptoms, and it includes all cases of urinary pain that can’t be attributed to other causes (such as infection or urinary stones).[3] The cause of this disease is unknown.[3]
Another disease that can become a serious problem is bladder infection. Both serious and/or recurring infections could be a cause for bladder surgery/replacement. This disease has symptoms similar to Pain Bladder Syndrome, but they are caused by bacterial infection. This disease is generally harmless if treated with antibiotics right away. The majority of urinary tract infections are caused by strains of uropathogenic E. coli that encode “filamentous adhesive organelles called Type 1 pili."[4] These organelle structures mediate bacterial attachment and invasion of bladder epithelial cells using a surface adhesion molecule called FimH. This surface molecule binds to receptors on the bladder epithelial cells.[5]
Bladder cancer is another one of the more likely reasons to need a bladder replacement. Symptoms of bladder cancer include blood in the urine (a.k.a. hematuria), pain during urination, frequent urination, feeling the need to urinate often in the night, possible unexplained appetite loss and/or weight loss.[7]
Motivation and Statistics
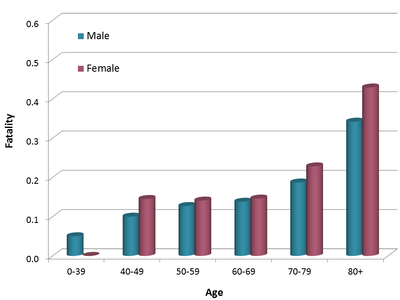
There is a need for artificial bladders because of the prevalence of these diseases. While not all of the cases of each disease require a full bladder replacement, there is still a good amount that could benefit from one. This is especially true because the common type of E. coli bacteria that causes bladder infection seems to be increasingly resistant to one of the common antibiotics.
- About 3.3 million U.S. women (2.7%) who are 18 years of age or older have pelvic pain and other symptoms, such as urinary urgency or frequency, that are associated with Interstitial Cystitis/Pain Bladder Syndrome.[3] About 1.6 million U.S. men (1.3%) who are 30 to 79 years old have persistent symptoms, such as pain with bladder filling or pain relieved by bladder emptying, that are associated with Interstitial Cystitis/Pain Bladder Syndrome.[3]
- Bladder infection is more prevalent in women. About 11% of women in the U.S. report having one physician-diagnosed Urinary Tract Infection (UTI) per year.[6] The lifetime probability that a woman will have a UTI is about 60%.[6] The management of this common condition is becoming more difficult due to increasing prevalence of E. Coli that are resistant to antibacterial agents. Recent studies show about 15-18% of E. Coli from UTI in women were resistant to trimethoprim-sulfamethoxazole, which is a common antibacterial treatment for UTI. [6]
- Bladder cancer has the ninth most prevalent malignancy of cancers. In 2008, there were an estimated 386,000 new cases of bladder cancer worldwide, with bladder cancer causing approximately 150,000 deaths.[8] In the United States, almost 75,000 new cases and 16,000 deaths occur each year due to bladder cancer.[9] This is one of the more serious conditions that need bladder replacements.
History of Artificial Bladders
- 1960: Research into artificial bladders began. [10]
- 1996: Artificial scaffold was created by Dr. Atala to represent bladder and was seeded internally with urothelial cells and externally with muscle cells.
