BME103:T930 Group 3: Difference between revisions
| Line 168: | Line 168: | ||
GGAAGTGGGTCCTAAAAACTCTTACA['''''C''''']TGCATACATAGAAGATCACAGTGGC<br><br> | GGAAGTGGGTCCTAAAAACTCTTACA['''''C''''']TGCATACATAGAAGATCACAGTGGC<br><br> | ||
Mutated Code: (due to SNP (or mutation))<br> | |||
GGAAGTGGGTCCTAAAAACTCTTACA['''''T''''']TGCATACATAGAAGATCACAGTGGC<br><br> | GGAAGTGGGTCCTAAAAACTCTTACA['''''T''''']TGCATACATAGAAGATCACAGTGGC<br><br> | ||
Revision as of 03:18, 15 November 2012
| Home People Lab Write-Up 1 Lab Write-Up 2 Lab Write-Up 3 Course Logistics For Instructors Photos Wiki Editing Help | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
OUR TEAM
LAB 1 WRITE-UPInitial Machine TestingThe Original Design
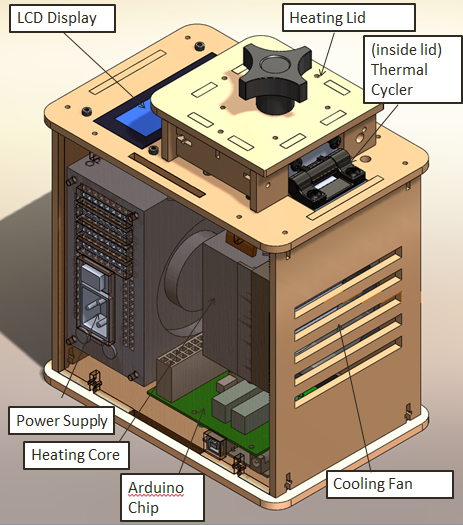
When we unplugged the lcd display wire(part 3) from the Arudnio chip(part 6), the screen turned off. Everything on the PCR was working fine expect there was no output on the display. When we unplugged the white wire that connects Arudino chip(part 6) to thermal cycler (part 2), the reading from the screen dropped to -40 degrees Celsius. We disconnected the wire multiple times and each time the screen displayed -40 degrees Celsius.
We ran a test run on 10/25/2012. For this test we placed some empty PCR tubes into the machine and ran a simple test program on the Open PCR software. After the simple test was over we noticed that the display screen on the Open PCR lid matched very closely with what was displayed on our computer screen. The agreement between our computer screen and our PCR display meant that our diagnostic test was a success.
ProtocolsPolymerase Chain Reaction Polymerase Chain Reaction Procedure: 2.)We labeled 8 empty PCR tubes. For the first sample we labeled the 3 DNA samples 1A, 1B and 1C. For the second sample we labeled the tubes 2A, 2B and 2C. For the positive and negative controls, we labeled the tubes + and - respectively. 3.)Using one pipette per sample, to avoid contamination, we transferred the PCR reaction mix we were given to the PCR tubes. 4.)We then placed the samples in the PCR machine 5.)We set our PCR program to three stages. Stage one: 1 cycle, 95 degree Celsius for 3 minutes. Stage 2: 35 cycles, 95 degrees Celsius for 30 seconds, 57 degrees Celsius for 30 seconds, 72 degrees Celsius. Stage three: 72 degrees Celsius for 3 minutes and then hold at 4 degree Celsius.
Fluorimeter Assembly
Fluorimeter Procedure: 2.)With the permanent marker we also labeled the Eppendrof tubes at the top, we had a total of 10 Eppendrof tubes labeled and 10 pipettes labeled. 3.)We transferred each sample separately into the Eppendorf tubes containing 400 ml of buffer. 4.)Using a specially labeled Eppendorf tube containing SYBR GREEN, with its own pippter, we placed two drops onto the first two center drops. 5.)Then using the sample we placed two drops on top of the SYBR GREEN solution drops 6.)Then we aligned the blue light to pass through the drop. 7.)Then the smartphone operator took a picture with the settings on the phone adjusted to inactive flash, iso to 800, white balance to auto, exposure to the highest setting and contrast to the lowest setting. 8.)This process was repeated for all samples 9.)After picture was taken it was given to the Image J software
Image J Procedure: 2.)Using the menu selection we used, image > color > split channels 3.) This created 3 files 4.)The we clicked menu bar to activate the oval selection. 5.)We drew an oval around our green drop image and then selected analyze > measure. 6.) We then repeated the oval process but for the area above the drop, to get the noise measurement.
Research and DevelopmentSpecific Cancer Marker Detection - The Underlying Technology In order to isolate and detect the cancer-causing gene, we essentially added a very specific primer that attaches to the cancer gene on the DNA. This Primer will not only allow for replication of the DNA, but more specifically, replication of the cancer gene in the DNA sample. The Open PCR machine then manipulates the temperature of the sample to facilitate the constant replication of the isolated DNA strands. We cycled the machine 30 times (the DNA was replicated 30 times) to be sure we had enough of the cancer DNA present in our solution. By understanding the mechanism of the Open PCR, we can intuitively understand how genes with specific diseases - such as cancer - are amplified. It is now necessary to learn how to identify which samples contain those replicated genes. The rs17879961 cancer-associated sequence in particular, can be identified within the DNA because of the single nucleotide variation - in this case a missense mutation - in its gene code. The mutation will yield a positive identification marker for cancer when the nucleotide cytosine is replaced by thymine in a very specific section of the DNA. Original Code: Mutated Code: (due to SNP (or mutation)) When considering scientific detection of the missense mutation itself, we have found that our DNA sequence rs17879961 is related to the condition of Breast and Colorectal Cancer. Therefore, in the case of PCR detection, the sequence for rs17879961 would be copied for by a primer. The primer starts the copying going forward and backward, with the primer that correlate to the strand of DNA; this primer identify the cancer sequence out of the DNA. Then, the patient would have that strand of DNA extracted and prepared for PCR amplification process. This preparation would include the use of primers, taq Polymerase, solution and dNTPs, and other necessary materials. This solution would be inserted into the PCR machine to be heated/cooled/heated. Eventually, the PCR process would yield multiple strands of the DNA that was initially placed and the SNP part that we had identified. A non-cancer DNA sequence would not produce a signal because the nucleotide variation where a primer would replicate DNA would be out of place; therefore, its process of DNA amplification would occur as normal. Only when we have a mutation, can we identify a signal from the DNA (assuming that we are attempting to detect a normal nucleotide sequence). As mentioned previously, we studied that the cancer marker, rs17879961, in the PCR experiment was correlated to the Breast and Colorectal cancer, but to completely understand the extent of this cancer's SNP to the development of cancer, we need to take a look at the statistics that not only follow Baye's Rule, but also provide useful information about the spread of this type of cancer. Based on conditional probabilities from a population diversity in Finland where the tested sample was 180 people, we found that the frequency of this cancer found in Finland was 7.8%. The genotype of this sequence of C/T in this population was 1.1% and the genotype of T/T was found to be 98.9%. For more infomation, visit http://www.ncbi.nlm.nih.gov/projects/SNP/snp_ref.cgi?rs=17879961.
Results
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||