- 1998: Utilizing new ideas, a German research team beings work on fully implantable alloplastic bladder that is still in progress. It is made of semi-rigid outer material and has a central control system. The system monitors the urine fill level and alarms the patient via remote control when it has to be emptied. Then, the patient can empty the bladder by activating the pump.[10]
- 1998: Dr. Atala's lab-grown bladder was successfully transplanted into dogs. After 11 months the bladders were still fully functional. [11]
- 1999: Seven patients between ages 4 and 19 had artificial bladders grown from their own cells implanted. [12]
- 2003: Patent for the artificial bladder process was licensed to Tengion. [12]
- 2006: The continued follow up and results of the patients from the 1999 study were published. Results were overall positive. This was cause for celebration because the positive results meant these were overall successful artificial bladder implantations. [12]
- 2010: Phase I clinical trials of the 'Neo-Urinary Conduit' made by Tengion began. [13]
- 2013: Seventh patient receives Phase I clinical trial of the 'Neo-Urinary Conduit.' [13]
Alternatives to Artificial Bladders
There are several alternatives to completely replacing the bladder with an artificial bladder of some sort. First, it is important to note that there are three main different kinds of bladder surgery. These different kinds are:
- Transurethral Resection - The least invasive surgery (no incisions). It is primarily performed for bladder cancer treatments. A resectoscope gets to the bladder through the urethra and a small, electrified loop of wire attached to the resectoscope is used to cut tumor and remove the tissue.[14]
- Partial Cystectomy - Relatively uncommon because it is only used to remove easily accessible and small tumors in the muscle of the bladder wall. This is hard to know that the tumor is only in the wall muscle and won't damage anything else.[14]
- Radical Cystectomy - This is the complete removal of the bladder. This is the type of procedure that is being treated by the production of artificial bladders.[14]
When a radical cystectomy is performed, the ideal situation is that there is something that will replace it that will perform the exact same function. This is why work is being done on producing an effective artificial bladder. Since artificial replacements are still rather rare there are other surgical alternatives that can be performed:
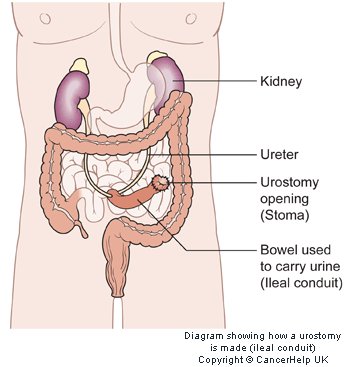
- Ileal Conduit - A small piece of bowel (ileum) is removed. The ureters are attached to one end of that piece of bowel and they attach the other end to a small hole that the surgeon cuts in the surface of the abdomen. This makes a stoma. A plastic ostomy bag is placed over the stoma and collects the urine that is expelled from the body in the bag. The bag can be emptied as often as the patient goes to the bathroom.[14]
- Continent Cutaneous Pouch - Similar to ileal conduit, but the patient does not have to wear a bag. A piece of the bowel is made into a pouch inside the body and is connected to the ureters. The pouch has an opening out of the body through a stoma in the abdomen (like the ileal conduit). Since the pouch to collect urine is inside the body the patient needs to insert a catheter into the stoma and drain the urine at least 4-5 times per day. This is subject to infection due to incomplete draining.[14]
- Neobladder - Again uses a small piece of bowel. But, it is made into a sphere and physically replaces the bladder and connects to the ureters and urethra in the same way. This allows for relatively normal urinary function. This is subject to leakage.[14]
One problem that is common between each of the three surgeries listed directly above is due to the fact that a part of the bowel is used in some way to simulate bladder function. The problem is that bowel is designed to absorb nutrients, so patients who have procedures like these can have problems with re-absorption of toxins and other health concerns. Problems with the bowel can also occur because part of it undergoes a surgical procedure.
Dr. Tony Atala's Process to Create an Artificial Bladder
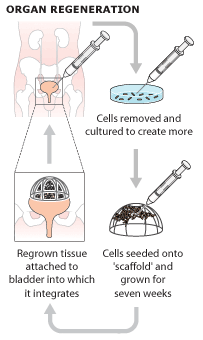
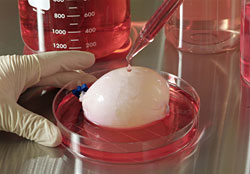
Several tests, such as, a urodynamic study and a bladder biopsy, are first performed. A CT scan of the patient helps determine the size and shape bladder to help in the formation of an effective scaffold.[12] A tissue sample from the patient's bladder has both primarily urothelial and muscle cells, which will both be used to seed the bladder scaffold. The urothelial and muscle cells are grown over a period of 7 to 8 weeks in their own respective conditions that help proliferate each type of cell the best. About 70 plates of each cell type (with 10,000,000 cells per plate) are created in this time and are used to make the artificial bladder.[12]
A biodegradable scaffold is created in the shape of the bladder that will be implanted into the patient. The scaffold is composed primarily of a mixture of collagen and polyglycolic acid (PGA).[12] As stated, the scaffolds are made to the estimated size that was determined by the CT scan. The muscle cells are seeded on the outside first at a concentration of 50,000,000 cells per cm^3 for 48 hours.[12] Then, the urothelial cells are seeded on the inside at the same concentration of cells.[12] It is kept in an incubator at 37 degrees Celsius for 3 or 4 days until the transplantation.[12] The artificial bladder is then ready to be implanted.
These artificial bladder constructs were implanted into seven patients between 4 and 19 years old for a study that commenced in 1999. All of the patients who had this artificial bladder construct from that study had improved function and good results.[12] They were examined using several different kinds of tests up to about 5 years after the artificial bladder was implanted in 1999. Normal function returned and stayed that way over the 5 years that they were being monitored. Biopsies were also taken after 31 months after implantation and showed that all of the artificial bladders had a tri-layer structure of cells like a normal bladder.[12] Also, since the patient's own cells were used, there was no real risk of rejection. Normal renal function was also maintained, which is sometimes a problem.
Future of Artificial Bladders

The future will probably be 3-D printed bladders with all the correct cell types. Although Dr. Atala says that "successful 3-D printing of organs is probably (at least) several years away." 3-D printing cells to produce organs is quite complex. In terms of engineering different tissues, Dr. Atala breaks the different tissues into basically 4 stages of complexity:
- Flat structures - Simplest to engineer. Basically made of one type of cells. Skin is an example.
- Tube Structures - Have at least 2 types of cells and act as a conduit. Blood vessels and urethras are examples.
- Hollow non-tubular organs - Have more complex structures and functions. Bladder and the stomach are examples.
- Solid organs - Most complex to engineer because they have a lot of different functions and cells types, and they also require a blood supply. The kidney, heart, and liver are examples.[15]
There are two great video links about Tony Atala and his work listed here with more information.
- A Time Magazine Piece: An Inkjet Made My Bladder!
- Dr. Tony Atala TED Talk: Printing a Human Kidney by Anthony Atala
The Neo-Urinary Conduit (from Tengion) is currently in Phase 1 clinical trials. It would be used similarly to how a part of the bowel is used in an ileal conduit procedure as seen above. It differs from that procedure because the Neo-Urinary Conduit is a physiologically functional tissue with a three-dimensional structure that uses the patient's own cells to create the structure.[16] It has been designed to replace the usage of bowel tissue. This procedure is simpler and cheaper than replacing the old bladder with an entirely new artificial bladder because the urine would just exit the body and go into a plastic bag.
- Excellent video from Tengion Website to show this kind of procedure: Neo-Urinary Conduit Surgery
Funding
In early 2014, the Institute for Regenerative Medicine at Wake Forest University School of Medicine, led by Dr. Tony Atala, has been chosen to be the primary group to lead a $75 million project that was funded by the U.S. Defense Department. This funding is to progress with the second phase of the Armed Forces Institute of Regenerative Medicine.[22]
The U.S. Defense Department funding contract is a five-year, $75 million federally funded project that focuses on applying regenerative medicine to injuries suffered on the battlefield. Wake Forest specifically will end up receiving $20 million out of the $75 million.[22] The Wake Forest Institute for Regenerative Medicine will lead more than 30 research institutions in this project. The 30 research groups will work on over 14 projects including "restoring function to severely traumatized limbs, reconstruction for facial and skull injuries through tissue regeneration, skin regeneration for burn injuries, and reconstruction of the genital and urinary organs, and lower abdomen."[22]
References
<biblio>
- 1 Urodynamic Testing. National Kidney and Urologic Diseases Information Clearinghouse. Jan 2012. NIH Publication No. 12-5106. 2 Apr 2014. <http://kidney.niddk.nih.gov/kudiseases/pubs/urodynamic/>.
- 2 Oluwaseun, Huthman, Adesanya Adewale, Soyebo Olusegun, Musa Adesina and Others. "Effects of Methanolic Extracts of Trichosanthes Cucumerina Seeds on the Weight of Urinary Bladder in Adult Male Wistar Rats." (2012): Print.
- 3 Interstitial Cystitis/Painful Bladder Syndrome. National Kidney and Urologic Diseases Information Clearinghouse. Sept 2011. NIH Publication No. 11-3220. 2 Apr 2014. <http://kidney.niddk.nih.gov/kudiseases/pubs/interstitialcystitis/>.
- 4 Mulvey, Matthew A, Joel D Schilling and Scott J Hultgren. "Establishment of a persistent Escherichia coli reservoir during the acute phase of a bladder infection." Infection and immunity, 69. 7 (2001): 4572--4579. Print.
- 5 Jones, C Hal, Jerome S Pinkner, Robyn Roth, John Heuser, Andy V Nicholes, Soman N Abraham and Scott J Hultgren. "FimH adhesin of type 1 pili is assembled into a fibrillar tip structure in the Enterobacteriaceae." Proceedings of the National Academy of Sciences, 92. 6 (1995): 2081--2085. Print.
- 6 Manges, Amee R, James R Johnson, Betsy Foxman, Timothy T O'bryan, Kathleen E Fullerton and Lee W Riley. "Widespread distribution of urinary tract infections caused by a multidrug-resistant Escherichia coli clonal group." New England Journal of Medicine, 345. 14 (2001): 1007--1013. Print.
- 7 "Bladder Cancer." Cancer.Net, 2014. Web. 2 Apr 2014. <http://www.cancer.net/cancer-types/bladder-cancer/symptoms-and-signs>.
- 8 Jemal, Ahmedin, Freddie Bray, Melissa M Center, Jacques Ferlay, Elizabeth Ward and David Forman. "Global cancer statistics." CA: a cancer journal for clinicians, 61. 2 (2011): 69--90. Print.
- 9 Siegel R, Ma J, Zou Z, Jemal A. "Cancer statistics." CA: a Cancer Journal for Clinicians, 64. 9 (2014). Print.
- 10 Roth, Matthias, H Wassermann and D Jocham. "Fully implantable alloplastic urinary bladder." (2009): 2220--2222. Print.
- 11 Oberpenning, Frank, Jun Meng, James J Yoo and Anthony Atala. "De novo reconstitution of a functional mammalian urinary bladder by tissue engineering." Nature biotechnology, 17. 2 (1999): 149--155. Print.
- 12 Atala, Anthony, Stuart B Bauer, Shay Soker, James J Yoo and Alan B Retik. "Tissue-engineered autologous bladders for patients needing cystoplasty." The lancet, 367. 9518 (2006): 1241--1246. Print.
- 13 "Tengion : Regenerative Medicine Brought to Life : Investor Relations : Press Release." Phx.corporate-ir.net, 2014. Web. 2 Apr 2014. <http://phx.corporate-ir.net/phoenix.zhtml?c=218965&p=irol-newsArticle&ID=1797085&highlight=>.
- 14 "Treating Bladder Cancer - Bladder Cancer Advocacy Network - BCAN." Bladder Cancer Advocacy Network - BCAN, 2012. Web. 3 Apr 2014. <http://www.bcan.org/learn/treating-bladder-cancer/>.
- 15 "Futurium - European Commission." Ec.europa.eu, 2014. Web. 3 Apr 2014. <http://ec.europa.eu/digital-agenda/futurium/en/content/advances-bio-artificial-and-3d-printed-organs>.
- 16 "Tengion : Regenerative Medicine Brought to Life." Tengion.com, 2014. Web. 3 Apr 2014. <http://www.tengion.com/pipeline/bladders.cfm>.
- 17 "Bladder Cancer — UVA Health." Uvahealth.com, 2014. Web. 3 Apr 2014. <http://uvahealth.com/services/cancer-center/conditions-treatments/12015>.
- 18 "Bladder cancer fatality by sex and age | Medinfographics.com." Medinfographics.com, 2014. Web. 3 Apr 2014. <http://www.medinfographics.com/cancer-statistics/bladder-cancer/bladder-cancer-fatality-by-sex-and-age/>.
- 19 "Types of surgery for invasive bladder cancer : Cancer Research UK : CancerHelp UK." Cancerresearchuk.org, 2014. Web. 3 Apr 2014. <http://www.cancerresearchuk.org/cancer-help/type/bladder-cancer/treatment/invasive/surgery/types-of-surgery-for-invasive-bladder-cancer>.
- 20 "The Top 13 Medicine Stories of 2006 | DiscoverMagazine.com." Discover Magazine, 2014. Web. 3 Apr 2014. <http://discovermagazine.com/2007/jan/medicine#.Uytm2fldUrU>.
- 21 "Top 50 Most Influential People of the 21st Century." Ranker, 2014. Web. 3 Apr 2014. <http://www.ranker.com/list/top-50-most-influential-people-of-the-21st-century/theomanlenz>.
- 22 "Wake Forest chosen for $75 million regenerative medicine project." News-Record.com, 2014. Web. 3 Apr 2014. <http://www.news-record.com/news/article_4545c3e6-2787-11e3-aff9-001a4bcf6878.html?mode=jqm>.
